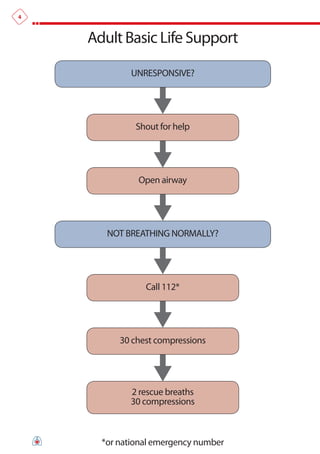
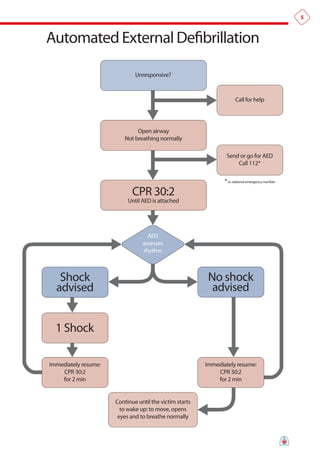
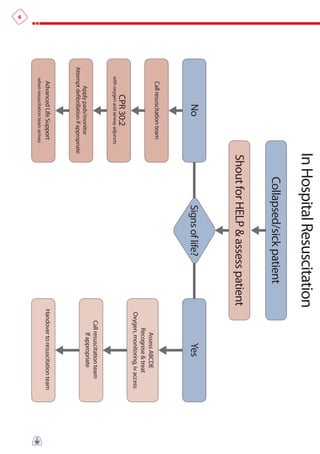
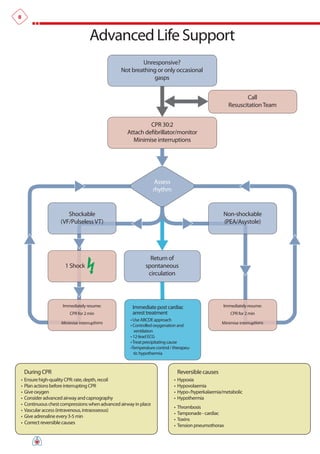
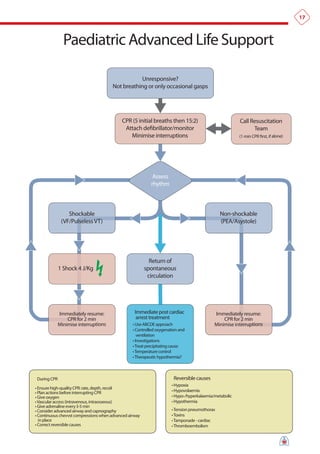
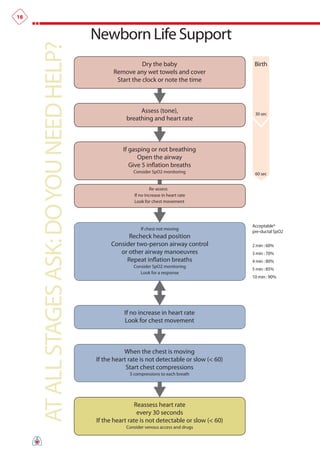
The document summarizes the main changes in resuscitation guidelines from 2010 compared to 2005. Key changes include an increased focus on high-quality chest compressions with minimal interruptions, continuing compressions when charging a defibrillator to reduce delays, and removing recommendations for a specified period of CPR before defibrillation for unwitnessed arrests. The guidelines emphasize the importance of early defibrillation and avoiding long pause times both before and after shocks.