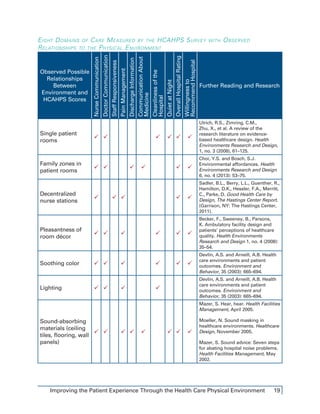
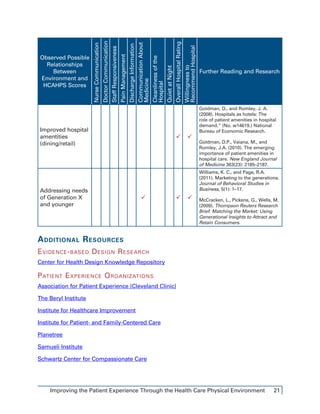
This document discusses how hospitals can improve patient satisfaction scores by taking a holistic approach involving people, processes, and place. It focuses on how the physical environment (place) influences patient experience in key areas measured by the HCAHPS survey like noise levels, pain management, and communication. Research shows noise negatively impacts sleep quality and satisfaction. Pain management is enhanced by positive distractions like views of nature. Communication is aided by quiet spaces and sink placement allowing eye contact. The document advocates a team approach across departments to identify opportunities through people's roles, care processes, and changes to the physical space. Case studies demonstrate how these factors together improved HCAHPS scores at different hospitals.