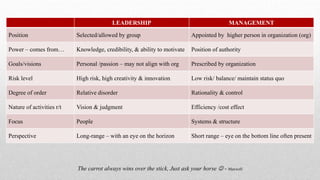
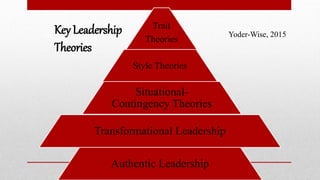
This document provides an overview of leadership in long-term care. It discusses how leadership theories have evolved over time from trait theories to current theories like transformational leadership. It also outlines objectives, trends impacting healthcare, governing bodies, knowledge and skills for nursing leadership. Key components of transformational leadership are described including building relationships and trust, creating an empowering work environment, and balancing priorities. The importance of organizations supporting nursing leadership is highlighted.