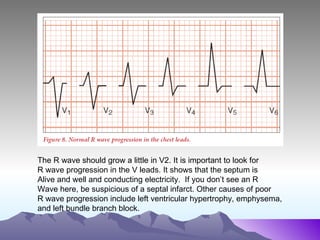
The document discusses the basics of interpreting a 12-lead ECG, including measuring heart rate and analyzing rhythm, intervals, axis deviation, and signs of hypertrophy. It covers normal cardiac anatomy and the two basic functions of the heart: circulating blood and adjusting blood flow in response to bodily factors. Key aspects are rate, rhythm, intervals, axis deviation, lead placement, and indicators of left ventricular, right ventricular, and bi-ventricular hypertrophy.