The document discusses hypothyroidism, including its causes, signs and symptoms, diagnosis, and treatment. Some key points:
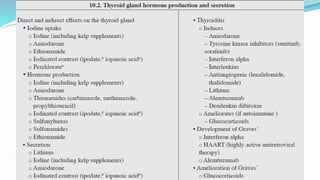
- Primary hypothyroidism is caused by failure of the thyroid gland and accounts for 99% of cases. Secondary hypothyroidism is caused by pituitary failure.
- Hashimoto's thyroiditis is the most common cause of hypothyroidism in iodine-sufficient areas. It is an autoimmune disorder more common in women.
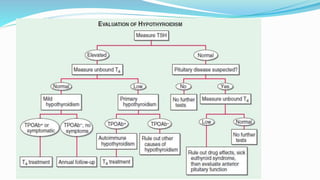
- Diagnosis is based on elevated TSH and low free T4 levels. Treatment involves daily levothyroxine replacement therapy with dosages adjusted based on follow up TSH levels.