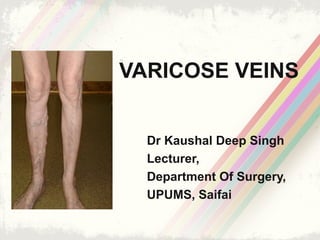
Varicose veins
- 1. VARICOSE VEINS Dr Kaushal Deep Singh Lecturer, Department Of Surgery, UPUMS, Saifai
- 2. Venous Anatomy of Lower Limbs • Superficial venous system • Deep venous system • Perforator veins
- 3. The Long Saphenous VeinThe Long Saphenous Vein The longest vein in the bodyThe longest vein in the body Surface AnatomySurface Anatomy •1 cm anterior to the medial malleolus •One hand breadth posterior to the medial aspect of the patella •Ends on the anteromedial side of the femoral vein 3.5 cm below & lateral to the pubic tubercle It receives the following tributaries near its termination: •Superficial & deep external pudendal v. •Superficial circumflex iliac v. •Superficial inferior epigastric v.
- 4. The Short Saphenous VeinThe Short Saphenous Vein AnatomyAnatomy • Behind the lateral malleolus • Pierces the deep fascia before it enters the popliteal vein • Variably terminates above or below the popliteal fossa • Communicates with the long saphenous vein by several channels
- 5. Venous valves • Venous valves are abundant in the distal lower extremity and number of valves decreases proximally, with no valves in superior and inferior vena cava • Delicate structures • Prevent reverse flow in the veins
- 6. Perforator Veins • Connect superficial to deep veins at various levels. • Travel from superficial fascia through an opening in the deep fascia before entering the deep veins. • Direction of blood flow - from superficial to deep veins. • Guarded by valves so that the flow is unidirectional, i.e. Towards deep veins. • Reversal of flow occurs due to incompetence of perforators which leads to varicose veins
- 7. Main sites of superficial to deep venous communicationMain sites of superficial to deep venous communication Medial malleolus Sapheno-femoral junction Mid thigh perforator (Hunter’s canal) Medial calf perforators Just below Just above 10 cm above Just below the knee MayMay oror KusterKuster ankleankle perforatorsperforators CockettCockett lowerlower legleg perforatorsperforators(3)(3) BoydBoyd gastrocnemiusgastrocnemius perforatorsperforators Distal ThighDistal Thigh PerforatorPerforator (Dodd(Dodd perforator )perforator )
- 8. Venous returnVenous return The heart pump maintaining a pressure gradient across the veins Gravity Pooling in dependent limbs may reduce cardiac output by 2 L/min & may cause fainting Venomotor tone Under control of sympathetic system [Upright position -- dependant pooling – dec. cardiac output -- inc. sympathetic discharge -- inc. venous tone -- inc. venous return.] With dependencyWith dependency This is counter acted by:This is counter acted by: With calf muscle contraction inWith calf muscle contraction in walkingwalking Calf muscle contraction Blood is pushed upwards and prevented from retrograde flow by competent venous valves
- 9. CompetentCompetent Veno-muscularVeno-muscular Pump is composed of:Pump is composed of: 1. Superficial & deep veins1. Superficial & deep veins with competent valves.with competent valves. 2. Competent perforating2. Competent perforating veins communicating theveins communicating the deep & superficial systemsdeep & superficial systems 3. Powerful lower limb3. Powerful lower limb muscles.muscles.
- 10. Varicose Veins • Long, tortuous and permanently dilated veins of the superficial venous system due to the pooling of blood in the lower extremities. • Risk factors – Gender - Female sex – Prolonged standing – Raised intra abdominal pressure – Increased progesterone – High heels – Genetics – Age – Pregnancy – Overweight and obesity
- 11. Classification Of Varicose Veins
- 14. Pathogenesis of Varicose Veins Any risk factor/cause ↓ ↑ced venous pressure ↓ Dilation of veins ↓ Valves stretched ↓ Incompetent valve ↓ Reverse blood flow ↓ Calf muscles fail to pump blood ↓ Venous distention
- 16. Clincial Features • Dragging pain, postural discomfort • Heaviness in the legs • Night time cramps • Oedema, itching • Discolouration • Ulceration
- 17. Cause Of Pain In Varicose Veins • Chronic venous hypertension • Anoxia • Hyperviscosity of red cells • Platelet aggregation • Capillary functional disorder • Altered cutaneous microcirculation
- 18. The patient should be standingClinical ExaminationClinical Examination Look for:Look for: The extent and distribution of VVThe extent and distribution of VV Antro-lat. tributary of LSV Short saphenous VV Communicating vein varicosity Long saphenous VV
- 19. Clinical Signs
- 20. Brodie –Trendelenburg test Test for incompetenceTest for incompetence Empty the veins & apply a mid thigh tourniquet Let the patient stand If the veins remain empty, but fill after removal of tourniquet, the incompetence must be above the tourniquet If the veins fill before removal of tourniquet, the incompetence must be below the tourniquet
- 21. Perthes’ walking testPerthes’ walking test Place a tourniquet around the thigh while the patient is standing (note that the vv are full) Let the patient walk in place If the veins empty with walking, then the tourniquet is preventing superficial reflux from an incompetent valve above, while deep veins are patent with intact valves.
