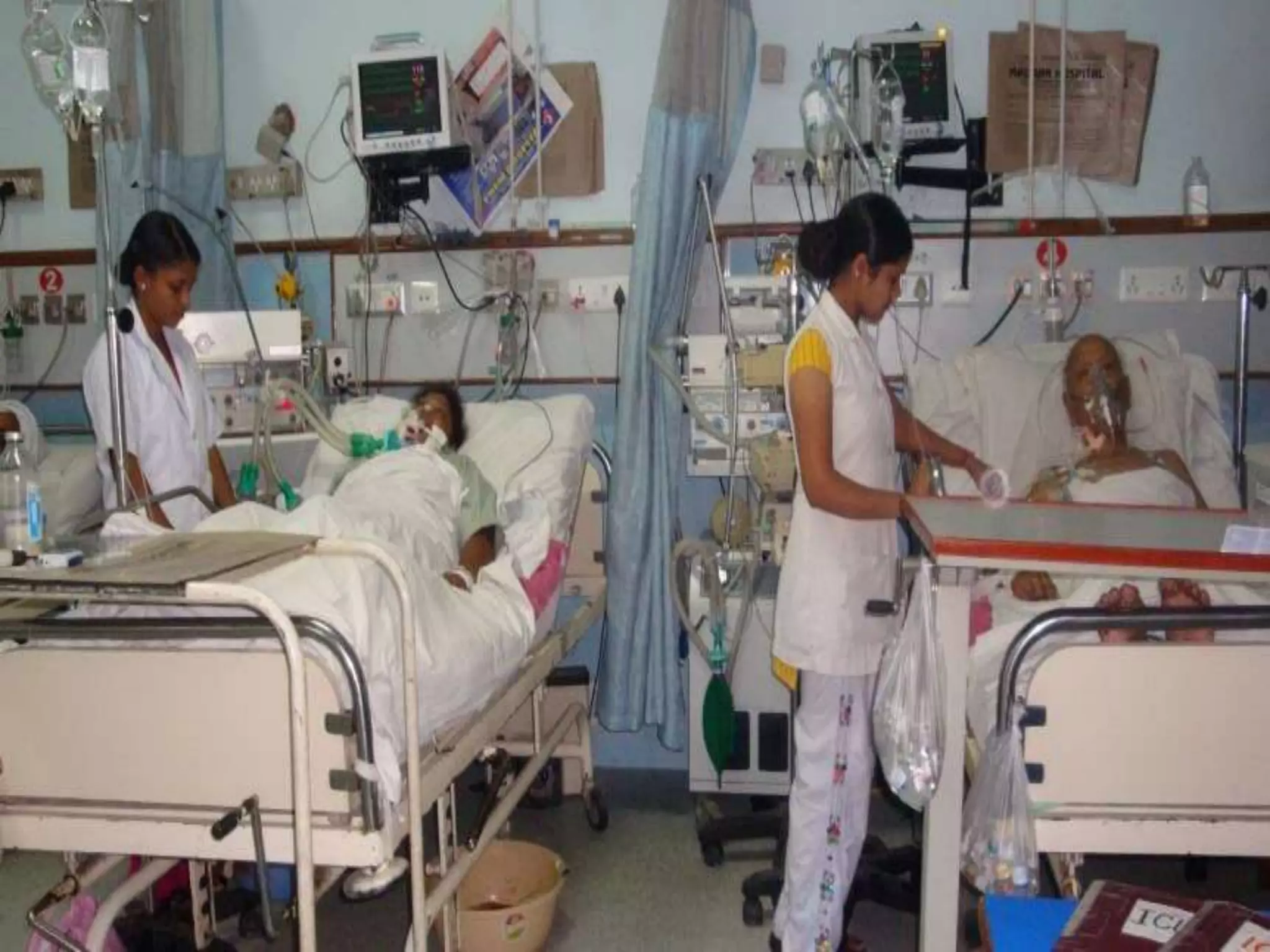
Telemetry allows for remote cardiac monitoring of patients who do not require intensive care unit placement but still need monitoring. It transmits data from a patient's heart to monitoring staff while allowing the patient mobility. An ideal intensive care unit environment focuses on reducing stress for patients through access to natural light, views, family involvement, and other therapeutic elements. Laboratory tests aim to be precise, accurate, sensitive and specific to reliably determine medical conditions and distinguish those with a condition from those without.