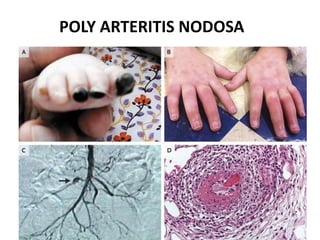
POLY ARTERITIS NODOSA POLY ARTERITIS NODOSA
- 2. CLASSIC POLYARTERITIS NODOSA • It involves purely medium vessel vasculities • It is a systemic vasculitis characterized by necrotizing inflammatory lesions ,preferentially at vessel bifurcation resulting in microaneyrysm formation,aneurysmal rupture with hemorrhage,thrombosis,and,consequently,organ ischemia or infarction. EPIDEMIOLOGY • PAN is a rare disorder • With an incidence of about 3 to 4.5 cases per 100,000 population anually. • M=F • Seen in 4th to 6th decade also seen in young patients
- 3. PATHOPHYSIOLOGY • The exact mechanism is not known • Vascular lesions in medium-sized muscular arteries occur mainly at bifurcations and branch points . • Inflammation may start in the vessel intima and progress to include the entire arterial wall destroying the internal and external elastic lamina resulting in fibrinoid necrosis. • Aneurysm develop in the weakened vessel,carrying a subsequent risk for rupture and hemorrhage • Thrombi may develop at the site of lesions • As lesion progress,proliferation of the intima or media may result in obstruction and subsequent tissue ischemia or infarction • It spares the large vessels [the aorta and its major branches],the smallest vessels {capillaries andsmall arterioles},and the venous system • Loss of function of mutations in CER1, the gene that encodes adenosine deaminase 2 (ADA2),have ben associated with spectrum of vascular and inflammatory phenotypes that includes PAN.
- 4. HISTOLOGY • Fibrinoid necrosis in the vessel wall is present • Transmural segmental necrotizing inflammation.All stages of inflammation can be seen in a single vessel
- 5. ETIOLOGY • Hepatitis B and PAN • Hepaititis B virus {HBV} infection is strongly linked with PAN. Evidence for immune complex-induced disease is confined to HBV-related PAN;the role of immune complexes in non-HBV-related PAN remains unclear. • Impaired function of endothelial cells may be part of idiopathic PAN or a consequence of it,in HBV-PAN virus replication may directly injure the vessel wall. • Endothelial dysfunction can perpetuate the inflammation through cytokine and adhesion molecule production • There is 30:1 rule in PAN and HBV
- 6. IMPORTANT FEATURES • PAN do not present as 1. petechiae 2. Purpura 3. Vesicle 4. Bulla • But presents as 1. Nodules 2. Deep ulcers 3. gangrene
- 7. • Glomerular capillaries and DAH are not manifested instead,involvement of bronchial arteries can cause hemoptysis • No antibodies in PAN. ANCA negative • Immune complexes and granulomas are absent • It has transmural involvement with necrotising vasculitis,fibrinoid necrosis,neutrophilic infiltration. • It is focal and segmental • BAD prognosis commonly assosiated with Hep B, hairy cell leukemia, and ADA-2 deficiency
- 8. Other Associations • Varicella-zoster virus • Parvovirus B-19 • Cytomegalovirus • Human T-cell leukemia virus • Rhematoid arthritis and sjogren syndrome have been also associated with PAN
- 9. CLINICAL FEATURES • PAN is an acute multisystem disease with a relatively short prodrome (ie,weeks to months) • Constitutional and musculoskeletal system sumptoms of PAN includes • Fever • Malaise • Fatigue • Anorexia and weight loss • Myalgia • Arthralgia in large joints or less commonly arthritis
- 10. RENAL SYMPTOMS • About 60% of patients have renal involvment • Flank pain may be present • Ischemic changes in the glomeruli and renal artery vasculities can cause renal failure,hypertension or both • A small % of patients may require dialysis • SYMPTOMS • Hypertension • Costophrenic tenderness • Retroperitoneal or intraperitonial hemorrhage
- 11. CUTANEOUS SYMPTOMS • Dermatalogic symptoms are very common in PAN and about 405 of patients manifest with skin lesions including • Gangrene,nodules,cutaneous infarcts,livido reticularis • Livedo reticularis that does not blanch with active pressure • Ulcerations-Especially on lower extremities near the malleoli and calf
