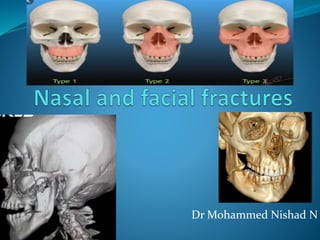
Nasal Fracture Treatment and Complications
- 1. Dr Mohammed Nishad N
- 2. NASAL FRACTURES Isolated fractures of the nasal pyramid --About 40% of all facial fractures. Fractures of the nasal bones are often occured along with other fractures of the facial skeleton. Delay in management --Significant cosmetic and functional deformity . Introduction
- 3. EPIDEMIOLOGY AND ETIOLOGY Relatively little force is required to fracture the nasal bones (25– 75lb/in). Young men --MC. The peak incidence : 15–30-year age group( assaults, contact sports and adventurous leisure activities are more common) . In childhood, Toddler also common (grean stick ) Compound and comminuted fractures are more common in the elderly
- 4. Classification and pathophysiology Nature of injury . Extent of deformity . Pattern of the fracture.
- 5. Nature of injury Laterally applied forces (> 66%) Frontal injuries ( 13%). Greater force is required as the nasal cartilages behave like shock absorbers.
- 6. Extent of deformity . Five-point grading system (developed for the extent of lateral deviation of the nasal pyramid): Grade 0: bones perfectly straight• Grade 1: bones deviated less than half of the width of the bridge of the nose• Grade 2: bones deviated half to one full width of the bridge of the nose• Grade 3: bones deviated greater than one full width of the bridge of the nose •Grade 4: bones almost touching the cheek.
- 7. Pattern of the fracture. Three broad categories :- Class I Class II Class III
- 8. Class 1 fractures(Chevallet ) Result of low–moderate degrees of force . Extent of deformity is usually not marked. Simplest form of a Class 1 fracture is the depressed nasal bone. The fractured segment usually remains in position due to its inferior attachment to the upper lateral cartilage which provides an element of recoil. The nasal septum is generally not involved.
- 9. Severe variant--Both nasal bones and the septum are fractured. The fracture line runs parallel to the naso-maxillary suture ipsilateral to the side of the applied force to a point approximately two-thirds along the length of the nasal bone, where the bone becomes much thicker. The fracture line then connects across to the contralateral side and runs parallel and just below the dorsum.
- 10. The cartilaginous septum is fractured approximately 0.5cm below the dorsum and this aspect of the injury may extend posteriorly into the bony septum, through the perpendicular plate of the ethmoid and skull base.
- 11. Class 2 fractures (Jarjavay) Class 2 fractures are the result of greater force . Associated with significant cosmetic deformity. It involves the nasal bones, the frontal process of the maxilla and septum . The ethmoid labyrinth and adjacent orbital structures remain intact (seen in Class 3).
- 12. The pattern of deformity A frontal impact- results in comminuted nasal bone # and cause gross flattening and widening of the dorsum Lateral impact- produces a high devia-tion of the nasal skeleton.
- 13. It is a complex ‘C-shaped’ fracture Extends from the quadrangular cartilage beneath the nasal tip posteriorly through to the perpendicular plate of the ethmoid, to the anterior border of the vomer forward through the lower part of the perpendicular plate of the ethmoid into the inferior part of the quadrilateral cartilage.
- 15. Class 3 fractures Most severe nasal injuries , result from high velocity trauma. Naso-orbito-ethmoid fractures and often associated fractures of the maxillae.
- 16. The external buttresses of the nose give way and the ethmoid labyrinth collapses on itself. This causes the perpendicular plate of the ethmoid to rotate and the quadrilateral cartilage to fall backwards.
- 17. It causes a foreshortened saddled nose and the nostrils facing more anteriorly, like the snout of a pig (pig-like’ appearance ) There is also telecanthus, which may be exaggerated further by disruption of the medial canthal ligament from the crest of the lacrimal bone.
