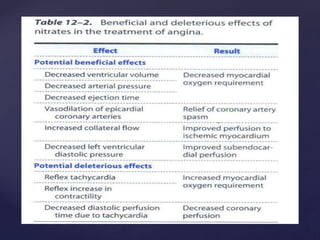
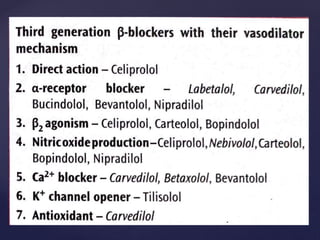
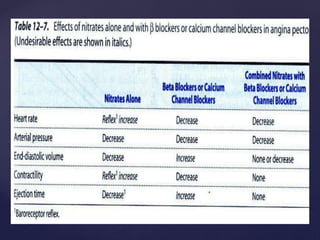
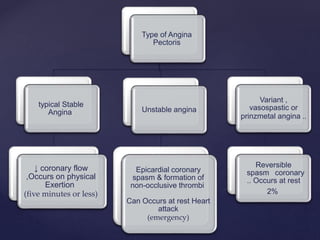
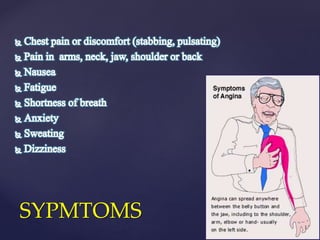
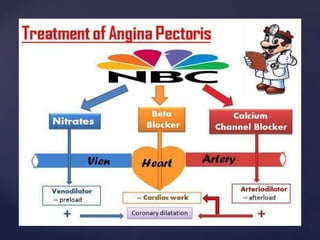
This document provides an overview of ischemic heart diseases and recent advances in treatment. It discusses the types of angina pectoris and myocardial infarction. Current treatment strategies include nitrates, beta blockers, calcium channel blockers, and potassium channel openers. Newer agents that are discussed include trimetazidine, ranolazine, and ivabradine which lower cardiac oxygen demand and improve symptoms of angina. Combination therapies are also used to maximize antianginal effects while minimizing side effects.