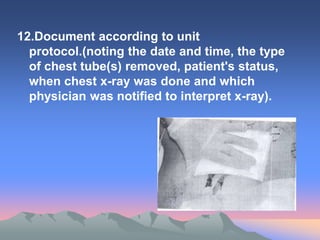
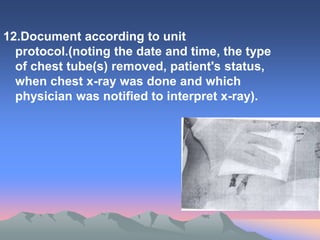
A chest tube is a flexible plastic catheter inserted through the chest wall to drain air, blood, or fluid from the pleural space surrounding the lungs. It connects to a chest drainage unit which uses water seals and suction to remove drainage. Chest tubes are used to treat pneumothoraces, hemothoraces, pleural effusions, and other chest conditions. Nurses must carefully monitor the tube, drainage system, and patient for complications and ensure proper positioning, dressing changes, and drainage assessment.