- 18. Two categories of naso-orbito-ethmoid fractures by Raveh. Type I : -The anterior skull base, posterior wall of the frontal sinus and optic canal remain intact. Type II:- disruption of the posterior frontal sinus wall, multiple fractures of the roof of the ethmoid and orbit that may extend posteriorly to the sphenoid and parasellar regions. Complication :- Multiple dural tears, fluid leaks (CSF), pneumocranium cerebral herniation .
- 19. Clinical presentation History MLC How and when the injury was sustained. Nasal obstruction , Pain. Change in appearance. Anosmia; hyposmia; Watery rhinorrhoea (skull base injury). Visual disturbance; diplopia; epiphora (Orbital trauma). Altered bite; loose teeth; trismus (Dental openion) Occupation.
- 20. Complete nasal obstruction and persisting pain --R/O septal haematoma. H/O previous injuries or past nasal surgery .
- 21. Examination Deviation, Depression, Step deformities. Mobility, Crepitus, Specific areas of point tenderness . Generalized swelling and specific bruising Skin and mucosal lacerations . Septal fracture/haematoma /abscess/perforation Other soft tissue injuries ENT, head &naeck examination
- 22. Investigation Nasal X-rays CT SCAN CSF analysis ,beta 2 transferrin
- 23. Treatment Indications for surgery in the acute phase significant cosmetic deformity nasal obstruction caused by a septal haematoma. Most of the patients (up to 80%) do not require any active treatment (undisplaced fracture). Soft-tissue swelling may mimic deformity — Reassurance. Topical vasoconstrictor drops --Alleviate congestion and obstructive symptoms.
- 24. Pts with pre-existing nasal deformity caused by a previous incident--Septorhinoplasty when everything has settled down some months later. Pts --Occupational hazard, sport or leisure activity-- It is better to advise definitive septorhinoplasty when the risk of further injury no longer exists.
- 25. The optimal time for clinical assessment around 4 days-- oedema will subside and any underlying deformity become apparent – ( So R/A 4 days –Reduction with in next 2-3 days ) >7 day delay -- effective reduction difficult and sometimes will require osteotomies. In children, healing occur more quickly and earlier intervention is indicated.
- 26. Anaesthesia LA/GA Local anaesthesia -- combination of external infiltration with internal application of topical preparations. Lignocaine is injected along the nasomaxillary groove, infraorbital nerve in its foramen and around the infratrochlear nerve. Topical EMLA (prilocaine and ligno-caine) cream or AMETOP (amethocaine) gel to the external nose instead of infiltration
- 27. Within the nose, sprays, injections, pastes or packs coated with local anaesthetic OR combinations of cocaine, lignocaine, adrenaline and phenylephrine. GA Indication- Patients who are not suitable for reduction under LA, Children , Patients with low pain thresholds or significant anxiety states , Delay in presentation
- 28. Methods of reduction Closed technique--The general principle is to mobilize the fragments first by increasing and then decreasing the degree of deformity. Various elevators and forceps have been developed specifically for this purpose,(Freer, Hills and Howarth elevators and Ashe and Walsham forceps .
- 30. All Class 1 and most Class 2 fractures can be reduced with closed techniques. Some Class 2 fractures –Open reduction ( require Osteotomy- to release the fragments before manipulation) A splint or plaster applied to the nasal bridge maintains the position of the nasal bones and prevents accidental displacement. Splints kept in place for about 7 days. Refrain from contact sports for at least 6 weeks.
