Cranial nerve problems
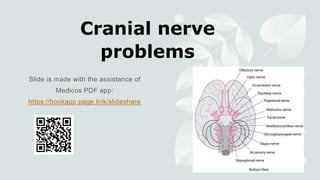
- 2. Neuroanatomy In simple terms, the cranial nerve nuclei are in 4 groups: Cortex: CN1 (olfactory bulb), CN2 (occipital lobe). Midbrain: CN3-4. Pons: CN5-8. Medulla (aka 'bulb'): CN9-12.
- 3. Upper motor neuron cranial nerve lesions Pathophysiology Lesions of the cortex or corticobulbar tract. The corticobulbar tract supplies all the cranial nerves (except 3, 4, 6) on its way to the medulla. Signs and symptoms In general, UMN cranial nerve lesions do not result in a significant deficit as supply to most CN nuclei is bilateral, though contralateral supply is often stronger. The exception is supply to the lower half of CN7, as there is only a contralateral supply. A cortical lesion thus leads to: Contralateral loss of lower facial muscles: mouth droop (and relatively raised on the lesion side) and loss of nasolabial folds. Upper half unaffected: eyes can close, brows can furrow. Causes: stroke, space occupying lesion, MS, HIV, syphilis.
- 5. Lower motor neuron cranial nerve lesions Pathophysiology Lesions of the CN nuclei or nerve fibres. Leads to an ipsilateral loss of function. Due to compression (e.g. tumour, aneurysm, trauma) or intrinsic disease (e.g. ischaemia, inflammation). These are more likely to be clinically apparent than UMN lesions of the cranial nerves. Thus when cranial nerve lesions are talked about in general, it usually refers to these LMN deficits.
- 6. Presentation The commoner lesions, 3, 4, 6, and 7, are described separately. CN5 lesions Reduced facial sensation. CN8 lesions Deaf and dizzy. CN9, 10, and 12 lesions Bulbar palsy. Dysarthria, dysphagia. See speech problems. CN10 lesions Uvula deviates to unaffected side when saying "ah" Impaired gag reflex. CN11 lesions Decreased strength in neck and shoulders. CN12 lesions Tongue protrudes towards lesion side.
- 7. Cranial nerve 3, 4, and 6 lesions Neuroanatomy Eye muscles: Horizontal movement: lateral rectus abducts, medial rectus adducts. Vertical movement: the superior rectus looks up and out, the inferior rectus looks down and out. The obliques look towards the nose, and work with the inferior/superior rectus to look straight up or straight down. Confusingly, the superior oblique looks down, and the inferior oblique looks up. So, up gaze is superior rectus plus inferior oblique, while down gaze is inferior rectus plus superior oblique. Nerves: CN6 moves lateral rectus, CN4 moves superior oblique, and CN3 moves all others: LR6SO4AO3. CN3 also controls pupil diameter and supplies the levator palpebrae superioris, which lifts the eyelid.
- 8. Causes CN3 lesions Intrinsic: Ischaemia due to diabetes (microvascular) is the commonest cause in adults. Can also be due to temporal arteritis. : Posterior communicating artery aneurysm coExtrinsicmpression. Presents with headache, and may be a sign of impending rupture and sub-arachnoid haemorrhage. Uncal (transtentorial) herniation due to ↑ICP, as CN3 passes just medially to the uncus (medial temporal lobe). A false localising sign. Cavernous sinus lesion (tumour, aneurysm): usually affects CN4, CN51, and CN6 too. The carotid sinuses are venous structures next to the sella turcica, containing cranial nerves and the carotid artery and its sympathetic plexus. CN4 lesions Isolated CN4 lesions are extremely rare. CN6 lesions Can be false localising, as it is commonly affected by ↑ICP due to its tortuous path. Multiple sclerosis, though a CNS disease, can sometimes cause LMN cranial nerve lesions due to brainstem effects. Most commonly CN6.
- 9. Other causes of eye muscle dysfunction Myasthenia gravis: NMJ lesion. Pupil sparing. Intranuclear ophthalmoplegia: medial longitudinal fasciculus lesion. CN3 impairment on conjugate gaze, but normal function during convergence. Chronic progressive external ophthalmoplegia (CPEO): mitochondrial myopathy. Ophthalmoplegia in thyroid eye disease.
- 10. Presentation General features of eye muscle weakness: Diplopia Impaired eye movement (paralytic squint). CN3 lesion: Eye looks down and out, ptosis, dilated pupil. Reduced pupillary and accommodation reflexes. Compressive causes tend to cause mydriasis, as the parasympathetic fibres are peripheral on the nerve, while intrinsic disease (e.g. ischaemia) is usually pupil sparing. Classified as complete or partial, depending on severity. If 2 adjacent nerves are affected, it could be due to compression. Otherwise, if ≥2 CNs are affected: With nystagmus = CNS. Without nystagmus = myasthenia gravis or myopathy (e.g. CPEO). Check for fatigability to differentiate, by having them hold eye in upward gaze.
- 11. Describing lesions Don't assume that every problem is a nerve palsy. Eye movements depend on the frontal eye fields ('supranuclear'), the nucleus and tracts in the brainstem, the nerve fibres, the NMJ, and the eye muscle. And nerve problems could be intrinsic to the nerve, or due to compression e.g. vascular, tumour. So when an abnormality is found, say what you see e.g. if they can't abduct on the left, it's a left lateral rectus problem, but not necessarily a left CN6 problem.
- 12. Cranial nerve 7 lesions Presentation Weak muscles of facial expression, including the upper half. Reduced taste on anterior tongue. Reduced corneal and blink reflexes. Causes Idiopathic (Bell's palsy): Acute onset, hours-days. Treat with prednisolone if patient presents in first 72 hours. Consider combining with an antiviral (aciclovir, valaciclovir, or famciclovir), which probably helps. Most recover fully within weeks-months. Intrinsic: Infection: VZV (Ramsay-Hunt syndrome type 2 aka herpes zoster oticus), otitis media, Lyme, HSV. Inflammatory: sarcoidosis, Guillain Barré, MS, Sjogren's. Extrinsic: Trauma Tumour: parotid gland carcinoma, cholesteatoma, acoustic neuroma. Do otoscopy to check for the latter two in anyone with CN7 palsy.