- 17. CNS SYMPTOMS • Cerebral arteritis ,which can cause cerebral ischemia and sub-archanoid heamorrage late presentation usually in second to third year of vasculitis • Acute or sub-acute myelopathy with paraparesis can occur at any cord level • Mononeuritis multiplex –infarction of (radial,ulnar,peroneal,sural).although nerve involvment is initially asymmetrical,the development of additional nerve lesions can cause the clinical picture to resemble symmetrical polyneurophathy • Rare less than 10% encephalopathy focal defecits strokes,seizures,and sometimes brain haemorrages PERIPHERAL NERVOUS SYSTEM SYMPTOMS : 1. Distal neurophathy 2. Cutaneous neurophathy GASTROINTESTINAL SYMPTOMS : • Abdominal pain which may be post prandial • Nausea and vomiting with or without GI bleeding • Rare and more serious complications are • Bowel infarction and perforation • Cholecystitis • Hepatic infarction • Pancreatic infarction
- 18. CARDIAC SYMPTOMS • Hypertension • Tachycardia out of proportion to fever • Pericardial friction rub • Arrythmias • Congestive heart failure OPTHALMOLOGIC SYMPTOMS • Retinal vasculitis • Retinal detachment • Cotton wool spots
- 19. DIFFERENTIAL DIAGNOSIS • Antiphospholipid syndrome • Eosinophilic granulomatasis polyangitis (churg-strauss syndrome) • Granulomatosis with polyangiitis (wegener granulomatosis) • Henoch-schonlein purpura • Small vessel vasculitis • Microscopic polyangitis
- 21. DIAGNOSIS • LAB findings ain PAN are nonspecific but can help to establish the systemic nature of the disease • Elevated ESR/C-reactive protein .These markers may be useful in evaluating some patients for active disease but do not correlate with activity in all patients • Thrombocytosis • Hepatitis B surface antigen and hepatitis C serologies • Elevated creatinine levels • Mild proteinuria • Elevated liver enzymes • Hypergammaglobulinemia • Decreased levels of complements (ie,C3,C4) • MR/CT ANGIOGRAM : microaneurysms are seen • DANGER SIGNS : abdominal pain/renal and CNS involvement
- 23. MANAGEMENT OF THE PATIENT • INVESTIGATIONS • MR-angiography • 5 FACTOR SCORE : CNS,CVS,GIT,proteinuria,sr.creatinine • ADA 2 in children : deficiency closely resembles PAN. Pure cutaneous involvement with small arteries and arterioles sparing the venules.
- 25. ACR CRITERIA PAN : 1. Weight loss >4kg 2. Livido reticularis 3. Testicular pain 4. Mononeurophathy 5. Systemic hypertension ,diastolic BP > 90 6. HbsAg 7. Aneurysm on arteriogram 8. BIOPSY: necrotising vasculitis with granulocyte and monocytes in arterial wall 9. Increase in blood urea or creatinine levels which is not related with dehydration or obstruction
- 26. TREATMENT • Immunosuppression continous to be standard therapy for PAN • Corticosteroids and cyclophosmide can prolong survival for patients with idiopathic PAN • For non-hep B patients : steroids and cyclophosphamide(response is poor) • For hep-B patients : steroids+Antiviral and plasmopheresis (PLEX). (Response is poor ) • Antiviral agents like tenofovir alaenamide is used.
- 27. PROGNOSIS Idiopsthic (non-HBV- related PAN) : • Recovery from neurological defecits due to PAN can take upto 18 months. CNS involvement carries a worse prognosis than does peripheral nerve involvement • The prognosis is markedly worse in patients with acute abdominal syndromes charecterized by extensive bowel involvement • Multiple perforations may be found,relapse are common,and the post operative course is complicated by infections and delayed healing. • The prognosisis better in patients with cutaneous PAN without systemic involvement.This disease is benign and tends to relapse HBV-related PAN : • Patients who seroconvert usually recover • Once HB-PAN goes into remission, the risk of recurrence is very low HCV-related PAN • One study found that in patients with HCV-related vasculitis, HCV PAN exhibits a more severe clinical presentation but a higher rate of clinical remission.
- 28. THANK YOU