- 31. indications for open reduction: Bilateral fractures with dislocation of the nasal dorsum and significant (pre-existent or recent) septal deformity. infraction of the nasal dorsum . Fractures of the cartilaginous pyramid, with or without dislocation of the upper laterals. For depressed tip or flail lateral fractures (unstable despite closed reduction techniques) --Kirschner (K) wires can be used(Removed after 2 wks)
- 32. Septal reduction -- performed with Ashe’s forceps, but often requires a Killian or hemitransfixion incision, elevation of mucosal flaps to expose cartilage and bone fragments, and replacement and/or removal of cartilaginous and bony fragments. Quilting sutures prevent haematoma formation. Management of the nasal septum
- 33. COMPLICATIONS Poor cosmetic result : Factors include: 1• Extent of the injury. 2• Time delay in surgical reduction. 3• Poor surgical technique. 4• Unrecognized and untreated septal fracture. 5• Pre-existing nasal deformity. 6• Post-operative trauma (in recovery room or subsequently). 7• scarring and fibrosis
- 34. Nasal obstruction : Causes: 1• Valve obstruction . 2• Collapse of upper lateral cartilages and depressed nasal bones. 3• Septal deviation. 4• Widened septum (haematoma). 5• Tip ptosis.
- 35. Epistaxis Fractures involving the nasoethmoidal complex can cause laceration to the anterior ethmoidal artery-- Result in repeated, brisk and significant haemorrhage --Stops once the fracture has been reduced. Rarely prolonged packing or ligation of the artery is required. Bleeding can also occur at the time of reduction( if instruments are used.) Preparation of the nose with vasoconstrictive agents helps to minimize this blood loss.
- 36. Septal complications submucoperichondrial bleed . Septal haematomas ,Septal abcess Cartilage necrosis ,Septal perforation Nasal deformity –saddle nose,columellar retraction,broadened septum Septal haematomas : Acute unilateral or bilateral nasal obstruction . On inspection --Reddish-purple, fluctuant swelling of the caudal septum. A deviated septum can be confused with a septal haematoma. Gentle pressure on the bulging area -- fluctuant if a collection is present. Untreated, -- Abscess ( fluctuating fever and severe facial and cranial pain). Rarely, cavernous sinus thrombosis or other forms of intra- cranial sepsis .
- 37. The haematoma or abscess - drained under LA/GA, using needle aspiration or . Preferably an incision. Quilting sutures - to eliminate the dead space. Packs or splints - to provide pressure on the septum. Appropriate antibiotic therapy
- 38. Facial fractures Introduction : Maxillofacial trauma is extremely common. 10%of all accident and emergency attendances are related to facial injuries. Immediate assessment of the airway is essential. Most facial fractures are managed by semi-rigid internal fixation through extended subperiosteal exposure of the fracture. Wiring of the jaws is no longer the standard of care. Cerebrospinal fluid (CSF) rhinorrhoea and retrobulbar hae-matoma should be excluded in all middle-third facial injuries.
- 39. RTA,Physical violence, falls, attempted suicide, and sporting injuries. Most injuries are low energy and heals well. Higher-energy injuries cause grosscomminution of the bones and do not heal as well Aetiology
- 40. Primary care 1.Airway: Evaluate and secure the airway, while maintaining alignment of the neck in case there is an unstable cervical spine injury. 2.Breathing: Make sure that there is adequate ventilation. 3.Circulation: Control sources of blood loss. 4.Disability: Assess the level of consciousness and neurological dysfunction. 5.Exposure: Ensure that all other injuries are identified. ATLS Protocols must be followed
- 42. Principles of primary management Once the primary survey of the injury completed, a secondary survey is carried out to exclude other injuries and to categorize the extent of the facial injury. The soft tissues of the face -- Any lacerations or cuts near relevant anatomical structures -- eyebrows, conjunctival margins, nasal aperture and the vermillion border of the lips. Facial nerve function . Integrity of the parotid duct .
- 43. Visual acuity and ocular movements. (retrobulbar haemorrhage and retinal detachment--both are preventable and treatable causes of permanent blindness.). Palpating the orbital margins, zygomatic projection, nasal skeleton and mandibular outline. A full dental examination is necessary. Dental occlusion and maxillary or mandibular instability .
