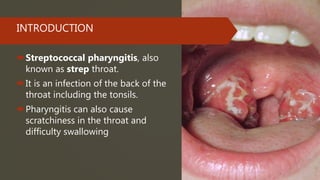
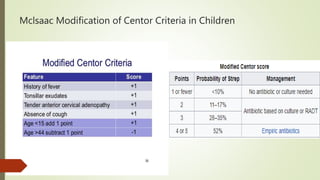
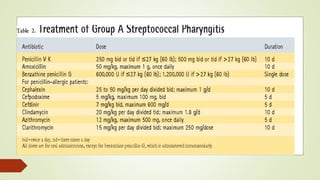
Streptococcal pharyngitis, or strep throat, is a bacterial infection of the throat and tonsils caused by Group A Streptococcus bacteria. It is common in children ages 5-15 and presents with sore throat, fever, pus on the tonsils, and swollen glands. While most cases are mild, complications can include scarlet fever and rheumatic fever. Diagnosis involves a throat culture or rapid strep test. Treatment is usually penicillin or amoxicillin to prevent complications and limit spread. Prevention involves handwashing, avoiding those infected, and treating strep throat with antibiotics.