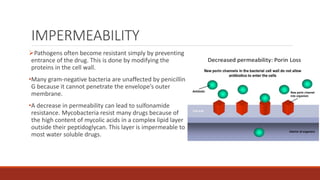
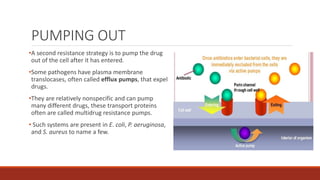
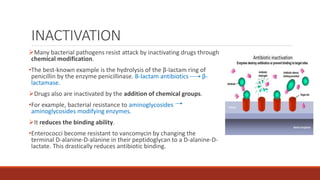
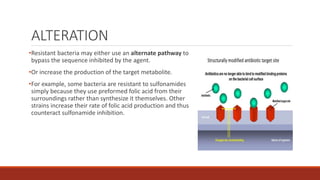
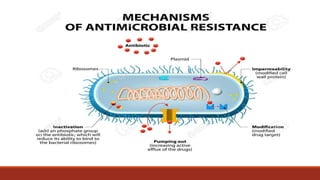
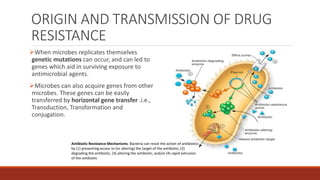
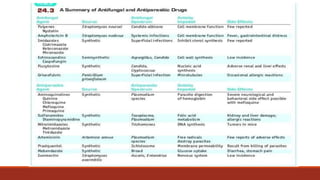
The document discusses antibiotic resistance, its definition, factors affecting it, and mechanisms through which bacteria develop resistance. It also highlights the importance of antibiotic susceptibility testing methods, such as the tube dilution method and disk diffusion method, to ensure effective treatment of bacterial infections. Preventive measures against antibiotic resistance include judicious use of antibiotics and following vaccination programs.