- 44. Radiographic evaluation X-rays of the facial skeleton, chest, cervical spine and pelvic . computerized tomography (CT) scan –Head &Facial skeleton. The timing of any maxillofacial intervention is contro- versial. With modern-day techniques-- trend is to fix facial fractures earlier. ( avoids double insult of accidental and surgical trauma). Swelling can be reduced by head-up position with ice packs, together with a single dose of dexamethasone. Facial wounds should be cleaned and lacerations closed as soon as possible. parenteral prophylactic anti-biotics
- 45. BEST CLINICAL PRACTICE ✓Maxillofacial fractures can endanger the airway. ✓Be aware of associated cervical spine injuries. ✓Consider tracheostomy at the outset in patients with extensive trauma. ✓Close soft tissues injuries as soon as possible. ✓CT scans of the head and facial bones help to define the extent of both facial and cerebral injuries. ✓Do not forget to give tetanus prophylaxis. ✓Exclude cervical spine injuries. ✓Check visual acuity in all patients with middle-third facial injuries.
- 47. Introduction Parabolic-shaped bone with a complex articulation that consists of paired synovial joints – the temporomandibular joint. Rehabilitation requires accurate reduction, adequate fixation and mobilization. The traditional method of treatment was immobilization of the fracture with intermaxillary fixation (IMF) . Nowadays –Miniplates fixation
- 48. Surgical anatomy Direct and indirect force. Fractures happen at points of potential weakness where the bone is relatively thin. The angles of the mandible -weakened by unerupted wisdom teeth, the para-symphysis- by the long root of the lower canine condylar neck -by its slender anatomy. Multiple site # also common Displacement of the fracture depends --Pull of attached muscles.
- 49. Signs and symptoms Depends on site of the fracture. Fractures of the body, angle and symphysis : Step deformity palpable either externally or intraorally Asymmetry of the lower dental arch and derangement of the occlusion. Pain and paradoxical movement and crepitus on dis- traction of the fractured segments . Haematomas in the buccal sulcus or floor of the mouth. Blood-stained saliva , Anaesthesia of the lower lip
- 50. Fractures of the condylar neck Tenderness over the TMJ. Trismus. Deviation of the jaw towards the injured side on open- ing the mouth. Inability to move the mandible to the side opposite the fracture. Deviation of the jaw to the fractured side at rest with an anterior open bite secondary to gagging of the molar teeth in fracture dislocation. Symmetrical anterior open bite in bilateral fractures of the necks of the condyles.
- 51. Closed reduction techniques Inter Maxillary Fixation (IMF) :-Much smaller role in modern maxillofacial surgery. Role in two groups of patients. First :- undisplaced fractures and no neural deficits who want to avoid more complex surgery . second, :- unilateral condylar fractures. In casuality IMF :-A simple tie wire placed around the teeth either side of a displaced fracture can reduce pain, bleeding from bone ends and make nursing easier in the initial hours and days before a planned open reduction and internal fixation.
- 52. THE INTACT DENTAL ARCH Methods of applying wire to an intact dental arch to provide IMF . Eyelet wires:- Can be applied if two adjacent teeth in contact. Disadvantage :- Difficult to combine eyelet wires with elastic traction Difficult to thread wire through tight interdental contact points. Modification is the Leonard button , an eyelet wire with a small metal disc instead of a loop.
- 53. THE INCOMPLETE DENTAL ARCH Arch bars :- It is a strip of metal that is wired to each jaw using several individual teeth. The bar is prefabricated using a dental impression (intra op/pre op). It can span short gaps within each jaw, but not with large gaps or when there is no posterior tooth. Advantage - stabilize more complex fractures provide indirect fixation
- 54. Intermaxillary bone pins A mono-cortical screw is placed through the mucosa between the canine and first premolar on each side and jaw. The screws are then wired together with elastic bands. The path of the screw should enter the bone and avoid the roots of teeth. These screws are brittle and care must be taken while inserting them .
