This document discusses atopic dermatitis (eczema), including its definition, epidemiology, risk factors, pathogenesis, clinical manifestations, and variants. Atopic dermatitis is a chronic inflammatory skin disease characterized by dry, itchy skin and often associated with elevated IgE levels and family history of atopy. Genetic and environmental factors contribute to its development. Clinically it presents differently based on age, from rashes on cheeks/scalp in infants to flexural lichenified plaques in older children/adults. Associated features include palmar hyperlinearity and infra-auricular fissuring.

![EPIDEMIOLOGY
Prevalence and incidence — Atopic dermatitis affects
approximately 5 to over 20 percent of children worldwide,
with large variations among countries and ethnic groups
[4,5]. Countries in Africa, Oceania, and the Asia-Pacific
region have higher rates of atopic dermatitis than
countries in the Indian subcontinent and Northern/Eastern
Europe [5]. In the United States, the overall prevalence is
approximately 16 percent, with the highest rates reported
in African American children (19 percent
Data on the prevalence of atopic dermatitis in adults are
limited.](https://image.slidesharecdn.com/atopicdermatitis-240216054026-3bd78aba/75/Atopic-Dermatitis-Atopic-Dermatitis-Atopic-3-2048.jpg)
![Risk factors
multiple genetic and environmental factors:
●Genetic risk factors – A family history of atopy (eczema, asthma, or
allergic rhinitis) is the strongest risk factor for atopic dermatitis
Approximately 70 percent of patients have a positive family history of
atopic diseases. Children with one atopic parent have a two- to
threefold increased risk of developing atopic dermatitis, and the risk
increases to three- to fivefold if both parents are atopic [Loss-of-
function variants in the FLG gene, resulting in defective epidermal
barrier, are a major risk factor for atopic dermatitis and other skin and
allergic diseases, including allergic contact dermatitis, asthma, and
food allergy. Multiple other genes have been proposed as potential
contributors to the risk of atopic dermatitis, including genes involved
in the regulation of innate host defenses and T cell function [21]](https://image.slidesharecdn.com/atopicdermatitis-240216054026-3bd78aba/75/Atopic-Dermatitis-Atopic-Dermatitis-Atopic-4-2048.jpg)



![PathoPHiziology
Other factors that can result in skin barrier
breakdown include:
Imbalance between stratum corneum protease
(eg, kallikrein, stratum corneum chymotryptic
enzyme) and antiprotease activity (eg,
lymphoepithelial Kazal-type related inhibitor
[LEKTI]).
•Abnormalities of the tight junction function.
Tight junctions are located in the granular layer of
the epidermis below the stratum corneum
and are thought to seal the intercellular space to
prevent the free diffusion of macromolecules .
Defective tight junctions may contribute to skin
barrier impairment.
•Microbial colonization and release of
proinflammatory cytokines
•Inflammatory cytokines, such as interleukin (IL)](https://image.slidesharecdn.com/atopicdermatitis-240216054026-3bd78aba/75/Atopic-Dermatitis-Atopic-Dermatitis-Atopic-8-2048.jpg)







