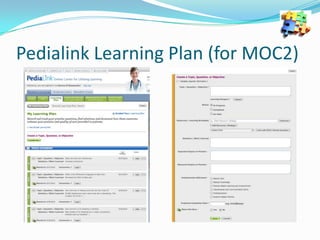
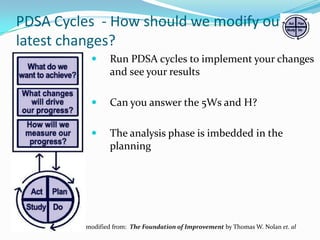
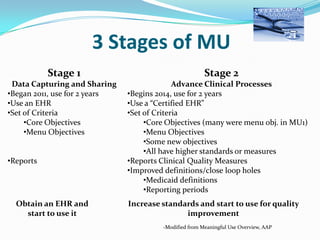
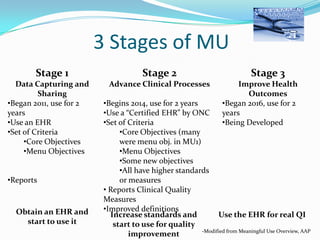
The document discusses the Maintenance of Certification (MOC) for pediatricians, detailing its components and requirements for professional competency, including quality improvement (QI) initiatives and the use of electronic health records (EHRs). It outlines the history and evolution of MOC, including the ongoing need for continuous professional development and the integration of healthcare technology to enhance patient care. The objectives include understanding how MOC, QI, and EHRs can be utilized collectively to improve pediatric practice and patient outcomes.