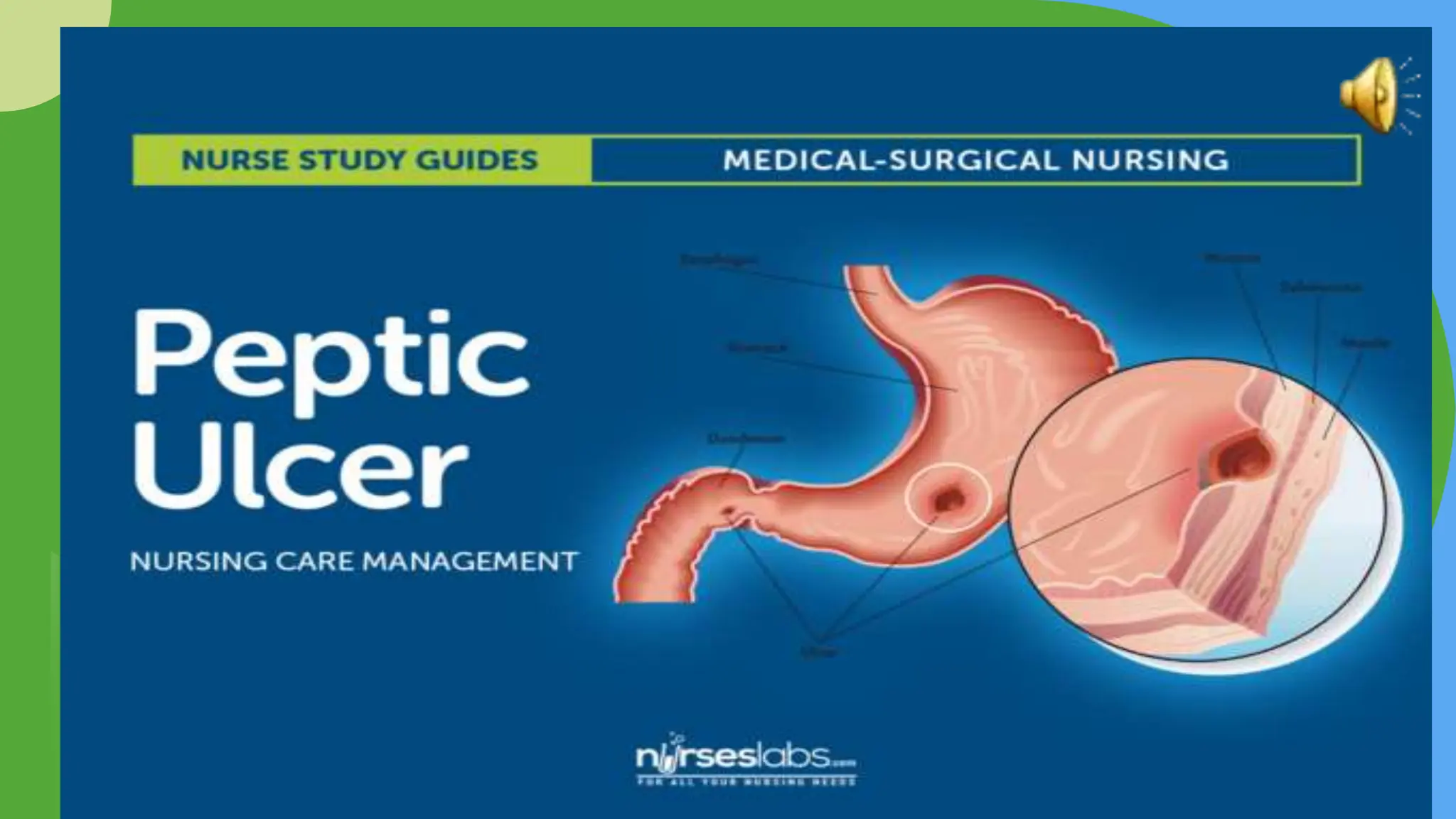
This document provides a lecture on gastritis and peptic ulcer disease. It outlines 11 nursing diagnoses related to these conditions, including pain, impaired nutrition, risk for dehydration, deficient knowledge, anxiety, risk of bleeding, activity intolerance, electrolyte imbalances, risk of infection, risk of perforation, and risk of pyloric obstruction. For each diagnosis, goals of care and interventions are described, such as pain management, dietary changes, fluid monitoring, education, and collaboration with medical teams for treatment.