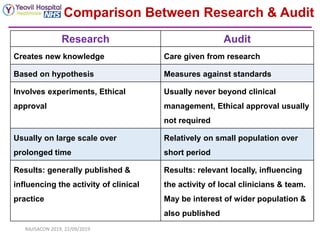
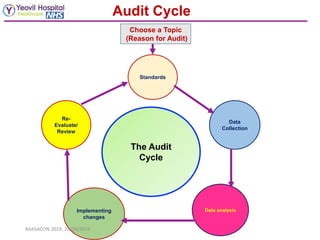
The document discusses creating effective clinical audits. It defines clinical audit as a quality improvement process that systematically reviews patient care against criteria to improve outcomes. The importance of clinical audits is described as helping to improve quality of care, reduce errors and costs, develop guidelines, and enhance education. Key differences between clinical audits and research are provided. The six stages of the clinical audit cycle are outlined as choosing a topic, setting standards, collecting data, analyzing performance against standards, implementing changes if needed, and re-evaluating to sustain improvements.