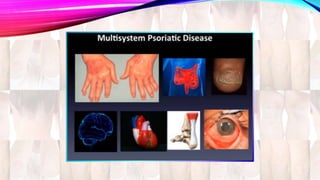
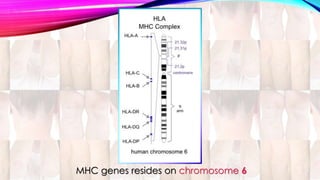
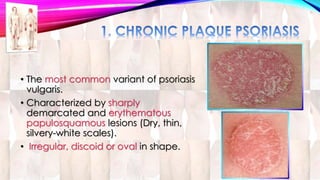
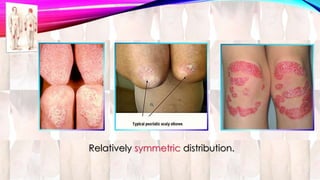
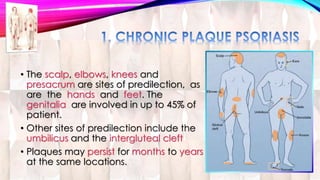
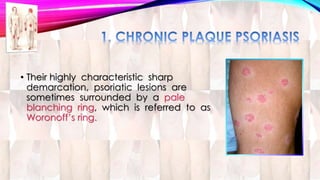
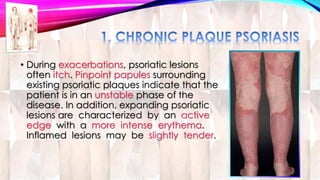
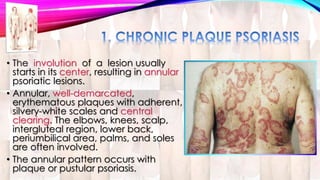
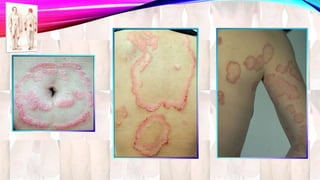
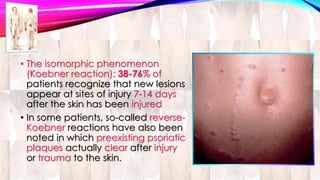
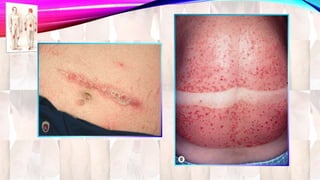
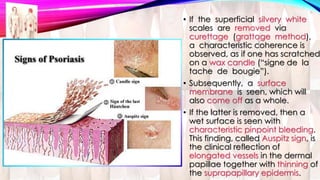
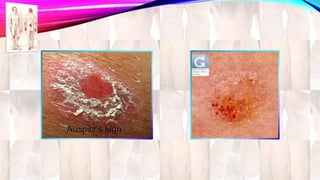
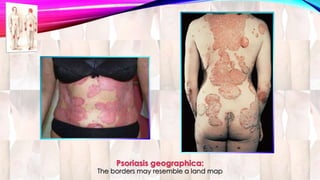
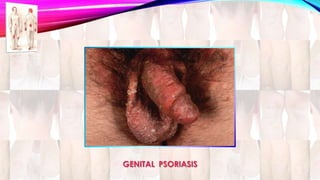
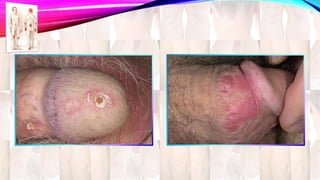
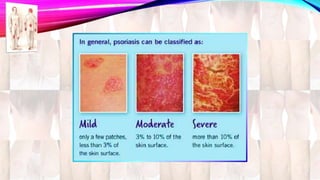
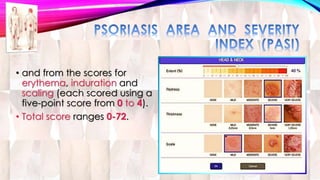
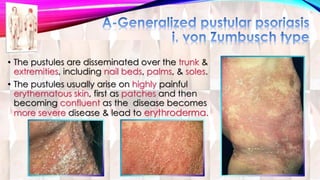
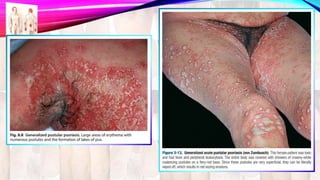
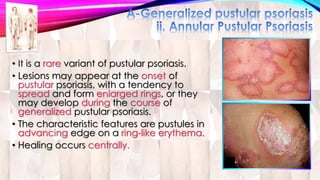
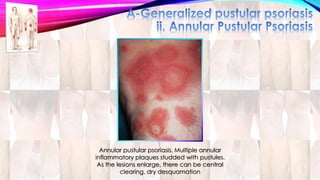
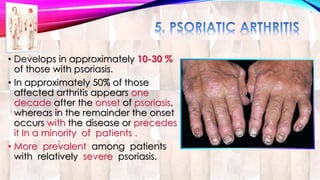
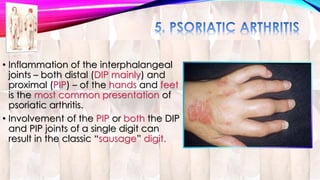
