A Closer Look at the Atopic Dermatitis Patient Journey: Effective Management Approaches Across the Age and Disease Spectrum
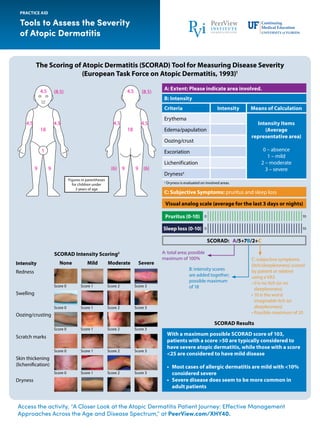
- 1. Access the activity, “A Closer Look at the Atopic Dermatitis Patient Journey: Effective Management Approaches Across the Age and Disease Spectrum,” at PeerView.com/XHY40. Tools to Assess the Severity of Atopic Dermatitis PRACTICE AID The Scoring of Atopic Dermatitis (SCORAD) Tool for Measuring Disease Severity (European Task Force on Atopic Dermatitis, 1993)1 A: Extent: Please indicate area involved. B: Intensity Criteria Intensity Means of Calculation Erythema Intensity Items (Average representative area) 0 – absence 1 – mild 2 – moderate 3 – severe Edema/papulation Oozing/crust Excoriation Lichenification Drynessa a Dryness is evaluated on involved areas. C: Subjective Symptoms: pruritus and sleep loss Visual analog scale (average for the last 3 days or nights) SCORAD: A/5+7B/2+C SCORAD Results SCORAD Intensity Scoring2 Pruritus (0-10) Sleep loss (0-10) A: total area; possible maximum of 100% B: intensity scores are added together; possible maximum of 18 C: subjective symptoms (itch/sleeplessness) scored by patient or relative using a VAS • 0 is no itch (or no sleeplessness) • 10 is the worst imaginable itch (or sleeplessness) • Possible maximum of 20 With a maximum possible SCORAD score of 103, patients with a score >50 are typically considered to have severe atopic dermatitis, while those with a score <25 are considered to have mild disease • Most cases of allergic dermatitis are mild with <10% considered severe • Severe disease does seem to be more common in adult patients 0 0 10 10 Figures in parentheses for children under 2 years of age Intensity Redness Swelling Oozing/crusting Scratch marks Skin thickening (lichenification) Dryness None Mild Moderate Severe Score 0 Score 0 Score 0 Score 0 Score 0 Score 1 Score 2 Score 3 Score 1 Score 2 Score 3 Score 1 Score 2 Score 3 Score 1 Score 2 Score 3 Score 1 Score 2 Score 3
- 2. Access the activity, “A Closer Look at the Atopic Dermatitis Patient Journey: Effective Management Approaches Across the Age and Disease Spectrum,” at PeerView.com/XHY40. Tools to Assess the Severity of Atopic Dermatitis PRACTICE AID 1. European Task Force on Atopic Dermatitis. Dermatology. 1993;186:23-31. 2. https://www.dermnetnz.org/topics/scorad/. Accessed October 3, 2019. 3. https://www.eczemacouncil.org/wp-content/ uploads/2018/02/Validated-Investigator-Global-Assessment-Scale_vIGA-AD_2017.pdf. Accessed October 3, 2019. 4. https://www.nice.org.uk/guidance/cg57/resources/atopic-eczema-in-under-12s- diagnosis-and-management-975512529349. Accessed October 3, 2019. Validated Investigator Global Assessment Scale for Atopic Dermatitis3 Score Morphological Description 0 – Clear • No inflammatory signs of atopic dermatitis (no erythema, no induration/ papulation, no lichenification, no oozing/crusting) • Postinflammatory hyperpigmentation and/or hypopigmentation may be present 1 – Almost clear • Barely perceptible erythema, barely perceptible induration/papulation, and/or minimal lichenification • No oozing or crusting 2 – Mild • Slight but definite erythema (pink), slight but definite induration/papulation, and/or slight but definite lichenification • No oozing or crusting 3 – Moderate • Clearly perceptible erythema (dull red), clearly perceptible induration/papulation, and/or clearly perceptible lichenification • Oozing and crusting may be present 4 – Severe • Marked erythema (deep or bright red), marked induration/papulation, and/or marked lichenification • Disease is widespread in extent • Oozing or crusting may be present Visual Assessment of Severity Proposed by the United Kingdom National Institute for Health and Care Excellence4 Mild • Areas of dry skin, infrequent itching (with or without small areas of redness) • Little impact on everyday activities, sleep, and psychosocial well-being Moderate • Areas of dry skin, frequent itching, redness (with or without excoriation and localized skin thickening) • Moderate impact on everyday activities and psychosocial well-being; frequently disturbed sleep Severe • Widespread areas of dry skin, incessant itching, redness (with or without excoriation, extensive skin thickening, bleeding, oozing, cracking, and alteration of pigmentation) • Severe limitation of everyday activities and psychosocial functioning, nightly loss of sleep
