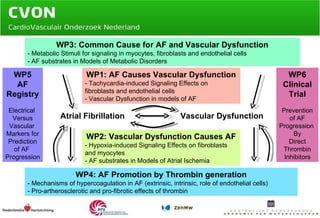
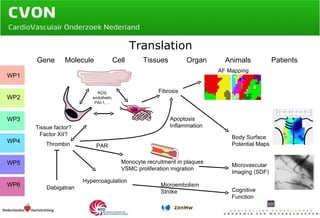
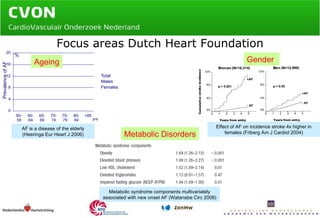
Atrial fibrillation (AF) is a serious health issue that increases morbidity and mortality, with a prevalence of 1-2% in the Netherlands. The document outlines a study involving a consortium of specialists aiming to explore the interconnected electrical and vascular mechanisms of AF to develop personalized therapies and reduce related complications. Key research questions focus on the molecular links between AF and vascular dysfunction, the impact of thrombosis, and aims to assess new treatments using thrombin inhibitors and evaluate risk factors in well-characterized patient cohorts.