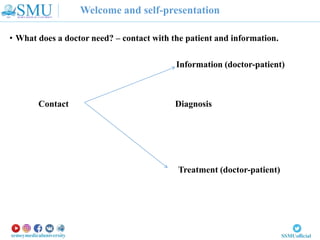
The medical interview document outlines the structure and goals of a medical interview between a doctor and patient. The interview includes gathering information about the patient's complaints, medical history, and life history to make an accurate diagnosis and treatment plan. It discusses the importance of establishing rapport, actively listening to understand the patient's perspective, and providing information to the patient in an understandable way. The doctor aims to understand the patient's health concerns and ensure informed consent during the medical interview process.