OCTA Guided PDT Triple Therapy
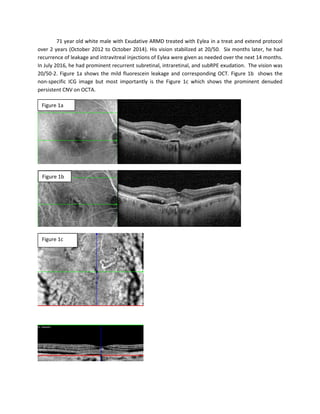
- 1. 71 year old white male with Exudative ARMD treated with Eylea in a treat and extend protocol over 2 years (October 2012 to October 2014). His vision stabilized at 20/50. Six months later, he had recurrence of leakage and intravitreal injections of Eylea were given as needed over the next 14 months. In July 2016, he had prominent recurrent subretinal, intraretinal, and subRPE exudation. The vision was 20/50-2. Figure 1a shows the mild fluorescein leakage and corresponding OCT. Figure 1b shows the non-specific ICG image but most importantly is the Figure 1c which shows the prominent denuded persistent CNV on OCTA. Figure 1a Figure 1b Figure 1c
- 2. Monthly Eylea injections were implemented however his vision deteriorated to 20/200 despite a reduction but incomplete resolution of the leakage (Figure 2a). The OCTA (Figure 2b) showed that new areas of CNV (arrows) were brewing (indistinct areas of increased vascular flow and activity) portending future progression of neovascular disaease and exudation. Note the large choroidal vessels in Figure 2a. In January 2017, the vision had improved to 20/60-2, but the leakage had markedly increased (Fig. 3) Figure 2a Figure 2b
- 3. The Automated 3D Amsler Grid testing system (CEEABLE) shows a central scotoma (Figure 4a) and moderate amounts of metamorphopsia (Figure 4b). One month later, OCTA-Directed PDT Triple Therapy (half-fluence PDT with Triescence preceded by Lucentis) was offered due to the frequency of post Eylea required and the degree of escalating exudation. Photo 5a shows the massive subretinal, intraretinal, and subRPE leakage on OCT. Figure 4a Figure 4b
- 4. Photo 5b shows the multimodality IVFA (left) and ICG (right) revealing neovascularization which is quite prominent on ICG – more difficult to see on IVFA. Targets for PDT administration are shown in Figure 5c based on IVFA/ICG/OCT multimodality imaging. The OCTA (Figure 5d) gives a more focused target, specifically the persistent denuded neovascularization upper nasal from the fovea. Figure 5a Figure 5b Figure 5c
- 5. The CEEABLE grid shows a more prominent scotoma (Figure 6a) and metamorphopsia (Figure 6b). One month after OCTA-Directed PDT Triple Therapy the vision had improved to 20/50-2.The leakage has mostly resolved (Figure 7a). The CEEABLE shows the absence of the scotoma (Figure 7b) and reduction in the metamorphopsia (Figure 7c) that correlates to leakage resolution . Figure 5d Figure 6a Figure 6 b
- 6. Two months after OCTA Directed PDT Triple Therapy, the vision is now 20/50 and leakage is mostly resolved on OCT (Figure 8a) Figure 7a Figure 7b Figure 7c
- 7. The OCTA (Figure 8b) shows disruption of the prominent precombination CNV and a more non- specific area of increased vessel activity. Figure 8a Figure 8b