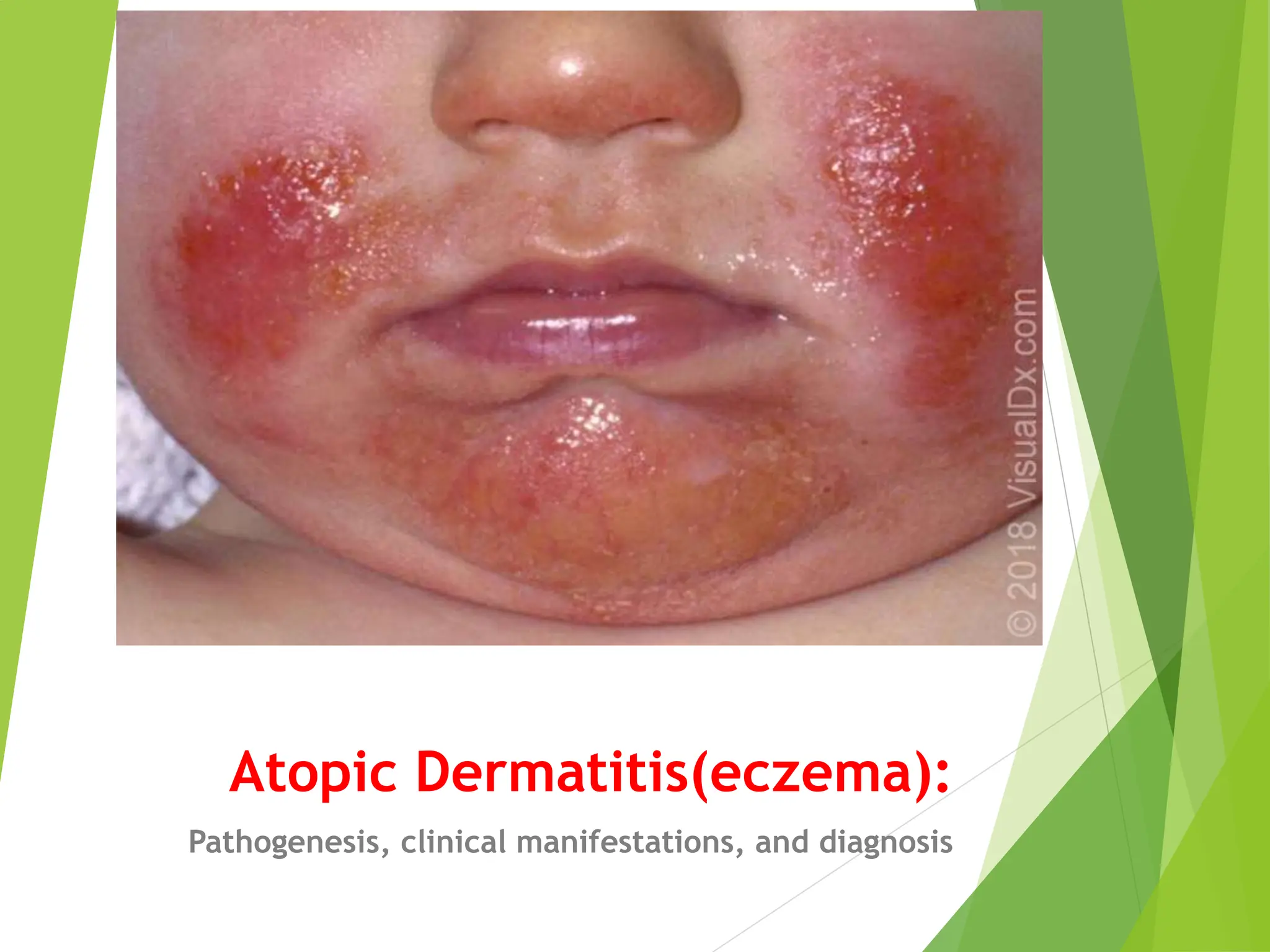
![CLINICAL MANIFESTATIONS
in infants and young children (zero to two years), atopic
dermatitis typically presents with pruritic, red, scaly,
and crusted lesions on the extensor surfaces and cheeks
or scalp (picture 4A-E) but may be diffuse (picture 4A,
4F). There is usually sparing of the diaper area (picture
5) [78]. Acute lesions can include vesicles, and there
can be serous exudates and crusting in severe cases.](https://image.slidesharecdn.com/atopicdermatitis-240216054026-3bd78aba/75/Atopic-Dermatitis-Atopic-Dermatitis-Atopic-16-2048.jpg)














![Diagnostic criteria
The American Academy of Dermatology criteria for the
diagnosis of atopic dermatitis include three sets of
essential, important, and associated features [2]:
●Essential features:
•Pruritus
•Eczema (acute, subacute, chronic) with typical
morphology and age-specific patterns:
-Facial, neck, and extensor involvement in infants and
children
-Current or previous flexural lesions in any age group](https://image.slidesharecdn.com/atopicdermatitis-240216054026-3bd78aba/75/Atopic-Dermatitis-Atopic-Dermatitis-Atopic-31-2048.jpg)














