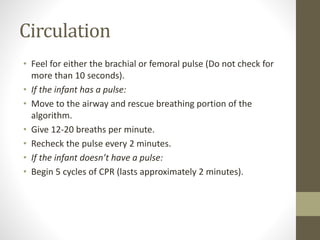
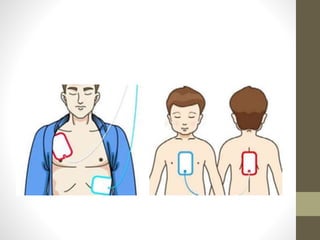
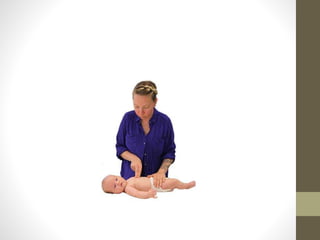
Pediatric advance life support (PALS) is a training for healthcare providers that teaches a systematic approach to evaluating, managing, and resuscitating critically ill pediatric patients. It covers protocols for resuscitating infants and children, including cardiopulmonary resuscitation (CPR) and use of an automated external defibrillator (AED). PALS focuses on identifying and treating reversible causes of cardiac arrest like hypoxia, hypovolemia, hypothermia, and electrolyte abnormalities. Survival rates for in-hospital pediatric cardiac arrest have improved since the introduction of PALS guidelines.