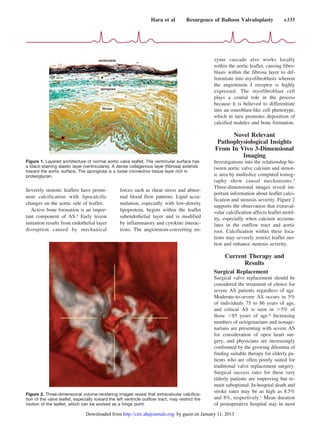
This document discusses percutaneous balloon aortic valvuloplasty (BAV) as a treatment for severe calcific aortic stenosis in high-risk elderly patients not suitable for surgical aortic valve replacement. It provides background on the pathophysiology and current treatment of aortic stenosis, including the limitations of surgical replacement in elderly populations. While BAV was previously abandoned due to high restenosis rates, the document argues that technical improvements and the growing population of very elderly patients make revisiting BAV worthwhile. It reviews the mechanisms and results of BAV, as well as guidelines for selecting patients for the procedure.