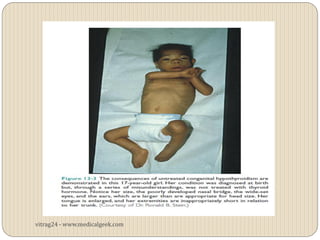
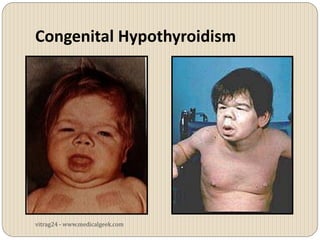
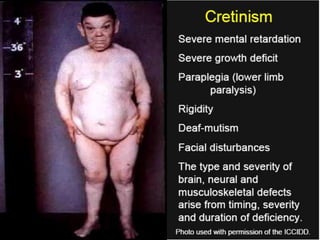
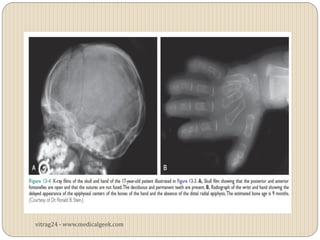
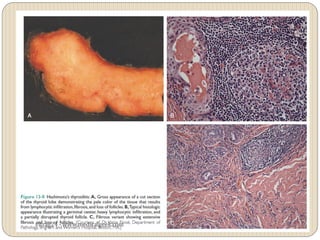
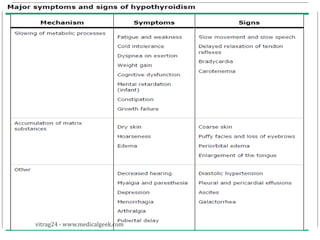
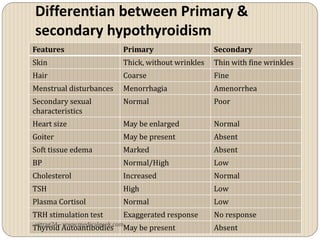
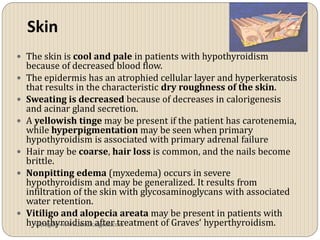
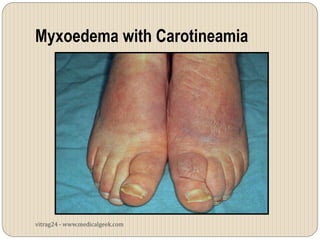
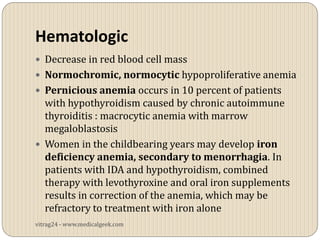
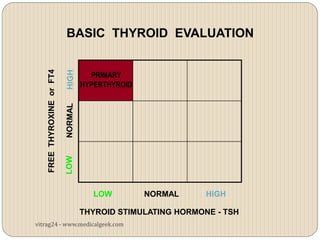
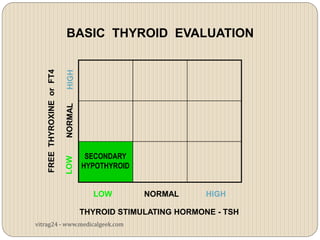
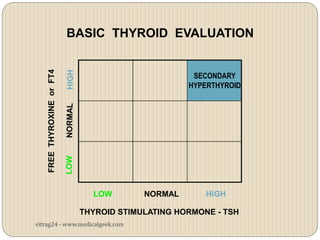
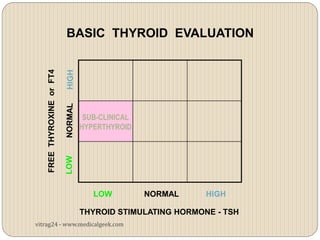
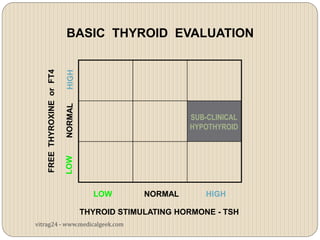
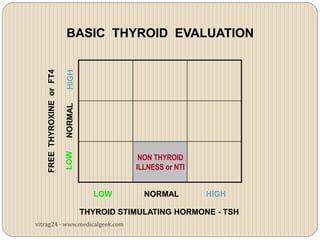
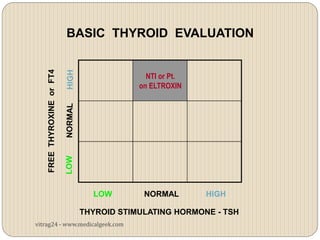
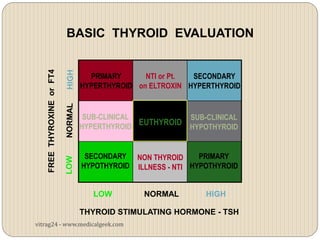
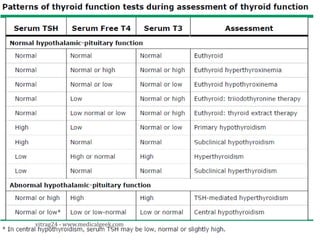
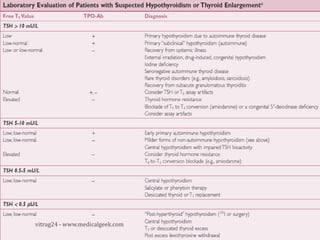
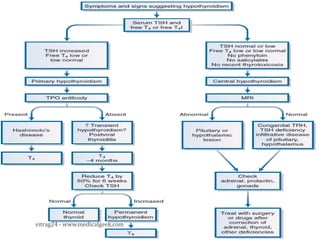
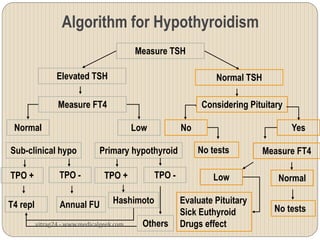
Hypothyroidism affects approximately 42 million people in India, with a prevalence rate of 3.9%, mostly in females and often increasing with age. It can be classified into primary, secondary, and other types, with various causes including autoimmune disorders and iodine deficiency. Early diagnosis and treatment are critical to prevent severe neurologic consequences, especially in congenital cases, while symptoms can range from fatigue and weight gain to more serious complications.