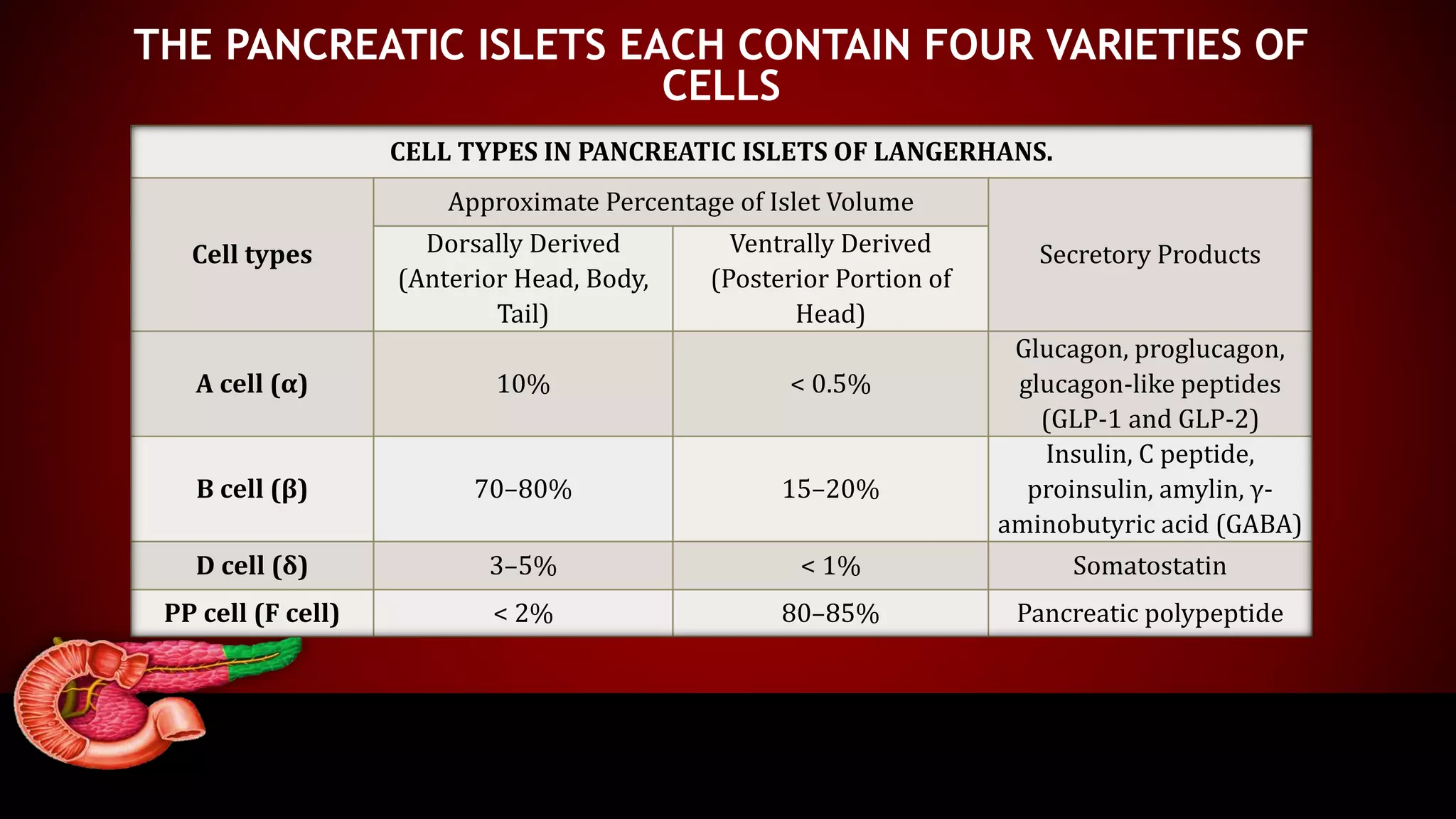
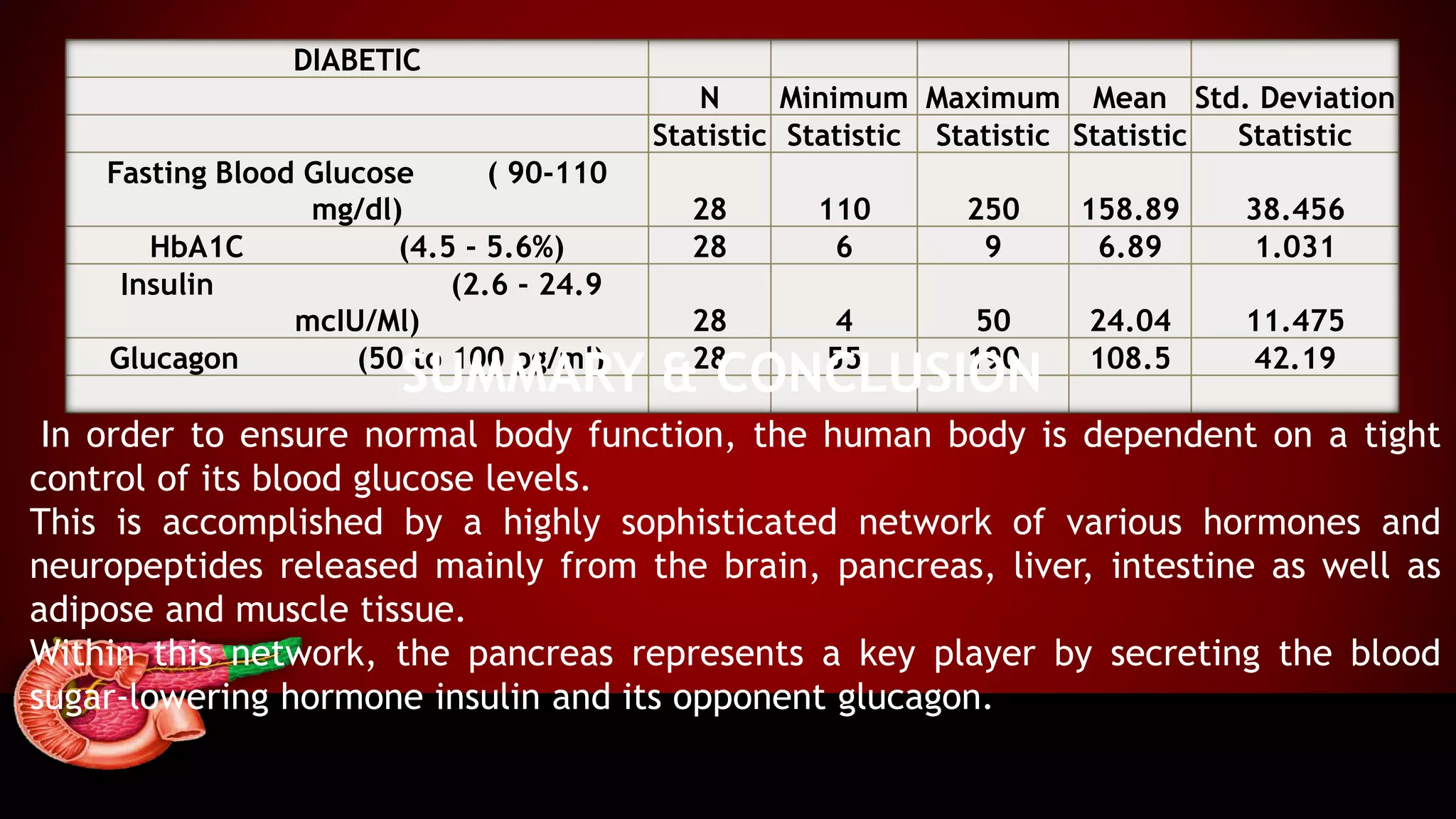
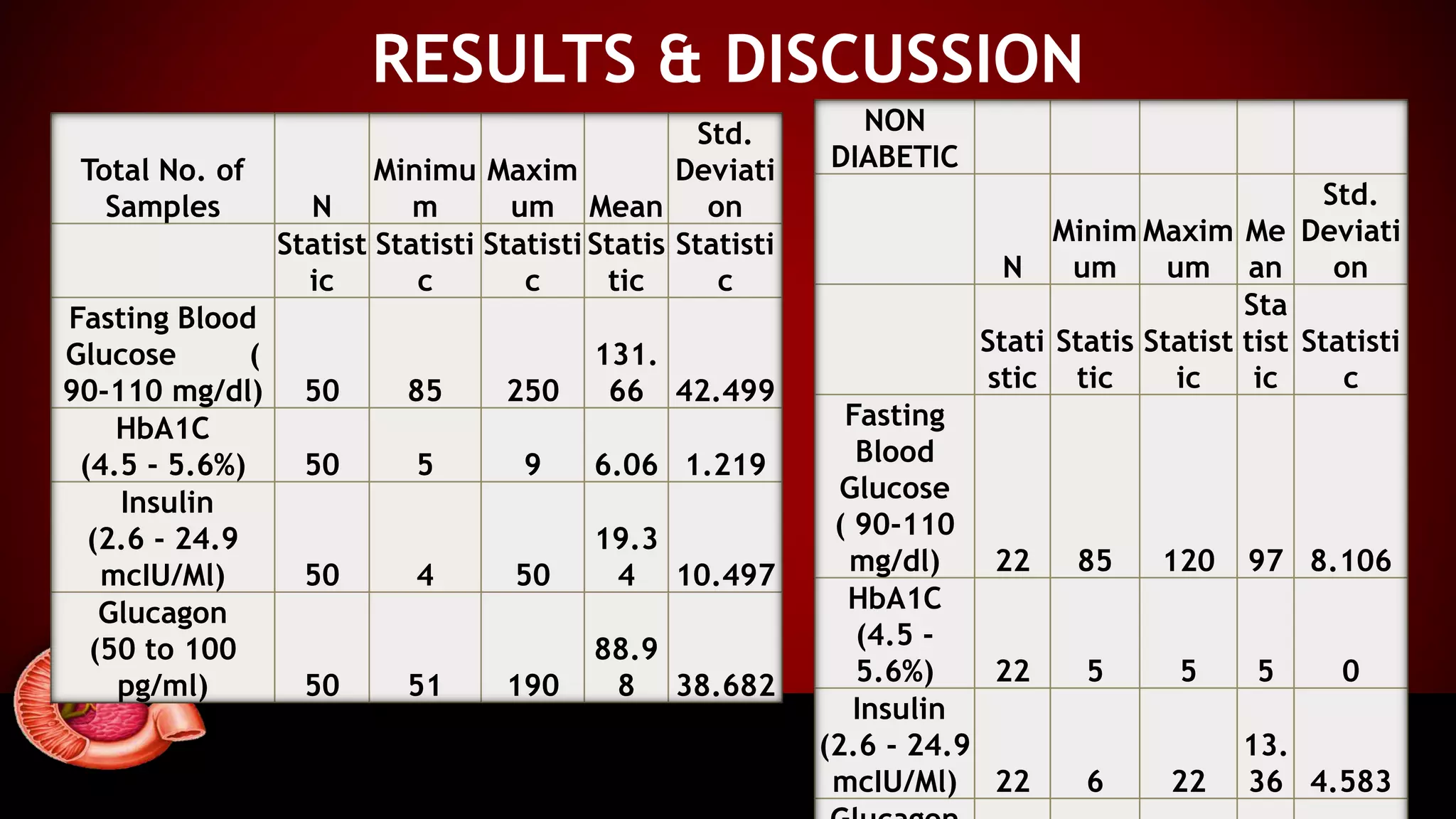
The document presents a case control study assessing pancreatic hormones in diabetic and non-diabetic patients, highlighting the critical roles of insulin and glucagon in glucose regulation. It outlines diabetes mellitus's types, symptoms, pathophysiology, and the methods used for hormonal analysis, revealing significant differences in hormone levels between diabetic and non-diabetic subjects. The conclusion emphasizes the need for targeting both insulin and glucagon abnormalities in diabetes treatment strategies.