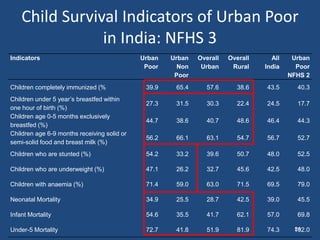
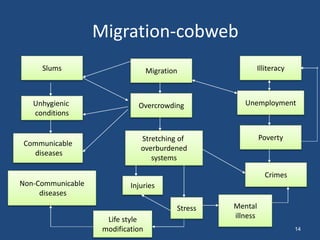
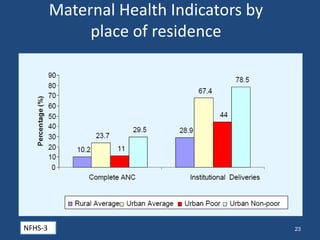
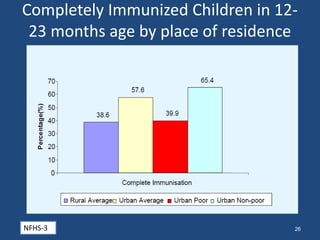
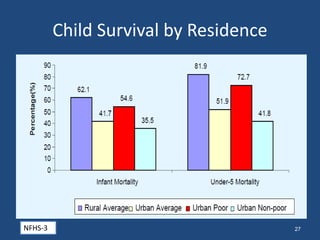
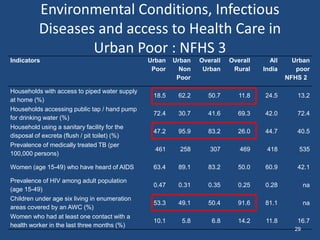
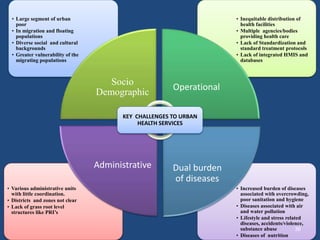
This document discusses urban health issues, challenges, and solutions in India. It notes that urbanization is increasing rapidly due to migration, leading to overcrowded slums lacking basic infrastructure. This puts urban populations at risk of communicable and non-communicable diseases. Key challenges to the health system include the dual burden of diseases, large urban poor populations, administrative issues, and operational challenges in equitably providing health services and coordinating various agencies. Proposed solutions include improving health data, inter-sectoral coordination, strengthening public-private partnerships, financing techniques, and public health facilities.