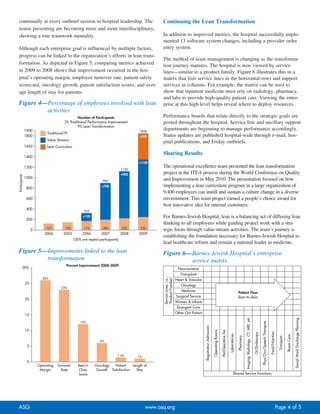
Barnes-Jewish Hospital implemented an organization-wide lean curriculum to teach lean methodology to all employees. This was done to address the issue of improving processes across the entire hospital rather than just in isolated areas or departments. The curriculum combines an education program for all employees with focused process improvements in specific value streams. As a result of the hospital's lean transformation, it has seen improved operating margins, lower employee turnover rates, and higher patient satisfaction scores. Barnes-Jewish Hospital was also named a finalist for the 2009-2010 International Team Excellence Award for its lean process improvements.