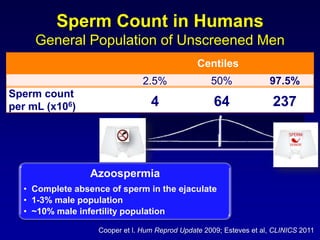
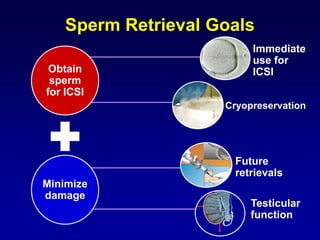
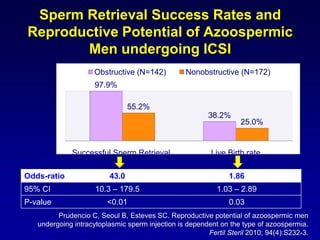
1. The document discusses sperm retrieval techniques for azoospermic men seeking fertility.
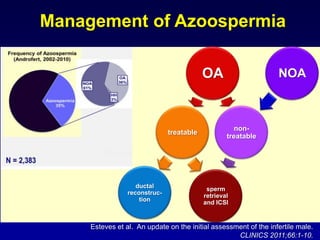
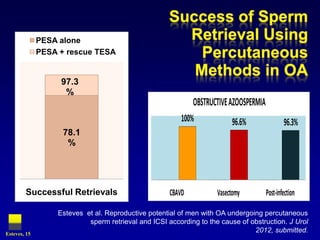
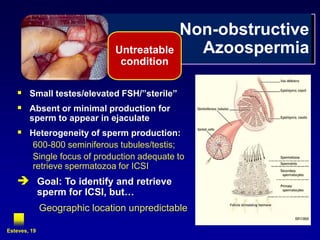
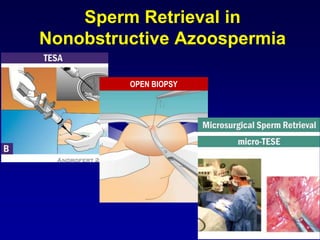
2. The optimal sperm retrieval method depends on whether the azoospermia is obstructive or non-obstructive.
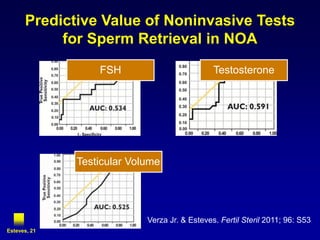
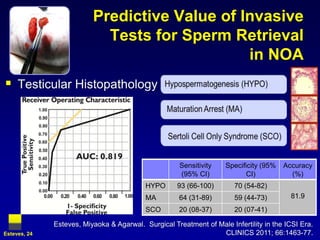
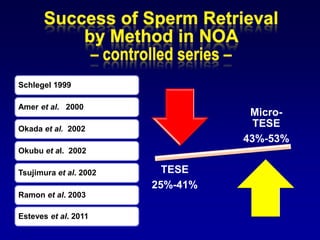
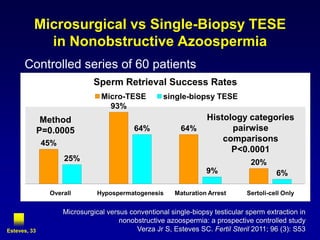
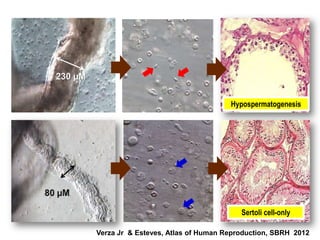
3. Microsurgical testicular sperm extraction (micro-TESE) has higher success rates than conventional testicular sperm extraction for non-obstructive azoospermia, especially for men with more severe testicular failure.