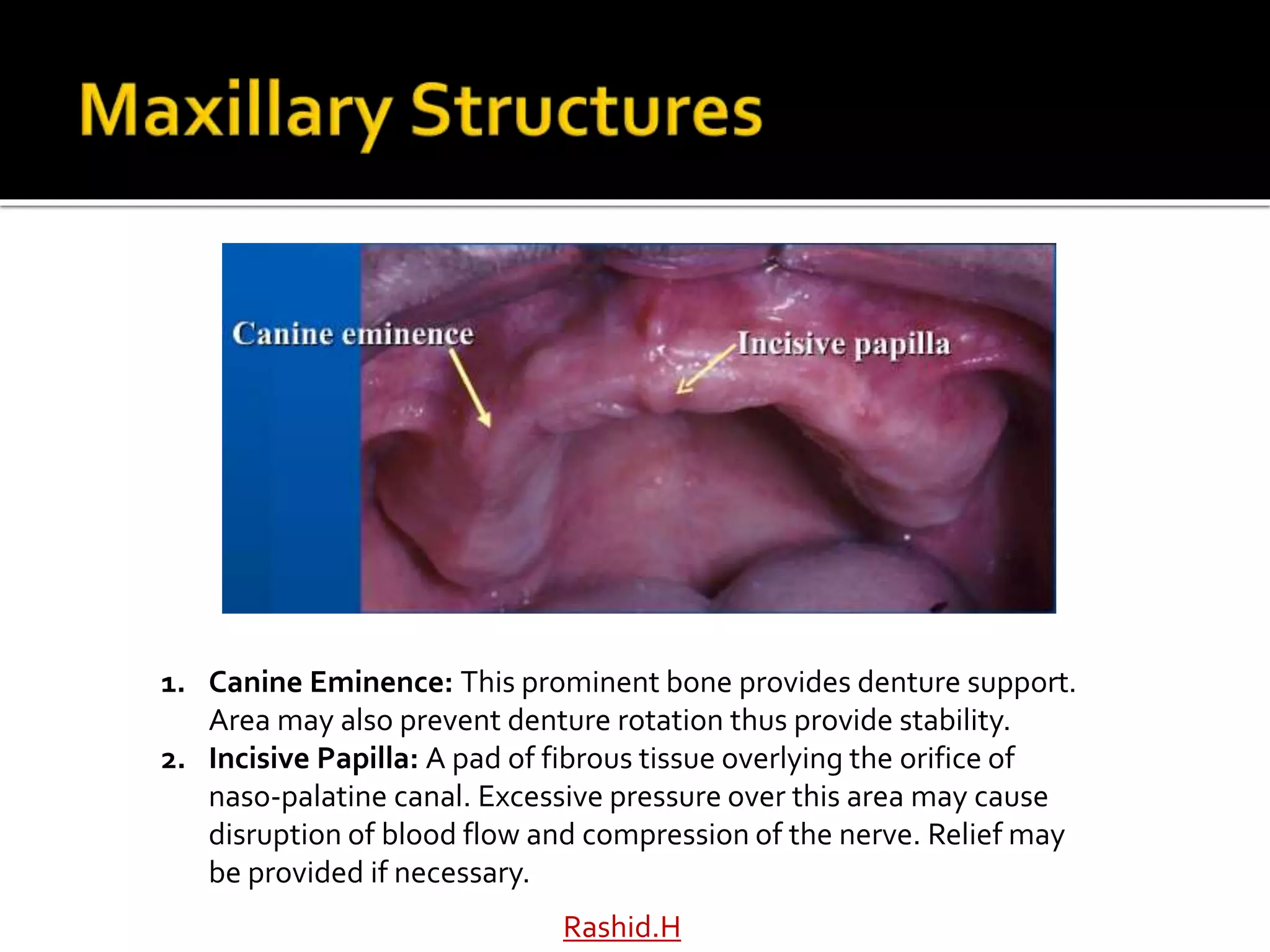
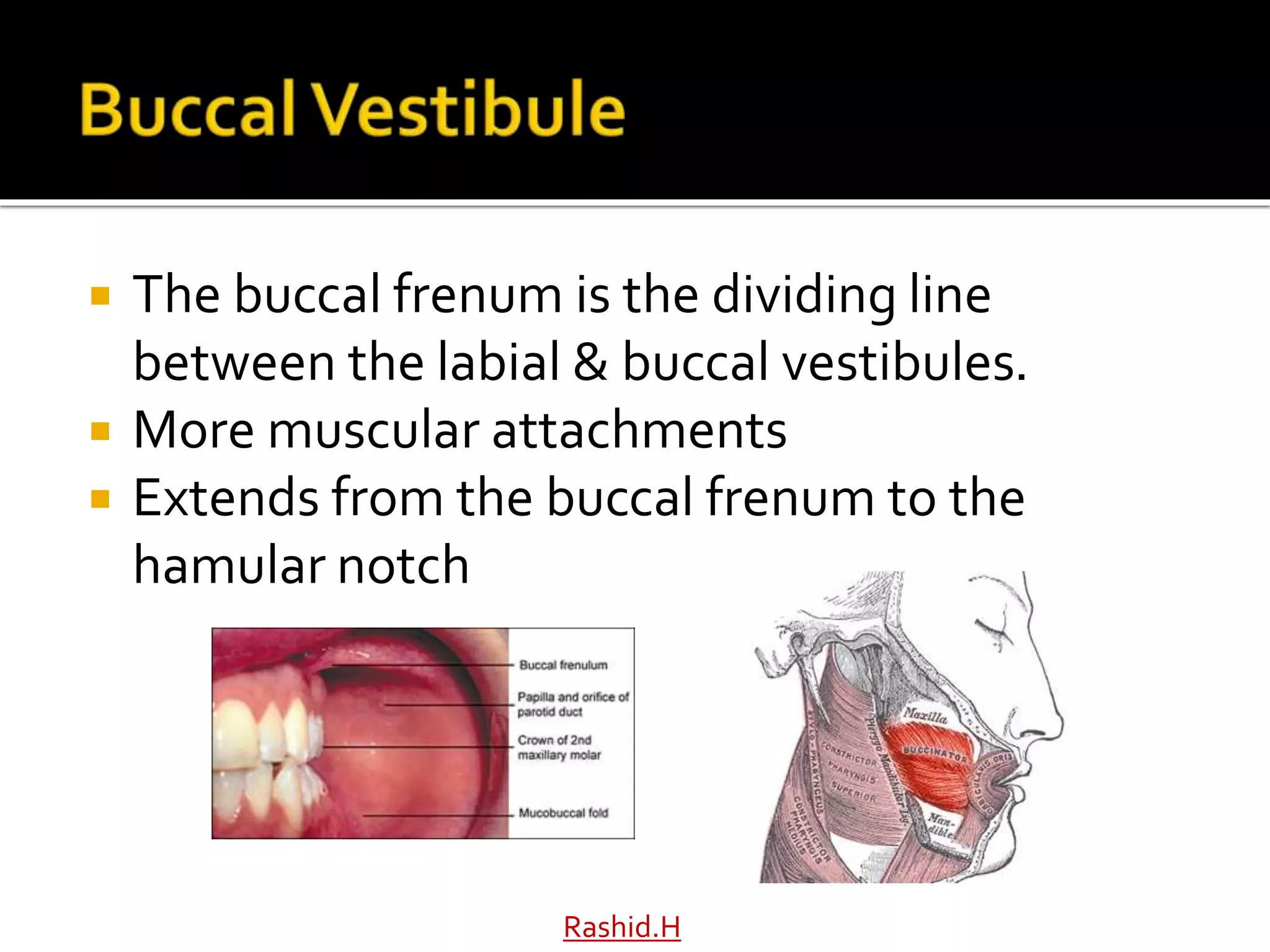
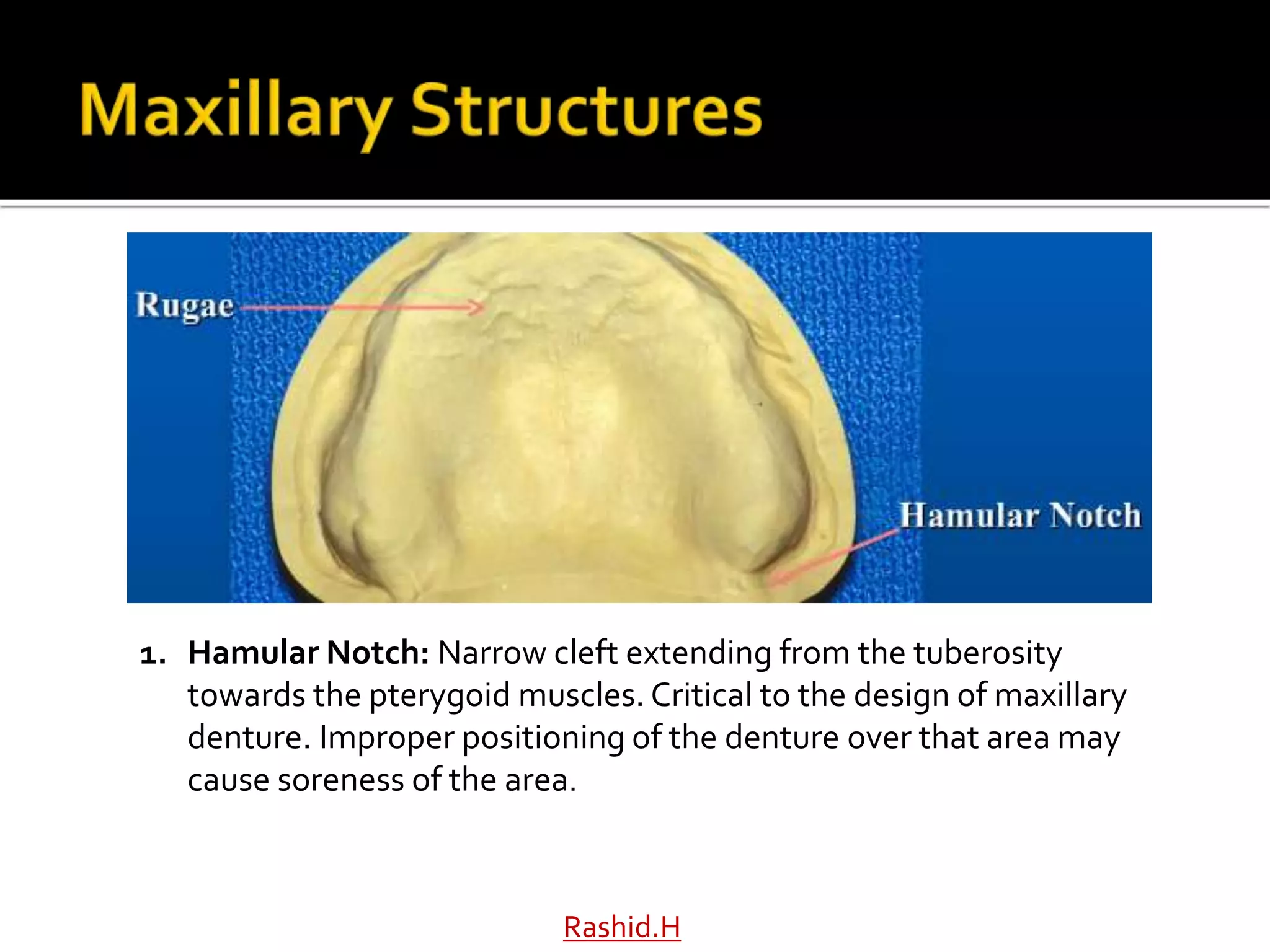
