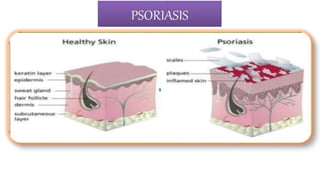
Psoriasis
- 2. Introduction of Psoriasis Psoriasis is a chronic inflammatory, hyperproliferative skin disease. It is characterized by well-defined, erythematous plaque with silvery-white surface scale. Distribution includes extensor surfaces (i.e., knees, elbows, and buttocks) In about 25% of cases, peculiar pitting of nails is seen. Psoriatic arthritis resembling rheumatoid arthritis is produced in about 5% of cases but rheumatoid factor is absent. may also involve palms and scalp (particularly anterior scalp margin). Associated findings include psoriatic arthritis and nail changes (onycholysis, pitting or thickening of nail plate with accumulation of subungual debris).
- 3. History of Psoriasis The word psoriasis is derived from Greek word ‘psora’ means itching. The Greek physician Galen of perganon (130-200 BC) use the term Psoriasis vulgaris to refer all dermo and epidermopathies accompanied by pruiritis. Since 1950 local application and systemic medications are used for the psoriasis.
- 4. EPIDEMIOLOGY Psoriasis is the most commonly recognized papulosquamous disease. It occurs in 2 to 3% of the general population, with considerable variation in different parts of the world. Lower rates are found in Japanese and psoriasis is rare in West Africans. It affects male and female patients equally. Approximately one third of the patients have a positive family history. Psoriasis has a bimodal peak of onset, at age 22.5 years and again at age 55 years. The onset of psoriasis before the age of 15 years is associated with a higher prevalence of positive family history of psoriasis and with more severe disease. Recent epidemiologic studies have shown that psoriasis is associated with an increased risk of heart attack and strokes, a relationship that may be related to a chronic inflammatory state. Psoriasis is also associated in up to 10% of patients with arthritis, which in some cases may be severe.
- 5. PATHOBIOLOGY Psoriasis involves the innate and adaptive immune systems, with abnormal keratinocyte proliferation. Factors playing a role in the pathogenesis include activation of antigen-presenting cells and development of TH1 and TH17 cells. Mediators include interleukin-12 (IL-12), IL-23, tumor necrosis factor-α (TNF-α), and interferon-γ. Exposure to precipitating factors such as infections (e.g., streptococcal or HIV infections), stress, or physical injury results in activation of T cells and generation of cytokines, followed by influx of neutrophils and subsequent release of inflammatory mediators, which lead to the development of cutaneous lesions. Psoriasis has a complex, polygenetic inheritance. Susceptibility genes include PSORS1 to PSORS9, although PSORS1, mapped to chromosome 6p21.3, is now considered a major locus for susceptibility to psoriasis.
- 6. Psoriasis is a multifactorial immunologic disease, both genetic (e.g., human leukocyte antigen [HLA] types) and environmental factors contribute to risk. It is not known if the inciting antigens are self or environmental. Sensitized populations of T cells home to the dermis, including CD4+ TH17 and TH1 cells and CD8+ T cells, and accumulate in the epidermis. These cells secrete cytokines and growth factors that induce keratinocyte hyperproliferation, resulting in the characteristic lesions. Psoriatic lesions can be induced in susceptible persons by local trauma (Koebner phenomenon), which may induce a local inflammatory response that promotes lesion development. GWAS studies have linked an increased risk of psoriasis to polymorphisms in HLA loci and genes affecting antigen presentation, TNF signaling, and skin barrier function. PATHOGENESIS
- 7. DEREGULATED INFLAMMATORY PROCESS PATHOPHYSIOLOG Y STRESS, GENECTIC, AUTOIMMUNE REACTION AND MEDICATION CAUSE HYPERACTIVE OF T-CELLS EPIDERMIS INFILTRATION AND KERATINOCYTE PROLIFERATION
- 8. SILVER SCALING OF SKIN LARGE PRODUCTION OF VARIOUS CYTOKINES ( INTEFERRON, INTERLEUKIN-12) SUPERFICIAL BLOOD VESSEL DILATED AND VASCULAR ENGORGEMENT EPIDERMAL HYPERPLASIA AND IMPROPER CELL MATURATION FAILS TO RELEASE ADEQUATE LIPIDS WHICH LEAD TO FLAKING, SCALING PRESENTATION OF PSORIASIS LESION Cont…
- 9. Etiology of Psoriasis (1)Unknown (2)Genetic Some factor may aggravated the condition such as:- Trauma • Psoriatic lesions can appear at sites of skin trauma, such as scratches or surgical wounds (Kobner isomorphic phenomenon) Infection • β-hemolytic streptococcal throat infections often precede guttate psoriasis. • Severe psoriasis may be the initial presentation of HIV infection. Sunlight • sun exposure, mainly due to Kobnerisation at sites of sunburn or polymorphic light eruption. Drugs • Antimalarials, β-adrenoceptor antagonists (β-blockers), lithium, NSAIDs and anti-TNF-α drugs. Psychological factors • Anxiety and stress may exacerbate psoriasis. Smoking and Alcohol Obesity Hormonal changes
- 10. Types of Psoriasis 1) Plaque psoriasis 2) Guttate psoriasis 3) Inverse psoriasis 4) Pustular psoriasis • Localised • Grneralised 5) Local forms of psoriasis • Palmoplanter • Scalp • Nail (psoriatic onychodystrophy) 6) Psoriatic arthritis
- 12. Plaque Psoriasis Most common type affects approximately 85%. Features pink, well defined plaques with silver scale. Lesion may be single or numerous. Plaque may involve large areas of skin. Classically affects elbows, Knees, buttocks and scalp.
