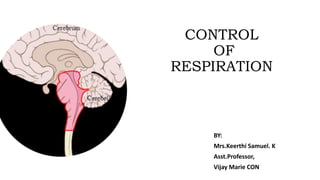
Respiratory centers
- 2. INTRODUCTION • At rest about 200ml of oxygen is used each minute by our body. • During strenuous breathing oxygen use typically increases 15-20 fold in a normal healthy adult.
- 3. RESPIRATORY CENTER • The size of thorax is altered by action of respiratory muscles which contract as a result of nerve impulses transmitted to them from the centers in the brain and relax in the absence of nerve impulses. • RESPIRATORY CENTER: Nerve impulses are sent from clusters of neurons located bilaterally in MEDULLA OBLONGATA and PONS. • THE THREE AREARS OF RESPIRATORY CENTER ARE: MEDULLARY RHYTHMICITY AREA PNEUMOTAXIC AREA APNEUSTIC AREA
- 4. 1.MEDULLARY RHYTHMICITY AREA • FUNCTION: TO CONTROL THE RHYTHM OF RESPIRATION • There are two areas: 1.INSPIRATORY 2. EXPIRATORY • During quiet breathing – Inhalation lasts about 2 seconds Exhalation lasts for 3 seconds • Nerve impulses will be generated in inspiratory area to establish the rhythm • Activation of inspiratory area • Generation of nerve impulse for 2 sec • These impulses propagate to ext. Intercostals via • INTERCOSTAL NERVES- EIM • PHRENIC NERVES-DIAPHRAGM
- 5. The cycle repeats Elastic recoil of lungs and thoracic wall With no impulses ,the diaphragm and EIM reax for 3seconds Inspiratory area becomes inactive inactive after 2sec and the nerve impulses cease As the muscles contract INHALATION occurs. 1.MEDULLARY RHYTHMICITY AREA Neurons of the Exp.area remains inactive during quiet breathing but during forceful breathing impulses from Insp.area activates the Exp.area
- 6. 2. PNEUMOTAXIC AREA Seen in upper pons which transmits inhibitory impulses to inspiratory area The major function of this area is to turnoff the inspiratory area before lungs become too full of air. In other words the impulses shorten the duration of inhalation. When this area is active , breathing is more rapid FUNCTION: CO-ORDICATES THE TRANSITION BETWEEN INHALATION AND EXHALATION
- 7. 2. APNEUSTIC AREA Present in LOWER PONS Stimulates and activates the inspiratory area during inhalation Results in long deep inhalation FUNCTION: CO-ORDICATES THE TRANSITION BETWEEN INHALATION AND EXHALATION
- 9. CHEMORECEPTOR REGULATION OF RESPIRATORY CENTER • The respiratory system functions to maintain proper levels of co2 and o2 and is very responsive to the changes in levels of these gases in the body fluids. • The sensory neurons that responds to these chemicals are called as CHEMORECEPTORS • They maintain levels of co2, H+ and O2. • This provides input to the respiratory center. • There are two types of chemoreceptors: • CENTRAL CHEMORECEPTORS • PERIPHERAL CHEMORECEPTORS
- 10. CHEMORECPTORS CONTINUED…. CENTRAL CHEMORECEPTORS • Located near Medulla Oblongata in CNS. • Respond to changes in both H+,Pco2or both in CSF PERIPHERAL CHEMORECEPTORS • Located in aortic bodies(clusters of chemoreceptors in he wall of arch of aorta) and carotid bodies(present in carotid arteries) • They respond to the changes in Po2,H+ and Pco2 in blood.
- 11. CHEMORECEPTOR REGULATION • Normal Pco2 in blood is 40mmHg , when increased it is called HYPERCAPNIA. • During hypercapnia • In addition the ONLY peripheral CR respond to deficiency of O2. Central CR are stimulated due to increased H+ Peripheral CR are stimulated due to increase in H+ and Pco2
- 12. REGULATION OF RESPIRATORY CENTER POSITIVE FEEDBACK When Pao2 falls from normal to 100 mmHg but is still above 50mmhg----- PR gets stimulated and inspiratory area in chemoreceptors gets deactivated. Decreased impulses to the respiratory ,muscles of inhalation. As breathing rate falls more and more PAo2 falls more and more leading to fatal result. NEGATIVE FEEDBACK The CR participate in negative feedback regulate levels of CO2,O2 and H+. Due to increase in PCo2, decreased PH, decreased Po2. Central and peripheral chemoreceptors stimulates inspiratory area to become active. Rate and depth of breathing increases--- HYPERVENTILATION. Allows inhalation of more O2 and exhalation of Co2. Until Pao2 and H+ are lowered to normal.