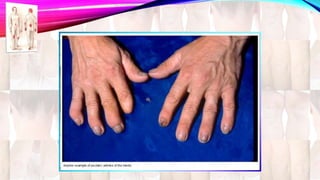
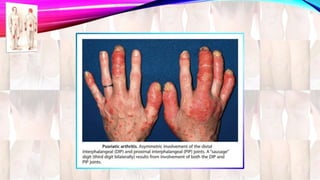
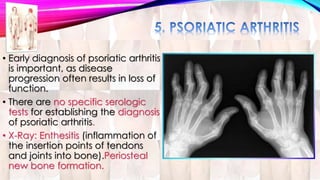
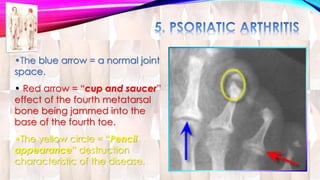
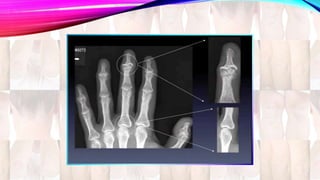
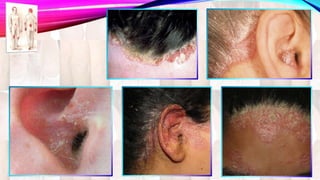
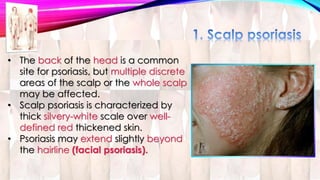
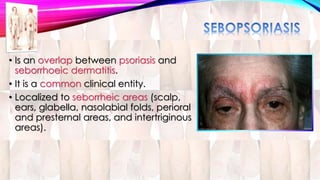
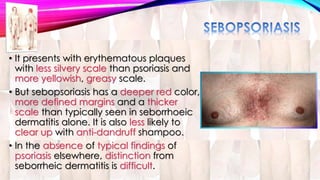
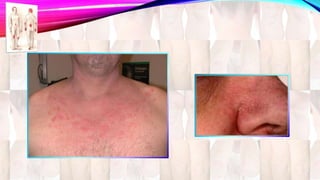
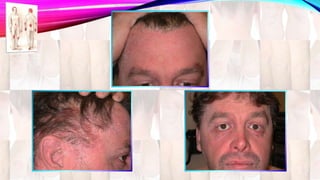
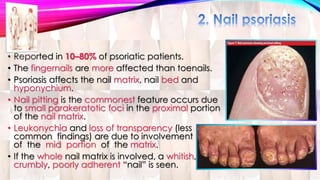
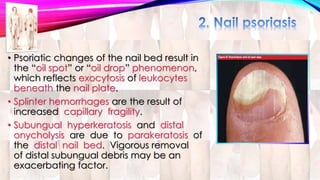
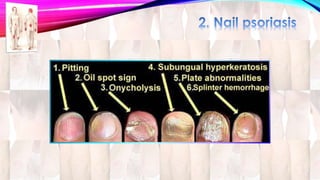
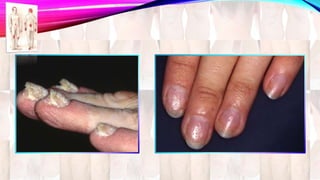
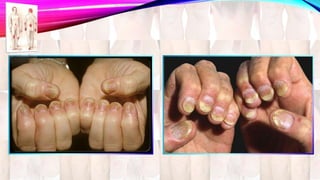
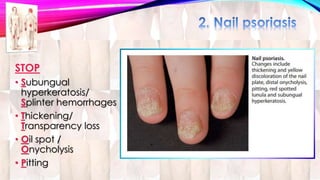
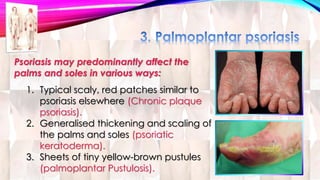
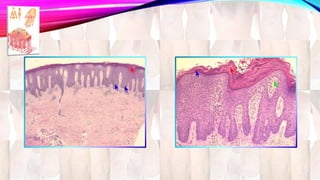
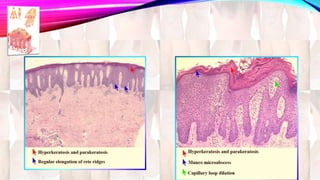
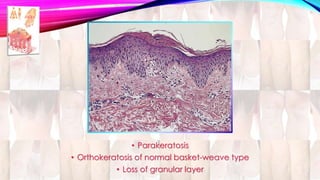
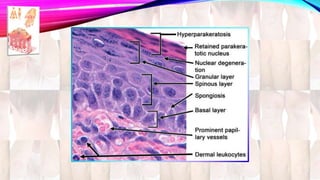
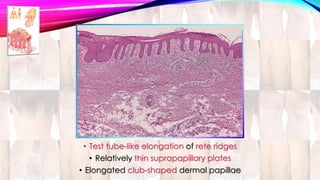