- 13. Guttate psoriasis Guttate psoriasis usually occurs after viral or bacterial (most commonly streptococcal) infection. This is most common in children and adolescents. It is commonly associated with HLA Cw6. Individual lesions are droplet-shaped, small (usually less than 1 cm in diameter), erythematous, scaly and numerous. An episode of guttate psoriasis may clear spontaneously or with topical treatment within a few months, but UVB phototherapy is often required and is highly effective. Guttate psoriasis often heralds the onset of plaque psoriasis in adulthood.
- 14. Inverse or flexural psoriasis psoriasis that occurs in skinfold areas such as the groin, axilla, and inframammary folds. It appears as an erythematous, somewhat shiny patch because of the constant friction in the involved areas, scales are usually absent. May cause diagnostic difficulty when genital or perianal region is affected in isolation.
- 15. Generalized pustular psoriasis is uncommon, unstable and life-threatening. It will often emerge in the context of plaque disease and the onset is usually sudden, with large numbers of small sterile pustules on aerythematous background, often merging into sheets, with waves of new pustules in subsequent days. The patient is usually febrile and systemically unwell, and this must be dealt with as a medical emergency. Pustular psoriasis Pustular psoriasis may be generalized or localized. Localised pustular psoriasis of the palms and soles (palmoplantar pustulosis) is more common, chronic and closely associated with smoking; small, sterile pustules and erythema develop and resolve with pigmentation and scaling. A localised form of sterile pustulosis of a few digits (acropustulosis) can also occur. It is unclear whether these localised forms of pustulosis are truly psoriatic.
- 16. Erythrodermic psoriasis Generalized erythema covering entire skin surface. May evolve slowly from chronic plaque psoriasis or appear as eruptive phenomenon. Patients may become febrile, hypo/hyperthermic and dehydrated. Complication include cardiac failure, infections, malabsorption and anemia. Relatively uncommon
- 17. Palmoplantar psoriasis Can be hyperkeratotic or pustular. May mimic dermatitis look for psoriatic manifestations elsewhere to aid diagnosis. Possibly aggravated by trauma.
- 18. Scalp psoriasis Varies from minor scaling with erythema to thick hyperkeratotic plaques. May extend beyond hairline. Patient scratching may produce asymmetric plaques.
- 19. Nail psoriasis May be present in patients with any type of psoriasis. Can take several forms:- Pitting:- Discrete, well circumscribed depressions on nail surface. Subungual hyperkeratosis:- Silvery white crusting under free edge of nail with some thickening of nail plate. Onycholysis:- Nail separates from nail bed at free edge. Oil drop sign:- Pink/red colour change on nail surface.
- 20. Psoriatic Arthritis Five to 30% of patients with psoriasis may also have psoriatic arthritis, which may precede the appearance of cutaneous lesions 95% of these patients present with peripheral asymmetrical oligoarthritis involving the interphalangeal joints of the hands and feet, while 5% have exclusively axial or skeletal disease. Psoriatic arthritis has been associated with HLAB57, although some studies have also reported HLA-Cw6 in more than 50% of all persons with this disease.