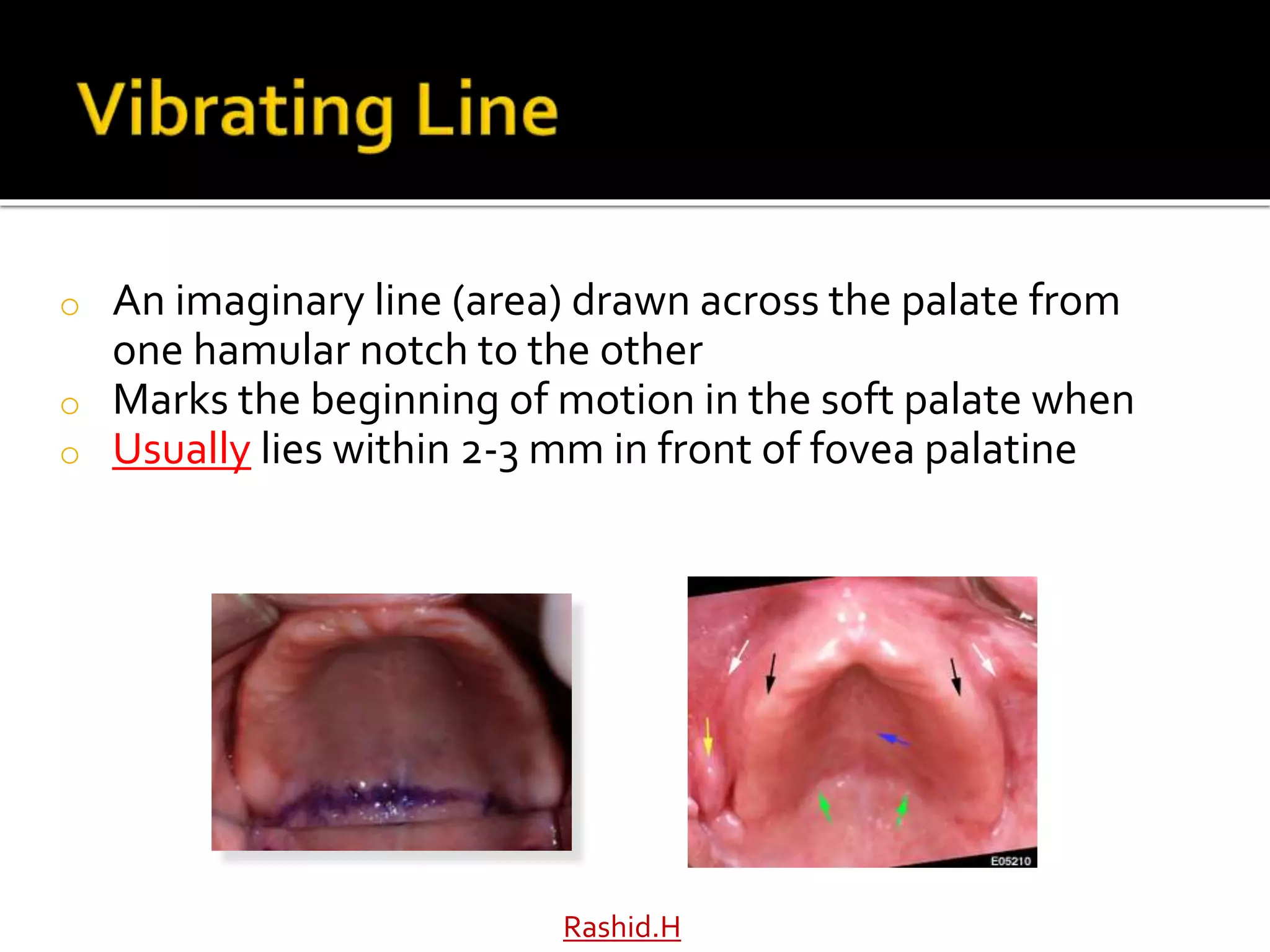
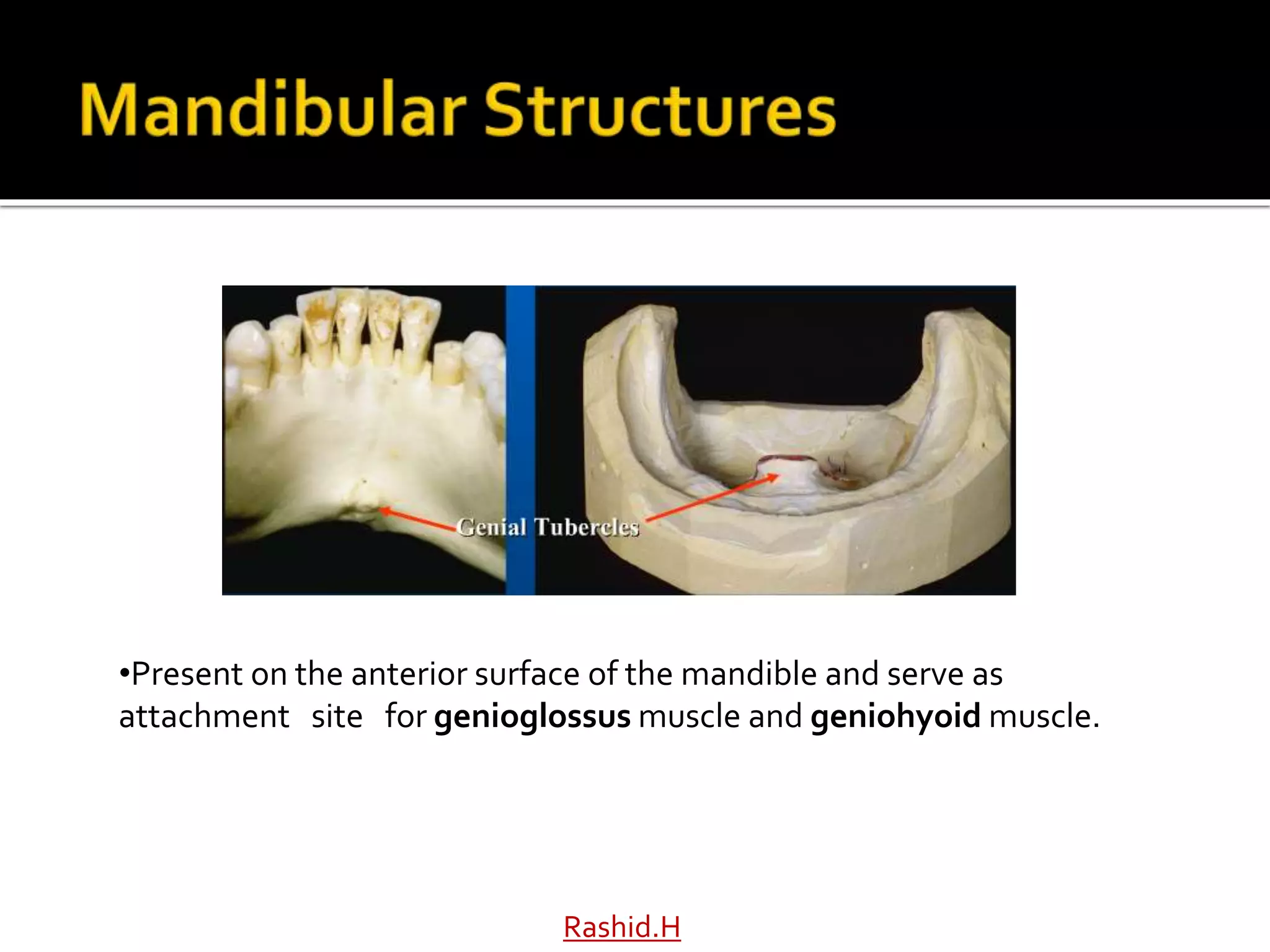
