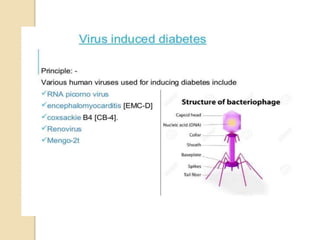
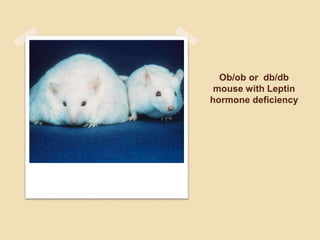
This document discusses various in vivo and in vitro models for studying anti-diabetic activity. It describes several chemical, viral, hormonal, and genetic methods for inducing diabetes in rodent models like mice and rats. These include alloxan and streptozotocin to chemically induce diabetes, viruses to infect pancreatic beta cells, growth hormone and corticosteroids to cause hormonal diabetes, and genetic mutations in leptin and leptin receptors. Spontaneous rodent models of obesity-related diabetes like ob/ob, db/db, ZDF, NZO, and OLETF rats are also covered. The document concludes with details of two in vitro assays - amylase inhibition and gl