- 21. It will vary according to types of at psoriasis. Initially the first sign of psoriasis is often red spots on the body. The patches of skin Dry, swollen and inflammed Covered with silver white flakes Raised and thick skin. Other symptoms of psoriasis includes:- Pain, itching and burning. Restricted joint motion or pain Cracked and bleeding skin. Dandruff on scalp Pus filled blisters Genital lesions in males. Pitting, small depression on the surface of the nail Yellow, dicsolored nail Koebner phenomenon Arthriti COMMON CLINICAL MANIFESTATIONS
- 23. 1)Auspitzsign(Grattage test):- Removing the scale reveals a smooth, red, glossy membrane with tiny punctate bleeding point. 2) Rich red color:- often referred to as 'salmon pink‘. This quality of color is of special diagnostic value to differentiate psoriasis from eczema in lesions on the palms, soles and scalp. 3) Candle grease sign 4) Koebner’s or Isomorphic phenomenon 5) Holo or Woronoff sign Signs of psoriasis
- 24. PASI Score (Psoriasis Area and Severity Index) ■It is a method to estimate severity of psoriasis in order to evaluate the clinical efficacy of new treatments ■Psoriatic plaques are graded based on three criteria: redness (R), thickness (T), and scaliness (S) ■Severity is rated on a 0-4 scale (0 for no involvement up to 4 for severe involvement) ■The highest PASI score is 12; the lowest is 0
- 26. Diagnostic Investigations Collect history Physical examinations Skin biopsy :- under local anesthesia Blood and radiography test was done to rule out psoriatic arthritis TLC ,ESR, C- Reactive protein, Serum calcium, Serum uric acid. Immunoglobulin Anti-nuclear antibody Nail dipping and skin scraping Throat swab
- 27. Localised patches/plaques Guttate Flexural Erythrodermic Palmoplantar Tinea Pityriasis rosea Tinea Eczema Tinea Eczema Drug eruption Eczema Cutaneous T-cell lymphoma Superficial basal cell carcinoma and Bowen’s disease Secondary syphilis Candidiasis Pityriasis rubra pilaris Seborrhoeic dermatitis Cutaneous T-cell lymphoma (mycosis fungoides) Seborrhoeic dermatitis Lichen planus Drug DIFFERENTIAL DIAGNOSIS
- 28. Complications Infection Fluid and electrolyte imbalance Low self esteem Depression Stress Metabolic syndrome (increased blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol levels) Hypertension Joint damage
- 29. Management of psoriasis Therapy includes 1) Topical medications 2) UV-based treatment 3) Systemic drugs For mild disease, topical therapy with topical corticosteroids(e.g., triamcinolone ointment, 0.1% twice daily for 1 to 2 weeks). Calcipotriene cream (0.005%, twice daily as needed). Tazarotene gel (0.05%, once or twice daily as needed), used alone or in combination, is effective.
- 30. UV-based treatment In patients who have widespread lesions, NB-UVB isthe best option, whereas PUVA should be considered for patients in whom NB-UVB therapy has failed. Systemic drugs For patients with recalcitrant disease, oral medications such as Methotrexate (7.5 to 15 mg/week) Acitretin (25 to 50 mg/day) Cyclosporine (3 to 5 mg/kg/day) Hydroxyurea (1 g/day) Mycophenolate mofetil (1 to 2 g/day) have all been used with success.
- 31. Topical agents Photo(chemo) therapies Systemic agents Intensive inpatient or day-patient care Emollients tars UVB Retinoids Topical agents and photo(chemo)therapie s under medical supervision dithranol vitamin D agonists, PUVA Immunosuppressants, e.g. methotrexate, ciclosporin, mycophenolate, hydroxycarbamide retinoids, excimer laser Immunomodulators, e.g. fumaric acid esters corticosteroids Biological immunosuppressants, e.g. infliximab, etanercept, adalimumab Treatment categories in psoriasis
- 32. BIOLOGIC AGENTS DOSE/DURATION MONITORING SIDE EFFECTS TNF-α INHIBITORS Etanercept (Enbrel) 50 mg SC twice a week for 12 wk, then 50 mg SC weekly indefinitely PPD CBC, LFT Injection site reaction, infection Infliximab (Remicade) 5-10 mg/kg IV at weeks 0, 2, 6, then every 8 wk indefinitely PPD CBC, LFT Infusion reaction, sepsis, lupus-like syndrome, aplastic anemia (rare) Adalimumab (Humira) 80 mg SC at week 0, 40 mg at wk 1, then 40 mg every 2 wk indefinitely PPD CBC, LFT Injection site reaction, infection ANTI-CD2 Alefacept (Amevive) 15 mg IM weekly for 12-16 wk; consider a second course after a 12-wk interval CD4 Infection ANTI–IL-12/23 Ustekinumab (Stelara) SC at weeks 0, 4, then every 12 wk 100 kg: 90 mg indefinitely PPD Infection BIOLOGIC AGENTS FOR PSORIASIS