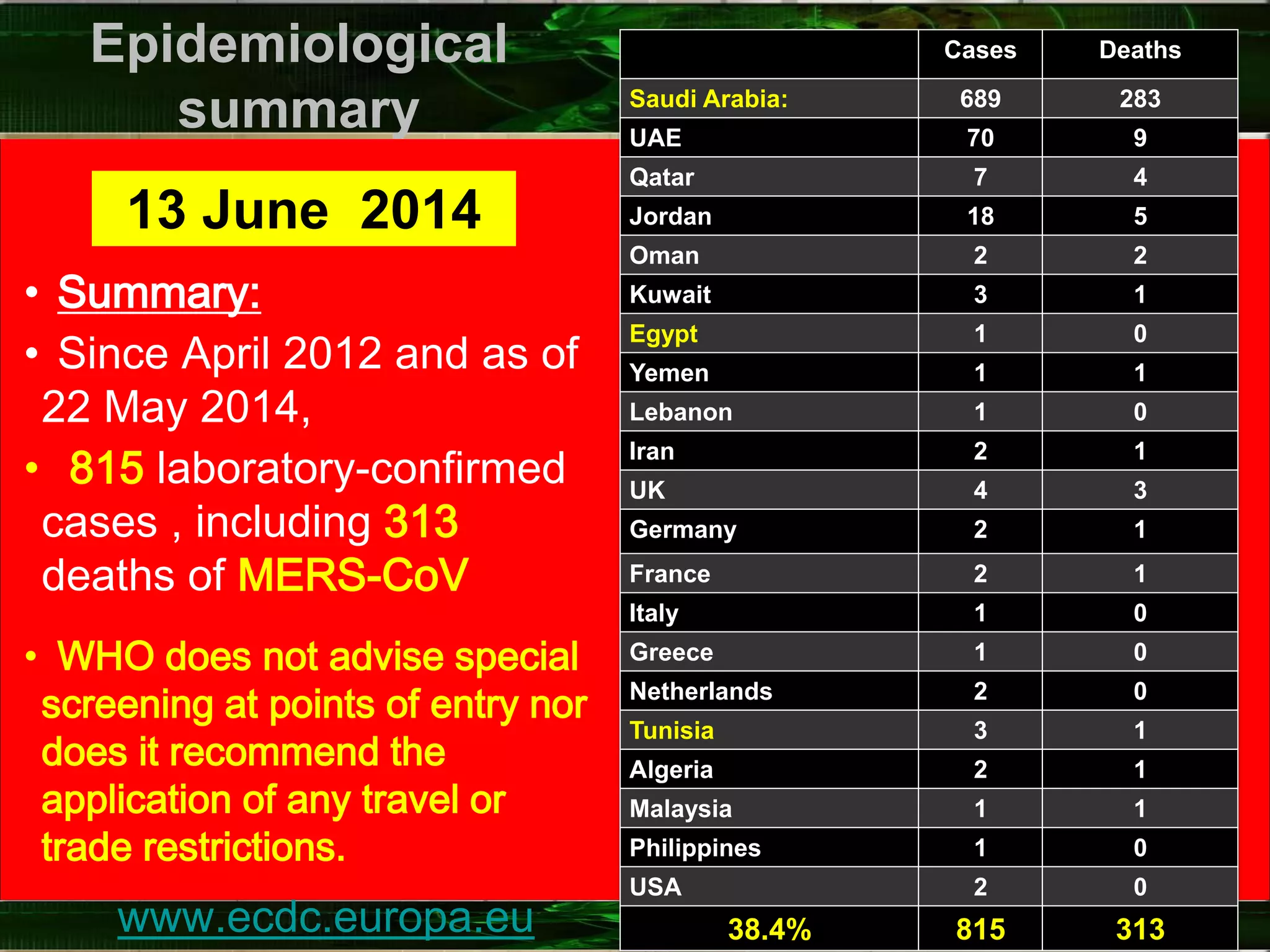
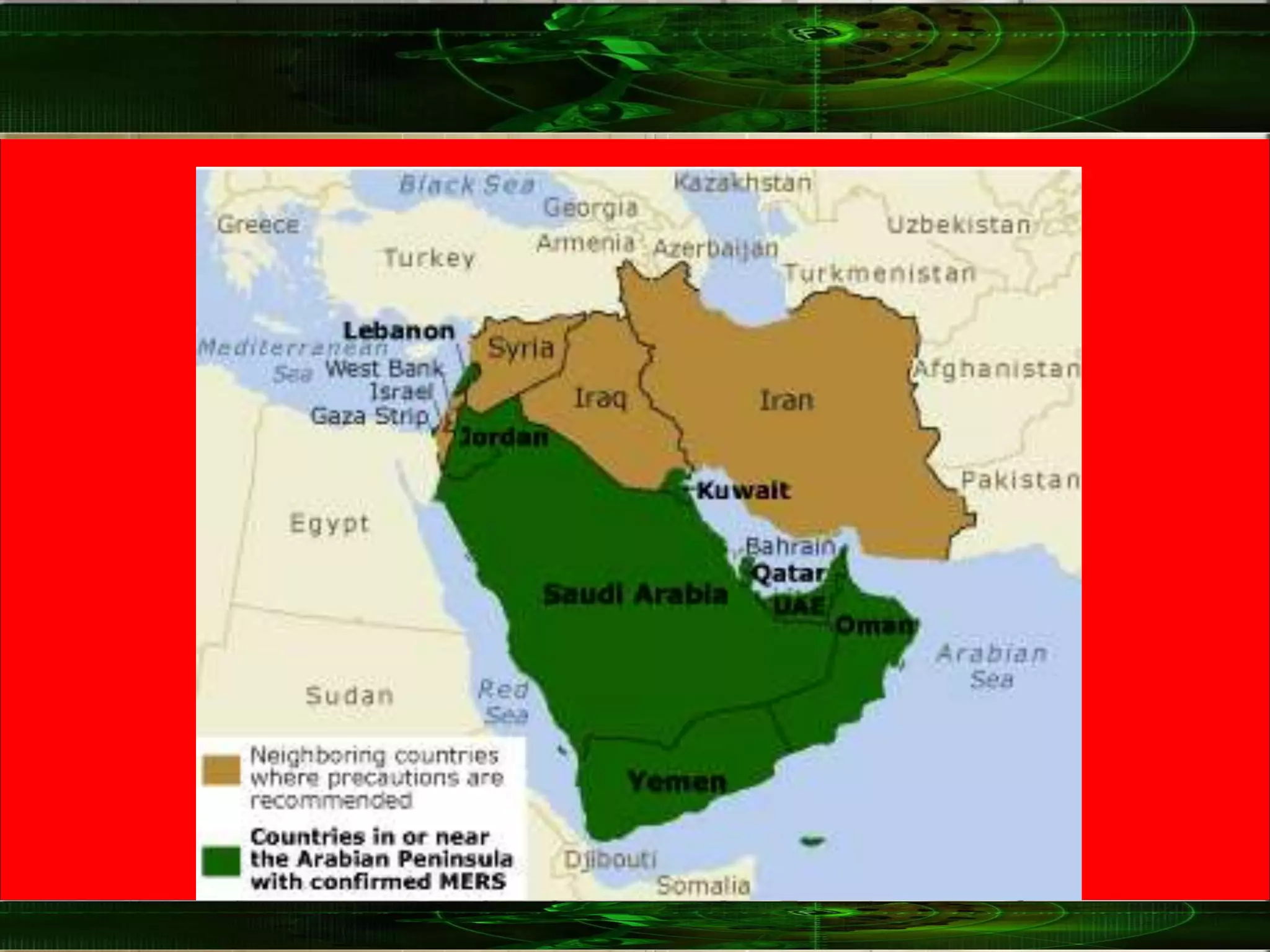
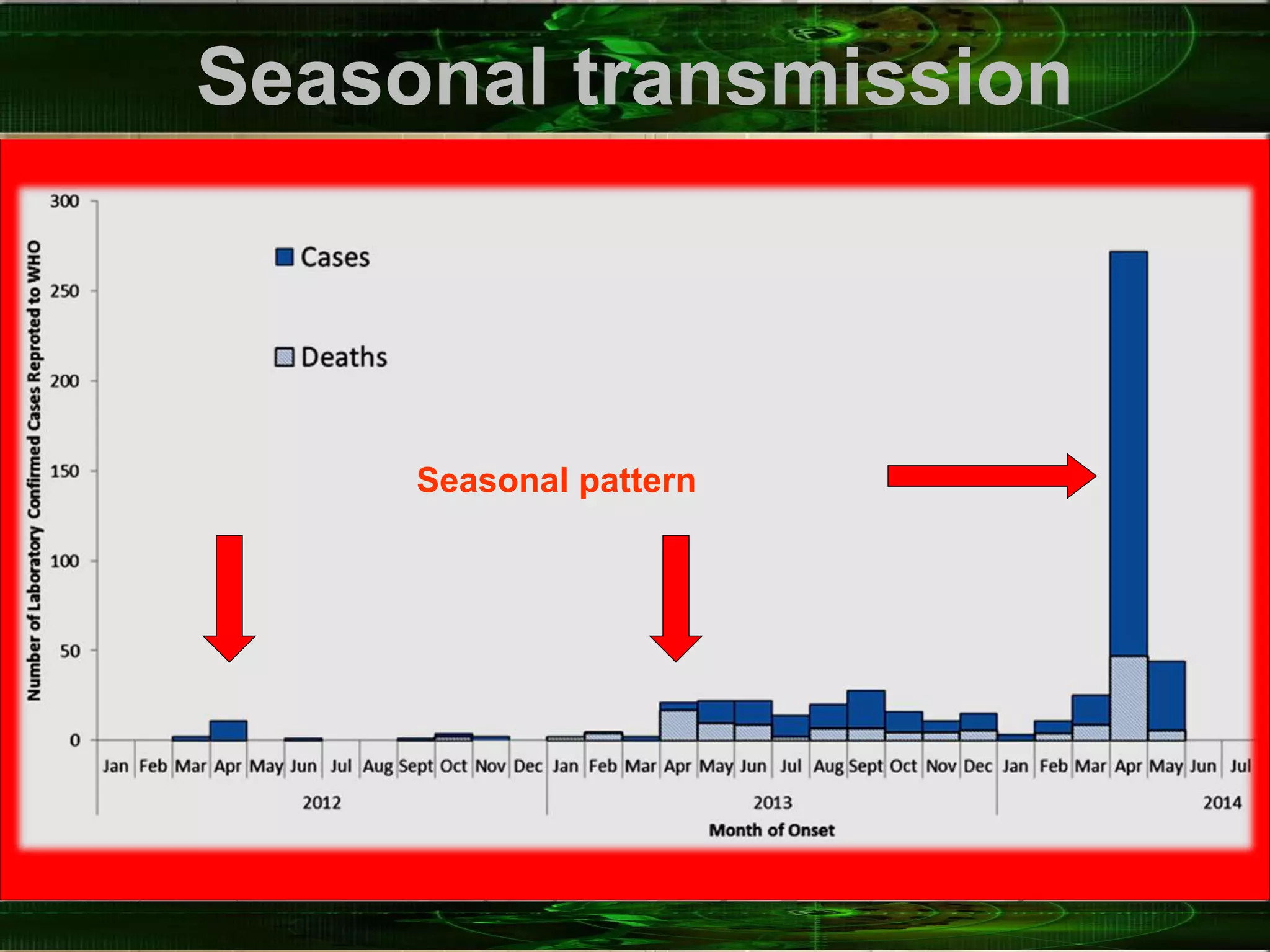
Coronaviruses are enveloped RNA viruses that appear under the microscope as having crown-like projections. The common cold is associated with several viruses including some human coronaviruses. MERS-CoV was first identified in 2012 in Saudi Arabia and has an incubation period of 2-14 days. MERS-CoV causes symptoms such as fever, cough and shortness of breath, and in some cases can cause pneumonia, kidney failure and death. Since 2012 there have been over 800 cases of MERS-CoV including many in Saudi Arabia and the UAE.