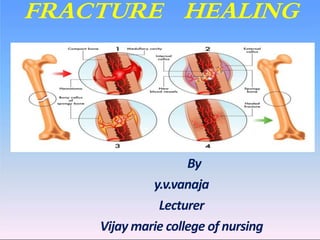
Fracture healing
- 1. FRACTURE HEALING By y.v.vanaja Lecturer Vijay marie college of nursing
- 2. INTRODUCTION • Fracture is a break in the structural continuity of bone or periosteum. • The healing of fracture is in many ways similiar to the healing in soft tissue wounds except that the end result is mineralised mesenchymal tissue i.e. BONE. • Fracture healing starts as soon as bone breaks and continues modelling for many years.
- 3. The essential event in fracture healing is the creation of a bony bridge between the two fragments which can be readily be built upon and modified to suit the particular functional demands .
- 4. Healing fracture by callus formation depends upon some clinical considerations whether the fracture is • Traumatic or pathological • Complete or incomplete like green stick fracture • Simple or compound fracture
- 5. Components of BONE Formation Cortex Periosteum Bone marrow Soft tissue
- 6. STAGES OF FRACTURE HEALING Primary union of fractures: • occurs in a few special situations when the ends of the fracture are approximated as is done by application of compression clamps. • In these cases, bony union takes place with formation of medullary callus without periosteal callus formation
- 7. secondary union Though it is a continuous process, secondary bone union is described under the following 3 headings: i) Procallus formation ii) Osseous callus formation iii) remodelling
- 8. Procallus formation steps involved in the formation of procallus are Haematoma Local inflammatory response Ingrowth of granulation tissue Callus composed of woven bone and cartilage
- 9. Tissue destruction and Hematoma formation – Torn blood vessels hemorrhage – A mass of clotted blood (hematoma) forms at the fracture site – Site becomes swollen, painful, and inflamed
- 10. Tissue destruction and Hematoma formation
- 11. INFLAMATION AND CELLULAR PROLIFERATION • occurs at the site of injury with exudation of fibrin, polymorphs and macrophages. • Macrophages clear away the fibrin, RBC and inflammatory exudate and debris
- 12. Ingrowth of granulation tissue • Begins with the neo vascularization and proliferation of mesenchymal cells from periosteum and endosteum • A soft tissue is formed which joins the ends of fractured bone without much strength
- 13. Callus composed of woven bone and cartilage : Starts with in the first few days. The cells of inner layer of the periosteum have osteogenic potential and lay down collagen as well as osteoid matrix in the granulation tissue. The osteoid undergoes calcification and is called as woven bone callus and united to bridge the gap between the ends giving spindle shape
- 14. Callus Formation
- 15. Osseous callus formation – blThe woven bone is cleared away by incoming osteoclasts and the calcified cartilage disintegrates. – Newly formed blood vessels and osteoblasts invade, laying down osteoid which is calcified and lamellar bone is formed by developing the haversian system cvoncentrically around the blood vessels
- 16. STAGE OF REMODELLING Excess material on the bone shaft exterior and in the medullary canal is removed Compact bone is laid down to reconstruct shaft walls
- 17. Schematic drawing of the callus healing process. Early intramembranous bone formation (a), growing callus volume and diameter mainly by enchondral ossification (b), and bridging of the fragments (c). Figure from Brighton, et al, JBJS-A, 1991
- 18. A: Roentgenogram of a callus healing in a sheep tibia with the osteotomy line still visible (6 weeks p.o.). B: Histological picture of a sheep tibia osteotomy (fracture model) after bone bridging by external and intramedullary callus formation. A few areas of fibrocartilage remain at the level of the former fracture line (dark areas).
- 19. COMPLICATIONS OF FRACTURE HEALING • MALUNION • DELAYED UNION • NONUNION
- 20. MAL UNION A MALUNITED Fracture is one that has healed with the fragments in a non anatomical position. CAUSES 1 INACCURATE REDUCTION 2 INEFFECTIVE IMMOBILIZATION
- 21. Nonunion • FDA defined nonunion as “established when a minimum of 9 months has elapsed since fracture with no visible progressive signs of healing for 3 months” • Every fracture has its own timetable (ie long bone shaft fracture 6 months, femoral neck fracture 3 months)
- 22. Delayed/Nonunion Factors contributing to development: • Systemic • Local
- 23. Delayed/Nonunion cont. Systemic factors: • Metabolic • Nutritional status • General health • Activity level • Tobacco and alcohol use
- 24. Delayed/Nonunion cont. Local factors • Open • Infected • Segmental (impaired blood supply) • Comminuted • Insecurely fixed • Immobilized for an insufficient time • Treated by ill-advised open reduction • Distracted by (traction/plate and screws) • Irradiated bone • Delayed weight-bearing > 6 weeks • Soft tissue injury > method of initial treatment
- 25. Nonunion cont Nonunited fractures form two types of pseudoarthrosis: • Hypervascular or hypertrophic • Avascular or atrophic