- 3. Atopic Dermatitis Yardstick: A Step-Care Approach to Patient Management1 AD: atopic dermatitis; TCI: topical calcineurin inhibitor; TCS: topical corticosteroids. 1. Boguniewicz M et al. Ann Allergy Asthma Immunol. 2018;120:10-22 PRACTICE AID Access the activity, “A Closer Look at the Atopic Dermatitis Patient Journey: Effective Management Approaches Across the Age and Disease Spectrum,” at PeerView.com/XHY40. Maintenance Treatment Acute Treatment Nonlesional Mild Moderate Severe BASIC MANAGEMENT Apply TCS to Inflamed Skin Low- to medium-potency TCS 2x daily for 3-7 days beyond clearance (Consider TCI, crisaborole) BASIC MANAGEMENT BASIC MANAGEMENT + TOPICAL ANTI-INFLAMMATORY MEDICATION Apply TCS to Inflamed Skin Medium- to high-potency TCS 2x daily for 3-7 days beyond clearance (Consider TCI, crisaborole) Apply on areas of previous/ potential symptoms (AKA flare) BASIC MANAGEMENT + REFERRAL TO AD SPECIALIST 1. Skin care • Moisturizer, liberal and frequent (choice per patient preference) • Warm baths/showers using nonsoap cleansers, usually once daily and followed by moisturizer (even on clear areas) 2. Trigger avoidance • Proven allergens and common irritants • Consider comorbidities 1. Skin care • Moisturizer, liberal and frequent (choice per patient preference) • Warm baths/showers using nonsoap cleansers, usually once daily and followed by moisturizer (even on clear areas) 2. Antiseptic measures • Dilute bleach bath (or equivalent) ≤2x/week according to severity (especially with recurrent infections) • Antibiotics, if needed 3. Trigger avoidance • Proven allergens and common irritants • Consider comorbidities Maintenance TCS • Low-potency 1-2x daily (including face) • Medium potency 1-2x weekly (except face) Or Maintenance TCI (pimecrolimus, tacrolimus) • 1-2x daily • 2-3x weekly (not an indicated dosage) Or Crisaborole 2% • 2x daily Phototherapy Dupilumab Systemic Immunosuppressants • Cyclosporine A • Methotrexate • Mycophenolate mofetil • Azathioprine • Corticosteroids Consider acute treatment for some patients to help gain control • Wet wrap therapy • Short-term hospitalization If not resolved in 7 days, consider • Non-adherence • Infection • Misdiagnosis • Contact allergy to medications • Referral
- 4. Access the activity, “A Closer Look at the Atopic Dermatitis Patient Journey: Effective Management Approaches Across the Age and Disease Spectrum,” at PeerView.com/XHY40. Topical Steroids Identified by Potency and Availability1 PRACTICE AID C: cream; L: lotion; O: ointment. 1. Dimitriades VR, Wisner E. Pediatric Health Med Ther. 2015;6:93-99. Potency Medication Vehicle Size Available Class I (ultra high) Betamethasone dipropionate 0.05% O 15 g, 45 g Clobetasol propionate 0.05% O, C L 15-60 g 30-120 mL Class II (high) Halobetasol propionate 0.05% O, C 15 g, 50 g Betamethasone dipropionate 0.05% C 15 g, 45 g Desoximetasone 0.25% O, C 15 g, 60 g, 100 g Fluocinonide 0.05% O, C 30 g, 60 g Halcinonide 0.1% O, C 15 g, 30 g, 60 g Mometasone furoate 0.1% O 15 g, 45 g Class III (medium to high) Betamethasone dipropionate 0.05% L 30 mL, 60 mL Desoximetasone 0.05% C 15 g, 60 g Fluticasone propionate 0.005% O 15 g, 30 g Triamcinolone acetonide 0.5% O, C 15 g Class IV (medium) Fluocinolone acetonide 0.025% O 15 g, 30 g, 60 g Hydrocortisone butyrate 0.1% O 15 g, 45 g Hydrocortisone valerate 0.2% O 15 g, 45 g, 60 g Mometasone furoate 0.1% O 15 g, 45 g Triamcinolone acetonide 0.1% O C L 15-454 g 15 g, 60 g, 80 g 60 mL Class V (medium to low) Betamethasone valerate 0.1% C 15 g, 45 g Fluocinolone acetonide 0.025% C 15 g, 30 g, 60 g Hydrocortisone butyrate 0.1% C 15 g, 45 g, 60 g Hydrocortisone valerate 0.2% C 15 g, 45 g, 60 g Mometasone furoate 0.1% C L 15 g, 45 g 30 mL, 60 mL Triamcinolone acetonide 0.025% O C L 15-454 g 15 g, 80 g 60 mL Class VI (low) Alclometasone dipropionate 0.05% O, C 15 g, 45 g, 60 g Desonide 0.05% C L 15 g, 60 g 60 mL, 120 mL Class VII (mild) Fluocinolone acetonide 0.01% C 15 g, 60 g Hydrocortisone 0.5%–2.5% O, C L 15-454 g 60 mL, 120 mL