- 55. External fixation Indication:- patients with gross tissue loss ( seen in war and for those with pathological fractures,) patient is too unwell to undergo extensive surgery. Method – Placement of corti-cal screws and then connecting them with an external bar made of acrylic.
- 56. Internal fixation ACCESS:- Intra-oral incisions bone plates are placed through an intra-oral approach. Mucogingival incisions are made – flap includes the periosteum Care must be taken- damage to mental nerve.
- 57. Extra-oral incisions External incisions use - for the lower border of the mandible and condylar neck. Lower border plates are ideal when there is gross comminution or tissue loss. Incision - made two finger-breadths below the lower border of the mandible in order to avoid damage to the mandibular branch of the facial nerve. Condylar neck fractures are approached through a retro-mandibular incision . Higher condylar neck fractures are better exposed through a pre-auricular incision .
- 58. FRACTURES OF MAXILLA INTRODUCTION subdivided :-lateral (zygomatic) central (maxillary, nasal, nasorbito-ethmoid) . Symptoms and signs --depend on the level of the fracture The classical features of a midfacial fracture – circum-orbital ecchymosis (panda facies), facial oedema emphysema, lengthening of the face anterior open bite. infra-orbital nerve sensory deficit bruising at the junction of the hard and soft palate
- 59. Surgical anatomy The bone of the midfacial region - very thin and offers little resistance to anterior and lateral forces. Le Fort described three levels of midfacial fracture
- 60. 1.Le Fort 1 (guerin #) This fracture runs above the floor of the nasal cavity, through the nasal septum, maxillary sinuses and inferior parts of the medial and lateral pterygoid plates.
- 61. Le Fort 2 (pyramidal fracture) Fracture line runs from the floor of the maxillary sinuses superiorly to the infraorbital margin and through the zygomaticomaxillary suture. orbit --it passes across the lacrimal bone to the nasion. The infraorbital nerve is often damaged by involvement in this fracture.
- 62. Le Fort 3 :- Disconnection of the facial skeleton from the cranial base. The fracture traverses the medial wall of the orbit to the superior orbital fis-sure and exits across the greater wing of the sphenoid and zygomatic bone to the zygomaticofrontal suture. Posteriorly-It runs inferior to the optic foramen, across the lesser wing of the sphenoid to the pterygomaxillary fissure and sphenopalatine foramen. The arch of the zygoma is also broken.
- 63. Le Fort classification is attractive and accu-rate for low-energy injuries, in high-energy injuries there are very few instances of pure Le Fort fractures and most configurations involve multiple Le Fort levels,33together with zygomatic and nasal/nasoethmoid com-ponents.
- 64. Signs and symptoms •epistaxis . •circumorbital ecchymosis. •facial oedema. •surgical emphysema. •lengthening of the face. •infraorbital anaesthesia.
- 65. Management Emergency Treatment It can compromise the airway with torrential epistaxes and posterior impaction of the maxilla. The bleeding can be arrested by using epistats or anterior and posterior nasal packs. If retroposition of the maxilla --it can be pulled forwards using the index and middle finger placed behind the patient’s soft palate
- 66. REDUCTION The maxilla is mobilized by a combination of digital pres-sure and traction on arch bars or interdental wires. FIXATION Internal fixation with 1.3 or 1.5mm, low-profile miniplates placed along the buttresses . Subperiosteal elevation with preser-vation of the infraorbital nerve allows reconstruction of the paranasal and zygomatic buttresses
- 67. . The infraorbital rim needs to be reduced and fixed in Le Fort 2 maxillary fractures, nasomaxillary fractures, zygomatic injuries and orbital floor repairs.
- 68. Zygomatic complex fracture Surgical anatomy The body and processes of the zygomatic bone forms lateral middle third of the facial skeleton. Blows to this part cause – Depressed fracture of the entire zygomatic bone Fracture of the zygomatic arch .
