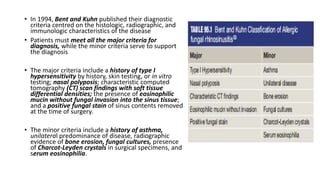
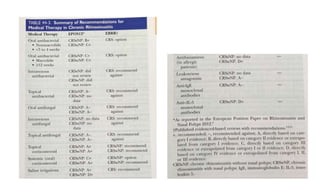
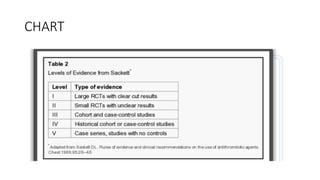
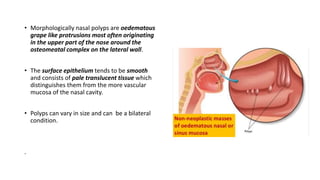
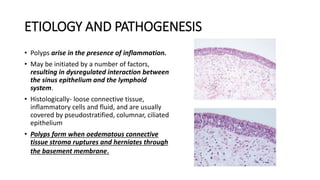
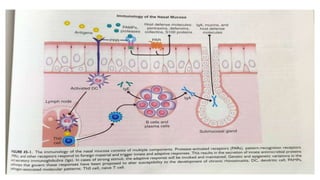
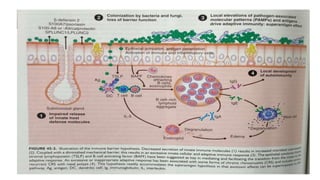
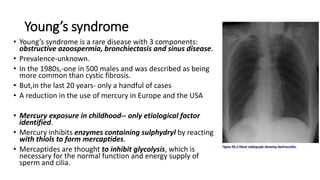
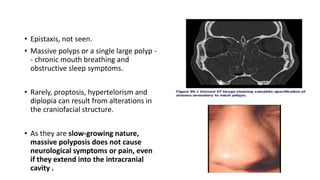
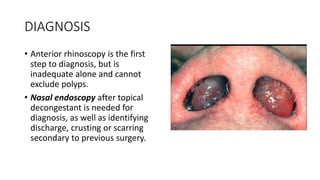
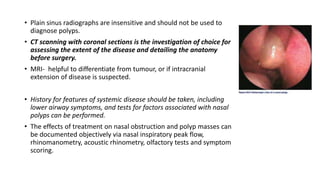
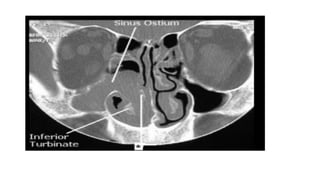
Nasal polyps are non-cancerous growths that can develop in the nose or sinuses. They are defined as a form of chronic rhinosinusitis with nasal polyps (CRSwNP). Nasal polyps are most often caused by inflammation within the nose and sinuses and can be triggered by environmental irritants, infections, or genetic factors. Clinically, nasal polyps may cause nasal congestion, nasal discharge, facial pain or pressure, and reduced or loss of smell. They can range in size from small to large polyps that cause significant obstruction. Nasal polyps are often associated with conditions like asthma, aspirin sensitivity, cystic fibrosis, and immune system disorders.