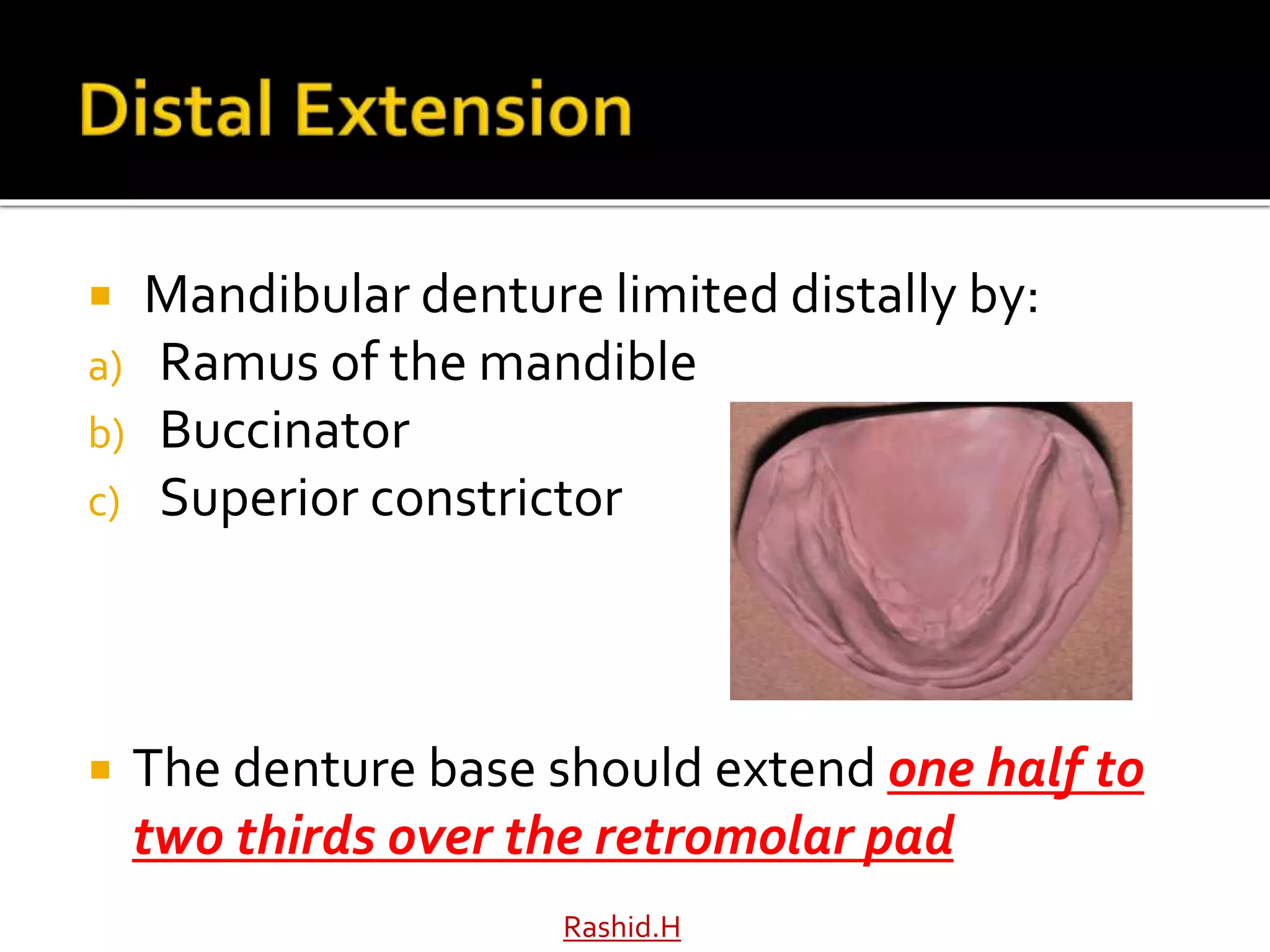
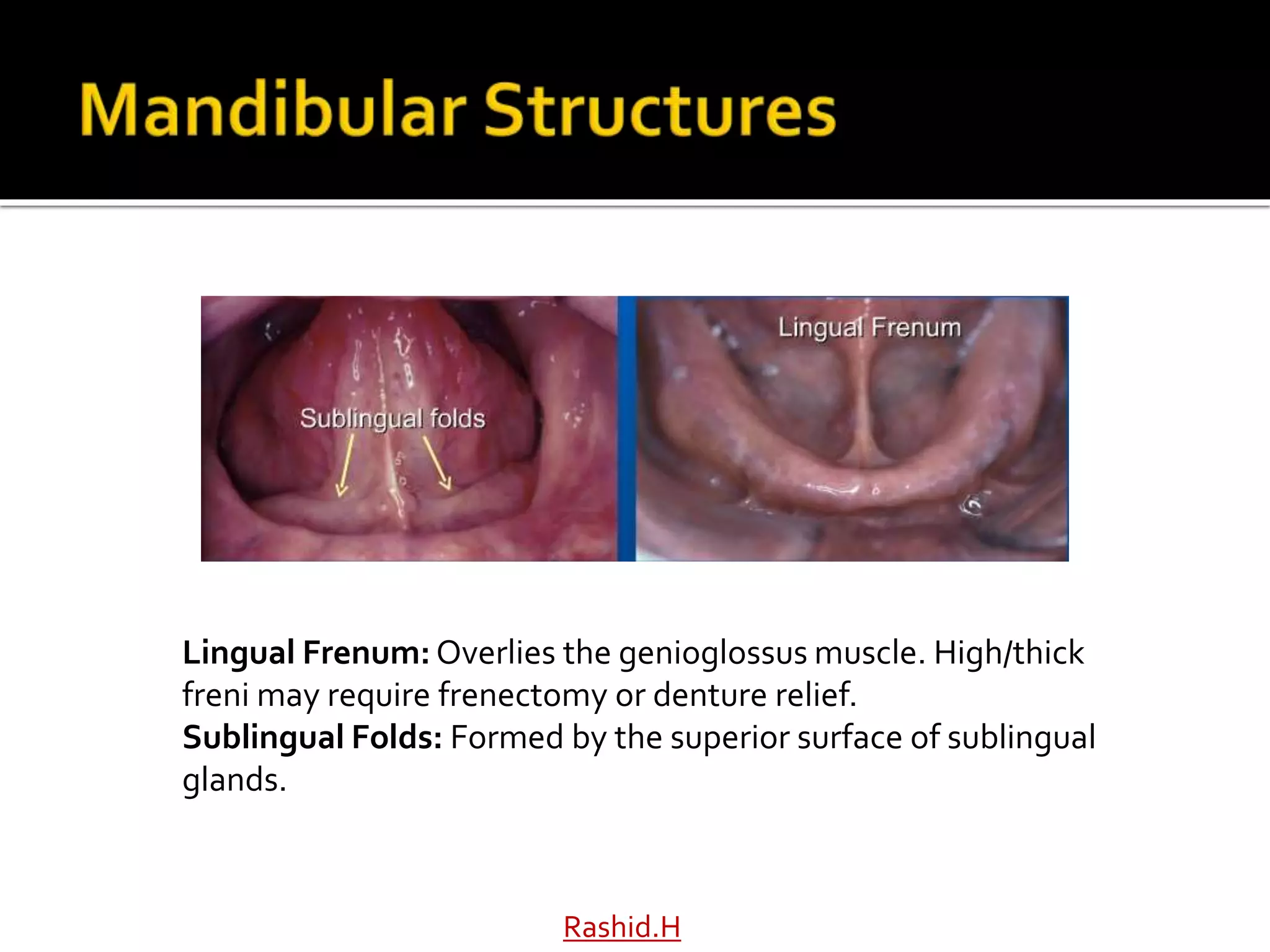
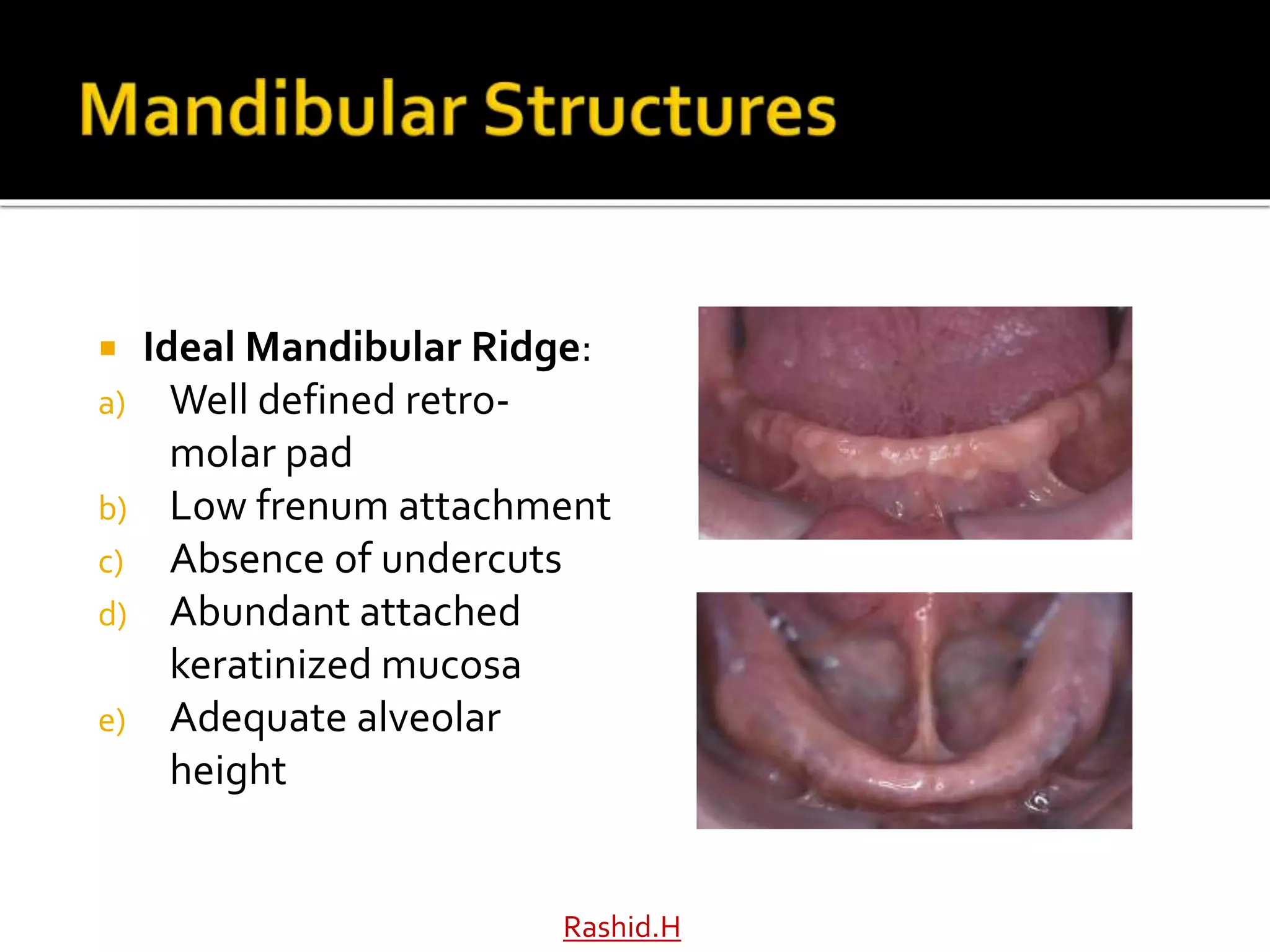
The document by Dr. Haroon Rashid Baloch discusses the importance of understanding the anatomy of denture-bearing surfaces for designing functional dentures. It details the relationship of anatomical structures that affect retention, stability, and support, particularly in the maxilla and mandible, and highlights key landmarks and muscle influences. The text emphasizes the need for careful consideration of anatomical features in denture fabrication to ensure optimal performance and comfort.