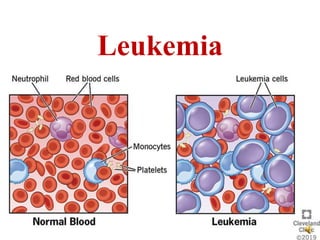
Leukemias
- 1. Leukemia
- 2. Introduction • Leukemia is a group of malignant disorders affecting the blood and blood-forming tissues in the bone marrow, lymphatic system, and spleen. • The word leukemia literally means “white blood” because it is a neoplastic proliferation of one type of blood cell, typically a leukocyte or white blood cell.
- 3. Contd. • Leukocytosis, an increased white blood cell count, is a normal response to infection, but when leukocytosis becomes chronic or progressively elevates without obvious cause, then it may indicate malignancy.
- 4. Risk Factors • Genetic predisposition, chromosomal changes, • Chemical agents (benzene) • Chemotherapeutic agents • Radiation, • Immuno compromised patients • Virus - only adult T cell leukemia is known to result from a virus, human T cell leukemia virus type 1 (HTLV-1).
- 5. Pathophysiology • Hematopoiesis, the process by which blood cells are formed, involves production of specific cells from stem cell precursors according to body needs. • In leukemia, a defect occurs in the myeloid or the lymphoid stem cell. • The most common feature of all types of leukemia is unregulated proliferation of leukocytes in the bone marrow.
- 6. Formation of blood cell
- 7. Classification Leukemia is classified by the type of white blood cells affected and by how quickly the disease progresses. Based on type of white blood cells affected • Lymphocytic leukemia (also known as lymphoid or lymphoblastic leukemia) develops in the white blood cells called lymphocytes • Myeloid leukemia (also known as myelogenous) may also start in white blood cells other than lymphocytes, as well as red blood cells and platelets in the bone marrow.
- 8. Based on disease progression Acute and chronic forms Acute forms: Acute leukemia is rapidly progressing and results in the accumulation of immature, functionless blood cells in the bone marrow. With this type of leukemia, cells reproduce and build up in the marrow, decreasing the marrow’s ability to produce enough healthy blood cells.
- 9. Contd.. • Chronic forms: Chronic leukemia progresses more slowly and results in the accumulation of relatively mature, but still abnormal, white blood cells.Chronic forms are rare in children.
- 10. Types of leukemia include: Type Description Acute lymphocytic leukemia (ALL) Progresses rapidly, replacing healthy cells that produce functional lymphocytes with leukemia cells that can't mature properly. Common in children. Acute myeloid leukemia (AML) Malignant, uncontrolled proliferation of an abnormally differentiated, myeloid stem cell results in high circulating numbers of immature blood cells and replacement of normal marrow by malignant cells. Common in adults and children. Chronic lymphocytic leukemia (CLL) Characterized by progressive accumulation of phenotypically mature malignant B lymphocytes. Common in adults. Chronic myeloid leukemia (CML) Overproduction of mature and immature granulocytes. Common in adults
- 14. Management Chemotherapy • The protocol for treatment varies depending on the type of leukemia. Generally, a combination of drugs is given as this approach is more effective than monotherapy. There are generally 3 stages to chemotherapy: • Induction • Consolidation • Maintenance
- 15. Induction • Patients are usually hospitalized for 4 to 6 weeks during initial treatment. • During this time, chemotherapy eradicates both leukemic cells and normal myeloid cells, so the person becomes severely neutropenic, anemic, and thrombocytopenic, putting patients at risk for severe infections and bleeding.
- 16. Consolidation • After the patient has recovered from the effects of induction, consolidation treatment is provided over 4 to 8 months, often with the same chemotherapeutic agents used during induction but at lower dosages in order to kill any remaining malignant cells.
- 17. Maintenance • Continued treatment may be provided for up to 3 years with some types of leukemia but with less intense chemotherapy in order to retain remission. • The patient is monitored closely for both progress and side effects with weekly blood counts.
- 18. Chemotherapeutic agents used • Vincristine • Doxorubicin • Methotrexate • Cyclophosphamide
- 19. Relapse • Sometimes people relapse after completing the 3 stages of chemotherapy. When that occurs, re-induction may be carried out, especially with children, usually using adifferent protocol of drugs.
- 20. Other treatments • Intrathecal chemotherapy is administered into the spinal fluid for treatment of infiltration of the central nervous system. • Radiation to the brain may be indicated in addition to intrathecal chemotherapy with severe disease, especially in children when infiltration poses danger to brain development. • Bone marrow transplant or peripheral blood stem cell transplant with donor stem cells or the patient’s stem cells. • Blood Transfusion/Platelet transfusion
- 21. Nursing management Nursing Diagnosis • Risk for Infection • Risk for Deficient Fluid Volume • Acute Pain • Activity Intolerance • Deficient Knowledge
