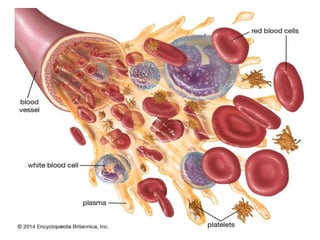
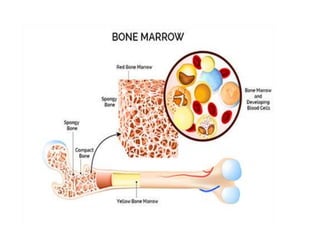
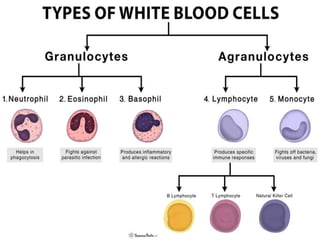
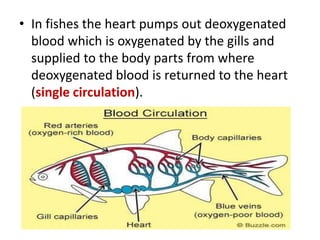
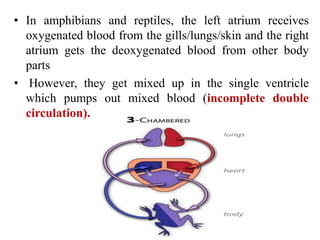
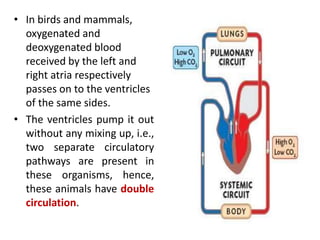
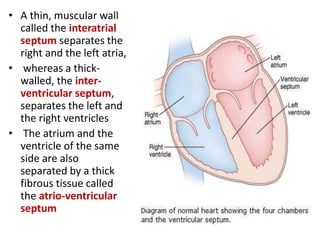
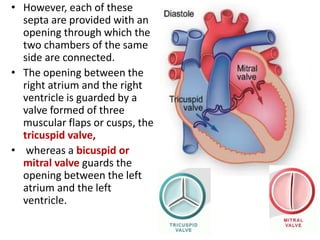
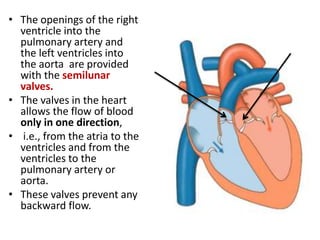
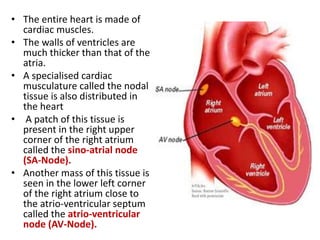
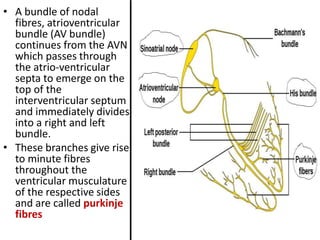
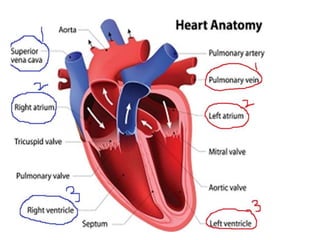
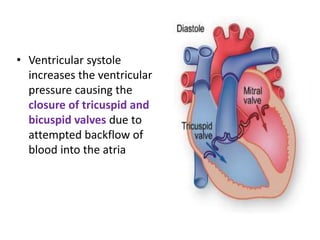
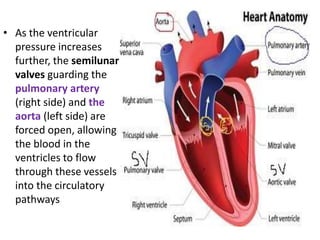
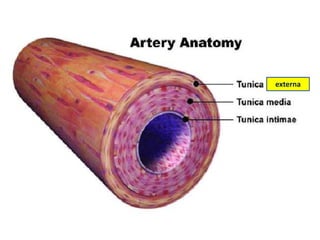
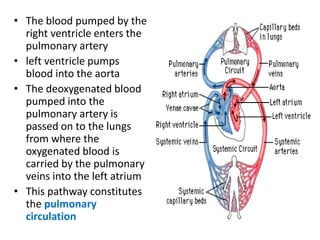
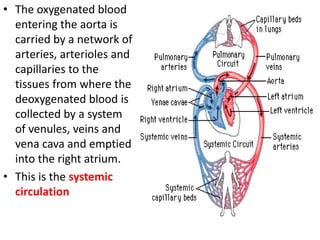
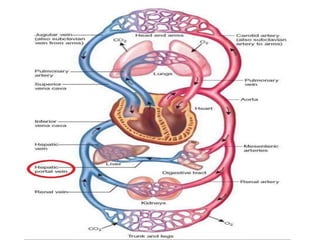
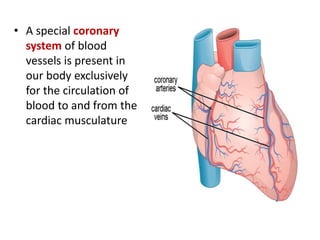
This document discusses the circulatory system in humans. It begins by explaining that blood and lymph are the two main circulatory fluids in the body, with blood being carried in a closed circulatory system of blood vessels and lymph being transported through the lymphatic system. It then describes the components of blood in detail. Next, it explains the structure and functioning of the human heart, including the cardiac cycle. It notes that the heart has four chambers and is able to efficiently circulate blood through a double circulation pathway to the lungs and body.