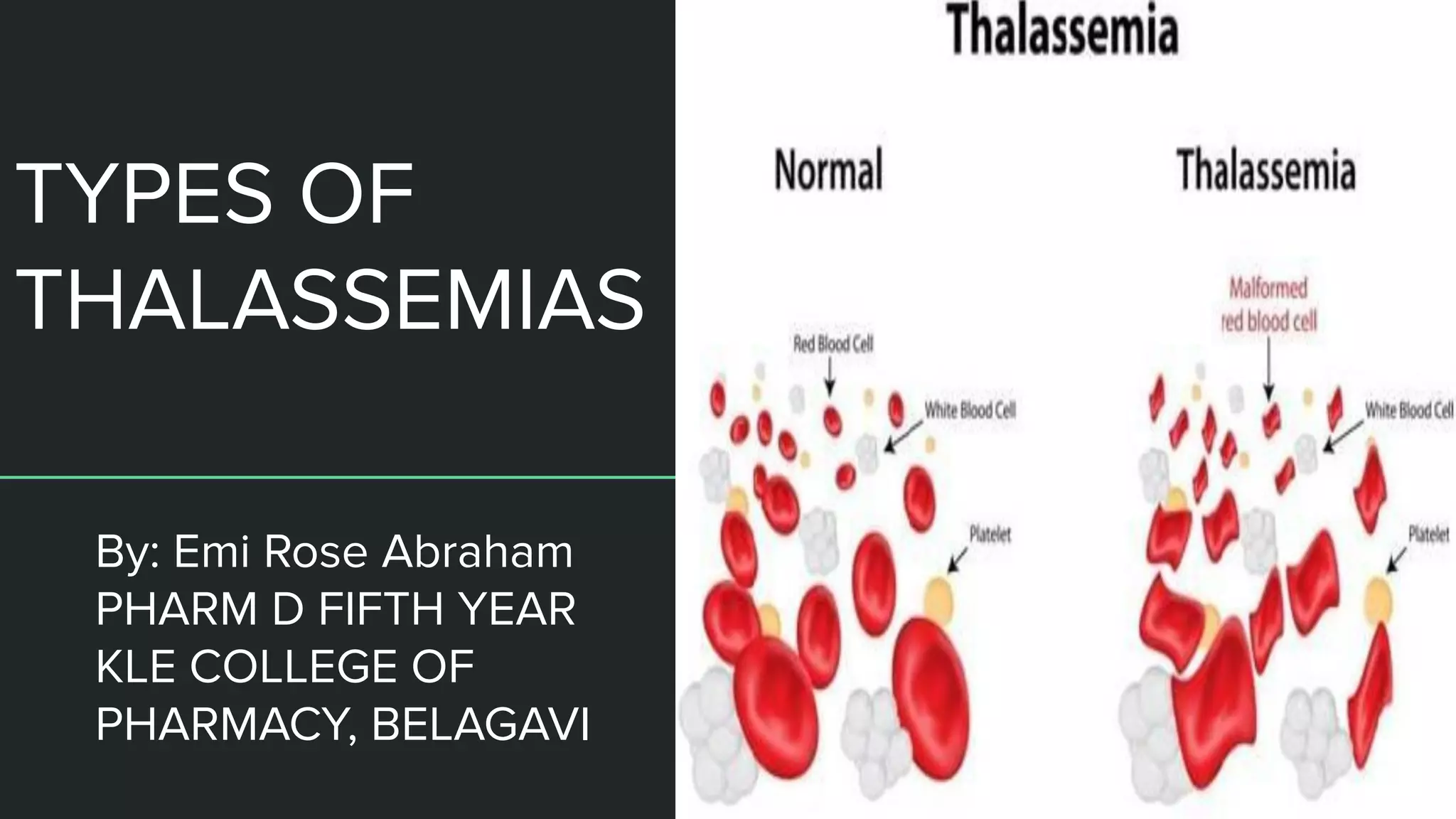
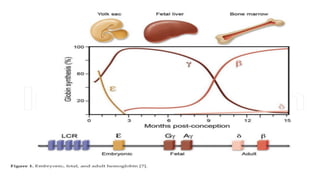
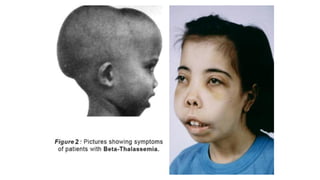
The document discusses thalassemias, hereditary disorders affecting the hemoglobin molecule characterized by a deficiency in the production of alpha or beta globin chains. It outlines the genetic basis, types of thalassemias including alpha and beta thalassemia, their pathophysiology, severity, signs, symptoms, and various classifications. Treatment options, including blood transfusions and bone marrow transplantation, are also mentioned.