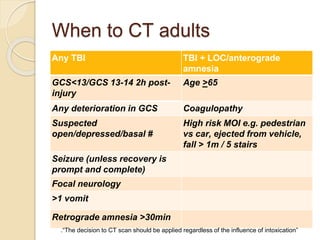
This document summarizes guidelines for head CT scans in adults and children presenting to the emergency department with head trauma. It outlines criteria for when to CT scan based on factors like Glasgow Coma Scale score, loss of consciousness, age, mechanism of injury, vomiting, and neurological symptoms. It also provides recommendations for when to perform a repeat CT scan if symptoms worsen or change. The guidelines aim to identify clinically significant traumatic brain injuries requiring intervention while avoiding unnecessary radiation exposure from CT scans.