- 22. Investigations In Varicose Veins • Identify the existence, site & degree of venous reflux. • Confirm deep venous patency to rule out DVT
- 23. Identification of venous reflux:Identification of venous reflux: 1.1. Doppler Ultrasound:Doppler Ultrasound: portable bedsideportable bedside examinationexamination It is accurate in detectingIt is accurate in detecting sapheno-femoralsapheno-femoral reflux inreflux in the groin.the groin. •Hold the Doppler probe on the groin and detect the venous signal •Squeeze the calf. This will augment the signal •If the SFJ is incompetent, you will hear a biphasic signal due to retrograde flow
- 24. Identification of venous reflux:Identification of venous reflux: Coloured Duplex Ultrasonography:Coloured Duplex Ultrasonography: 1. Doppler combined with B mode ultrasound 2. Functional as well as anatomical information 3. Visually demonstrates venous reflux into the superficial and deep veins. 4. The degree of venous reflux can be assessed. (Dynamic Study) 1. DVT can be ruled out. 2. Can detect incompetent perforators. Uniphasic signal – normal Biphasic signal – reversal flow
- 25. Identification of venousIdentification of venous reflux:reflux: Magnetic Resonance Venography Photoplethysmography Descending venography
- 26. Confirming Deep VenousConfirming Deep Venous Patency:Patency: As in patients with suspected post-phlebitic syndrome (chronic complication of maltreated DVT) 1. Duplex Ultrasound1. Duplex Ultrasound 2. Ascending2. Ascending VenographyVenography
- 28. Physiologic Testing of Venous Function • Venous refilling time • Maximum venous outflow • Calf muscle pump ejection fraction
- 29. Complications • Hemorrhage • Pigmentation/ eczema • Periostitis • Venous ulcer • Lipodermatosclerosis • Talipes equinovarus • DVT • Recurrent thrombophlebitis • Venous thromboembolism
- 31. • Preventive measures C1 • Medical Measures C1-3 • Surgical/Ablative measures C3-6
- 32. Treatment of Venous Disorders Based on Pathophysiology
- 33. Management of Varicose Veins Minor VVMinor VV Supportive stocking Injection sclerotherapy, compression Trunk VV (long or short saphenous) with incompetenceTrunk VV (long or short saphenous) with incompetence Endovenous Ablation (Radiofrequency/Laser) >> Sapheno-femoral / sapheno-popliteal ligation with stripping of the long or short saphenous vein. (no need to strip the long saph. In the leg) BranchBranch VaricositiesVaricosities Avulsion/ligation via multiple stabs IncompetentIncompetent perforatorsperforators (detected by(detected by Duplex)Duplex) SEPS >> Individual ligation
- 34. Preventive Measures • Avoid prolonged sitting & standing • Elevation of limbs • Weight reduction
- 35. Medical Management 1. Compression Therapy – first-line therapy for symptomatic varicose veins (prevention, treatment & post-op.) •Elastic crepe bandage – 30-40mm Hg •Unna boot – Non-elastic compression – Zinc oxide, calamine and glycerine – Dressing changed once in a week – Infection should not be there •Graded compression stockings – Reduce ambulatory venous pressure – Trans capillary leakage – Improve cutaneous micro circulation
- 36. Medical Management contd… 2. Oral medication •No evidence for monotherapy (only in addition effect on ulcer healing) •Calcium dobesilate – Improves lymph flow, reduce edema •Daflon, Pentoxifylline (Trental), Aspirin
- 37. Medical Management (contd)… Рhlebo/Venotropic drugs a)Diosmin – • Semisynthetic flavonoid (modifies hesperidin) • Venotonic, lymphotonic, Improves microcirculation • Improves edema, dermatitis, venous ulcers a)Hesperidin – • Flavonoid • Venotonic • Used along with diosmin a)Rutoside – • Glycoside • Inhibits platelet aggregation, decreases capillary permeability, anti-inflammatory • Less certain role
