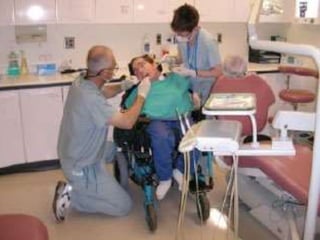
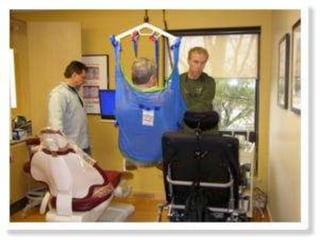
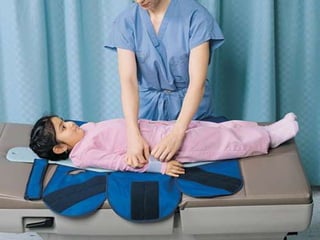
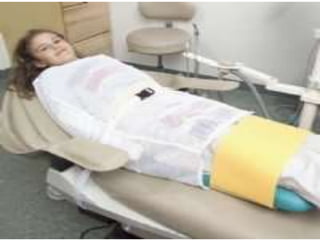
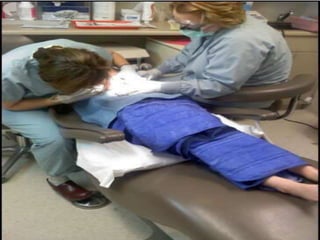
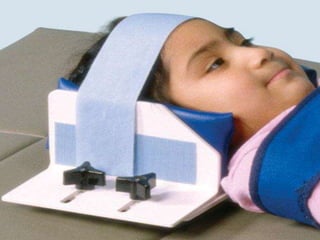
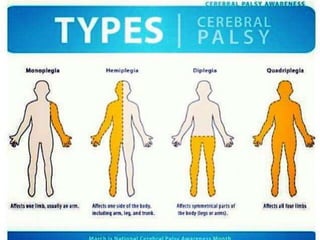
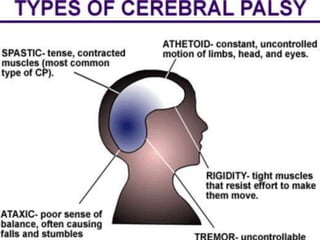
Children with disabilities and special health care needs present unique challenges for dental care. They often experience poorer oral health than others due to limited access to care, difficulties with home care, and disability-related factors. Providing care requires special preparation and modifications including protective stabilization, treatment plan alterations, desensitization to dental equipment, and management of anxiety. Common conditions discussed that impact oral health are intellectual disabilities, Down syndrome, autism, and fetal alcohol spectrum disorder.

![World Health Organization [WHO]
A handicapped person as one who over an appreciable
period is prevented by physical or mental conditions from
full participation in the normal activities of their age
groups including those of a social, recreational,
educational and vocational nature.
Children with disabilities have poorer oral health than
their nondisabled counterparts.
Variable access to dental care, inadequate oral hygiene
and disability-related factors are the causes.](https://image.slidesharecdn.com/handicappedchildppt1-220319073030/85/Handicapped-child-Dr-REENA-EPHRAIM-2-320.jpg)



![• World Health Organization [WHO]
• A handicapped person as one who over an appreciable
period is prevented by physical or mental conditions
from full participation in the normal activities of their
age groups including those of a social, recreational,
educational and vocational nature.
• Children with disabilities have poorer oral health than
their nondisabled counterparts.
• Variable access to dental care, inadequate oral hygiene
and disability-related factors are the causes.](https://image.slidesharecdn.com/handicappedchildppt1-220319073030/85/Handicapped-child-Dr-REENA-EPHRAIM-6-320.jpg)