- 69. ‘Tripod fracture’ because of the disruption of the three commonly recognized articulations 1.fronto-zygomatic 2.infraorbital rim 3.zygomaticomaxillary buttress. Accurate anatomical reduction is important for facial appearance, optimum function of the eye, and because of its close proximity to the coronoid process, for opening and closing the mandible.
- 70. Signs and symptoms The lateral aspect of the face will be swollen and bruised. subconjunctival haemorrhage . Periorbital edema . Eye movements restricted, particularly in upward gaze if there is an orbital floor dehiscence and blowout of the orbital contents . Step deformity of the infraorbital margin. frontozy-gomatic suture - tender . In arch fractures -palpable depression and limited mouth opening. Altered sensation of the cheek.
- 71. Imaging fractures are visible on 15 and 30° occipi-tomental X- rays, CT scanning -if there are signs of diminished ocular motility. Hess charting should done in all cases with subjective diplopia.
- 72. Management Minimally displaced fractures – Conservative with a full explanation to the patient and instruc-tions not to blow their nose for a period of 2–3 weeks. Review after 10 days to make sure that no active intervention is required. Displaced fractures – Reduction with or without fixation.
- 74. GILLIES TEMPORAL APPROACH:- Small incision is made down to the superficial temporal fascia. The fascia is then incised and an elevator is passed down on the temporalis muscle so that its tip lies just under the fracture. The bone is then elevated.
- 75. POSWILLO HOOK:- The point of application of the hook is the intersection of a line drawn vertically from the lateral orbital margin and a horizontal line drawn from the inferior margin of the nose. The hook is inserted through a stab incision and the zygoma lifted back into position
- 76. INTRA-ORAL OR KEEN APPROACH mucogingival incision is made in the buccal sulcus in the molar/premolar region. An elevator may be passed behind the zygomatic body to elevate the fracture.
- 77. Post-operative care The patient is instructed not to blow their nose , For the first 12 hours, they should be closely observed for signs or symptoms of a retrobulbar haemorrhage. Increasing pain, Proptosis, Ophthalmoplegia, Diminishing visual acuity Loss of light reflex Dilated pupil Palpable increase in ocular pressure indicate the need for urgent exploration and evacuation of any haematoma. long-term complications - malunited fractures.
- 78. ORBITAL FLOOR FRACTURE Blunt trauma to the globe or adjacent bone can lead to fracture of the orbital floor. Signs and symptoms :- cardinal signs :-- Enophthalmos Hypoglobus (depressed pupillarylevel). Other signs :- Supratarsal hollowing, Hooding of the eye, Narrowing of the palpebral fissure width infraorbital nerve deficit. Diplopia on upward gaze
- 79. Imaging:- CT imaging with axial, coronal and sagittal plane Management:- exploration and repair. soft-tissue components should be mobilized and supported by a graft. Various grafts and materials --Polydimethylsiloxane (PDS) , Titanium alloplasts are used
- 80. Naso orbito ethmoid fractures Definition and classification It involve the ana-tomical confluence of the nose, orbits and ethmoids. Markowitz et al classified NOE in terms of their attachment to the medial canthal ligaments
- 81. Signs and symptoms:- Loss of nasal projection Tipping up of the end of the nose Splaying of the nasal root and telecanthus -- Gross comminution. Blunting of the canthal angle and movement of the medial canthus can be elicited by displacement of the lateral palpebral ligament. common features
- 82. Management Type I fractures : stabilized using miniplates. Surgical access is through a coronal flap, intra-orally and lower eyelid incisions may be required. Type II and III fractures: repaired with miniplates. Require transnasal canthopexy to reduce the telecanthus and hold the position of the medial canthal ligaments. This is done by plates and/or a wire. The lacrimal integrity should be assessed pre- or peri- operatively and stented if damaged
- 83. THANK YOU