- 38. Medical Management (contd)… d) Sulodexide – • Highly purified glycosaminoglycan consisting of 80% low- molecular-weight heparin and 20% dermatan sulfate • Anti-inflammatory, endothelial-protective • Improves venous ulcers e) Micronized purified flavonoid fraction (MPFF) (Daflon) – • 90% micronized diosmin and 10% flavonoids as hesperidin • Veno and lymphotonic, decreases capillary permeability, anti-inflammatory • Improves venous ulcers, reduces edema • Horse chestnut seed extract
- 39. Exercise •Graded exercise programs rehabilitate the muscle pump and improve the symptoms of CVI. •Structured exercises re-establishes calf muscle pump function. Medical Management (contd)…
- 40. Sclerotherapy • For obliterating telangiectases, reticular veins, varicose veins, and saphenous segments with reflux. • Complete sclerosis of the venous wall. • Indications – Uncomplicated perforator incompetence – Smaller varices – Recurrent varices – Isolated varices – Aged/unfit patients
- 41. Sclerotherapy (contd.)… • Sclerosants used are – Hypertonic solution of sodium chloride (23.4%) – Sodium tetradecyl sulphate – Sodium morrhuate – Ethanolamine oleate – Polidocanol – Glycerin • Mechanism of action – Aseptic inflammation – Perivenous fibrosis – Endothelial damage – Obliteration by intimal approximation
- 42. Sclerotherapy (contd.)… • Sclerotherapy with polidocanol foam under duplex ultrasound guidance has become standard in the treatment of – • Intracutaneous telangiectases • Subcutaneous varicose veins • Transfascial perforating veins • Venous malformations • Complication - Hyperpigmentation of the surrounding skin from deposition of hemosiderin.
- 45. Surgical Management • Trendelenberg’s procedure – Juxtafemoral flush ligation of long saphenous vein Flush ligation of tibutaries Superficial circumflex iliac Superficial external pudendal Superficial inferior epigastric Deep external pudendal
- 46. Surgical Management Contd… • Stripping of long saphenous vein • Upto knee joint • Myer’s stripper • Complications – Saphenous nerve injury – Hematoma – Infection
- 47. Surgical Management Contd… • Perforator incompetence – Subfascial ligation of perforators – Linton’s method – Stab avulsion method
- 48. SEPS • Subfascial endoscopic perforator surgery • Minimally invasive method
- 49. Endovenous Laser Ablation - EVLA • US guidance LSV canulated above knee jt • Guide wire passed beyond SFJ • Tip is placed 1cm distal to SF junction • Laser fibre inserted upto the catheter • Diode laser used for firing
- 50. EVLA Cotd… • Office based procedure • Done under local anesthesia • One needle puncture at the level of the knee • Takes about 1 hour • Patient resumes normal activity same day
- 51. • Skin grafting can be put on a non infected granulating skin defect of a venous ulcer
- 52. • Major complications following VV surgery are relatively rare. • Up to 20% morbidity – Infection – Hematoma – Pain – Nerve damage • Saphenous nerve (LSV surgery) • Sural, peroneal nerve (SSV surgery) – Lymphatic leak - Venous thrombosis - Vascular injury – Recurrence
- 53. Recurrent Varicose Veins A. Are more common if the long saphenous vein is not tied flush in the first procedure B. Are more common if incompetent perforators are not identified at the first procedure C. Should be investigated by duplex ultrasound D. Can be treated with sclerotherapy
- 54. THANK YOU
Editor's Notes
- Reduce pain, swelling, skin pigmentation, activity and general well-being.
- Fortunately, major complications following VV surgery are relatively rare. However, up to 20% of patients may suffer some form of minor morbidity, such as hematoma, lymphatic leak, pain, saphenous neuritis, and venous thrombosis. In the U.K., VV surgery is the commonest cause of litigation against general and vascular surgeons. This not a field for the unsupervised, inexperienced surgeon and it behooves surgeons who undertake VV surgery to carefully audit their management, techniques, and outcomes. Surgery is for recurrence in 20% of patients.
