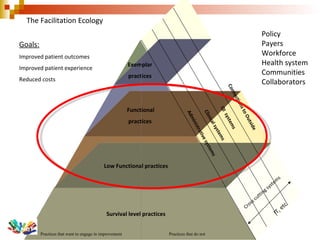
The document discusses the roles and effectiveness of practice facilitators (PFs) in supporting quality improvement within safety net healthcare practices. It highlights the need for specialized training, effective resource allocation, and a tailored approach to facilitation to improve patient outcomes, access, and financial viability in primary care. Ongoing evaluation and collaboration among stakeholders are emphasized as essential for achieving desired healthcare improvements.