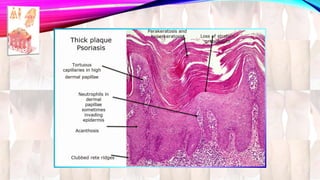
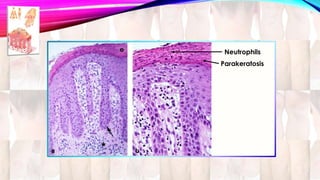
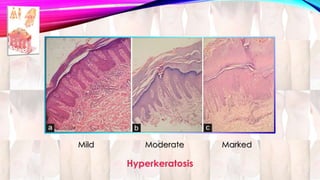
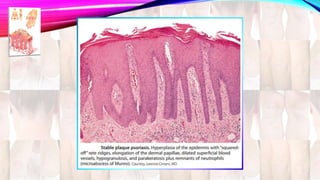
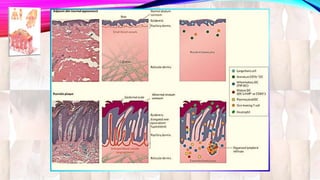
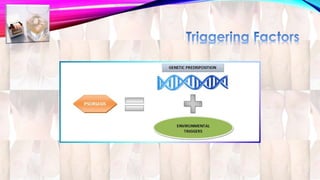
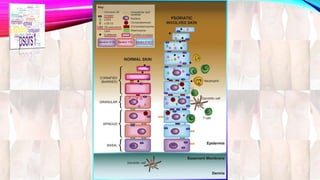
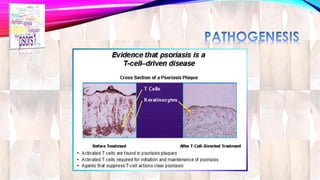
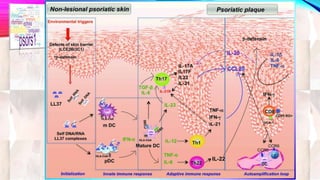
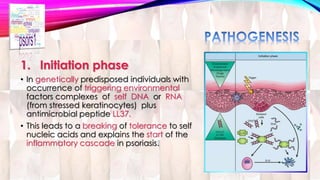
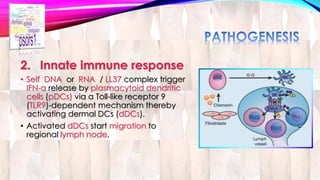
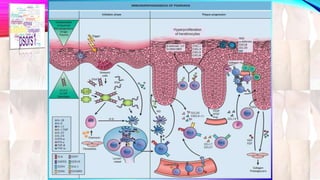
Psoriasis is a chronic immune-mediated disorder with a genetic basis influenced by environmental factors, affecting about 2% of the global population. It presents with characteristic erythematous plaques and has significant impacts on quality of life, with up to 30% of patients developing psoriatic arthritis. The condition can manifest in various forms and severity, with symptoms including itching, localized redness, and scaling, and can be exacerbated by stress or environmental factors.