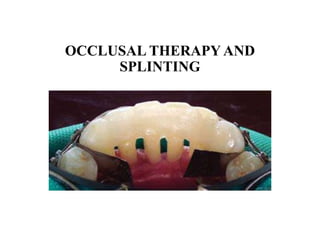
09. Splinting.pptx periodontium and health
- 4. 1. Definitions 2. Terminology 3. Early History 4. Objectives 5. Indications 6. Contraindications 7. Principles 8. Ideal Splint 9. Splintee / Splinters 10. Mode of Action 11. Classifications 12. Temporary Splints 13. Provisional Splints 14. Permanent Splints 15. Commonly Used Splints 16. Disadvantages 17. Case Reports 18. Conclusion CONTENTS
- 5. SPLINTING – Definitions “The joining of two or more teeth into a rigid unit by means of fixed or removable restorations or devices” “The joining of two or more teeth for the purpose of stabilization” -Dawson
- 7. EARLY HISTORY A Phoenician mandible from 500BC found in modern day Lebanon which has two carved ivory teeth attached to four natural teeth by gold wire Findings from digging of Egyptians (3000 -2500 B.C.) show similar gold wiring
- 8. 1. Providing rest to the supporting tissues 2. Redirection of forces 3. Redistribution of forces 4. Immediate reduction of mobility 6. Preserving arch in 7. iRestoration of functional stability 8. Psychological well being 9. Stabilizing mobile teeth during surgical, especially regenerative therapy OBJECTIVES
- 9. OBJECTIVES
- 10. INDICATIONS (Tarnow & Fletcher, 1986) 1. Stabilization of a severely periodontally compromised tooth 2. Stabilization of teeth after acute dental trauma 3. Stabilization of mobile teeth for masticatory comfort 4. Redistribution of forces along the long axis of teeth
- 11. 5. Cross arch stabilization 6. Control of forces of parafunction or bruxing 7. Stabilize teeth in secondary occlusal trauma 8. Restoration of the vertical dimension of occlusion in case of posterior bite collapse 9. Prevention of the eruption of an unopposed tooth 10. Post orthodontic retention
- 12. CONTRAINDICATIONS (Tarnow & Fletcher, 1986) 1. Moderate to severe tooth mobility in the presence of periodontal inflammation and/or primary occlusal trauma 2. Insufficient number of firm or sufficiently firm teeth to stabilize mobile teeth
- 13. 3. Prior occlusal adjustment not done on teeth with occlusal trauma or occlusal interferences 4. Patient not maintaining oral hygiene
- 14. CLINICAL FEATURES RADIOGRAPHIC FEATURES TREATMENT REQUIRED • Increased Mobility • Increased width of PDL • Normal bone height Occlusal equilibration • Increased Mobility • Increased width of PDL • Reduced bone height Occlusal equilibration • Increased Mobility • Patient NOT functioning comfortably • Normal width of PDL • Reduced bone height Occlusal equilibration ± Splinting • Increased Mobility • Patient functioning comfortably • Normal width of PDL • Reduced bone height No occlusal adjustment required
- 15. PRINCIPLES Should decrease movement 3 dimensionally Centre of rotation of the affected teeth must be located in the remaining supported bone No inflammation Minimum of 1/3rd of bony support remaining
- 16. Occlusion must be adjusted prior to stabilization Sufficient number of sound teeth should be involved Non irritating to other soft tissues Should allow for practice of oral hygiene methods
- 17. Should not impair or disturb the phonetic pattern Esthetically pleasing Crown root ratio should be considered Favorable tooth position in the arch No periapical pathology
- 18. IDEAL SPLINT (Simring & Thaller, 1956) SIMPLE ECONOMIC STABLE & EFFICIENT HYGIENIC NON-IRRITATING
- 19. IDEAL SPLINT NO INTERFERENCE WITH TREATMENT ESTHETICALLY ACCEPTABLE NO IATROGENIC DISEASE EASY CLEANSABLE EXTEND AROUND ARCH
- 20. SPLINTEE TOOTH THAT NEEDS SUPPORT SPLINTERS ADJACENT TEETH THAT PROVIDE SUPPORT
- 21. MODE OFACTION Loose teeth become stabilized Occlusal forces are better distributed Trauma minimized, repair enhanced
- 22. CLASSIFICATION OF SPLINTS PERIOD OF STABILIZATION TOOTH PREPARATION TYPE OF MATERIAL • Bonded composite resin • Braided wire • A-splints • Temporary • Provisional • Permanent • Intracoronal • Extracoronal
- 23. GOLDMAN, COHEN, & CHACKER CLASSIFICATION TEMPORARY PROVISIONAL EXTRACORONAL INTRACORONAL 1. Wire ligation 2. Orthodontic bands 3. Removable acrylic appliances 4. Removable cast appliances 5. UV light polymerizing bonding materials 1. Wire and acrylic 2. Wire and amalgam 3. Wire, amalgam and acrylic 4. Cast chrome- cobalt alloy bars with acrylic 1. All acrylic 2. Adapted metal band and acrylic
- 24. ROSS, WEISGOLD, & WRIGHT CLASSIFICATION TEMPORARY LONG TERM PROVISIONAL 1. Removable extracoronal 2. Fixed extracoronal 3. Intracoronal 4. Etched metal- resin bonded 1. Acrylic 2. Metal band & acrylic 1. Removable 2. Fixed 3. Combination of removable & fixed
- 25. FACTORS TO BE CONSIDERED Mobility patterns of the teeth to be splinted Crown to root ratio of involved teeth Status of the remaining teeth in the arch Nature and the extent of periodontal destruction Method of therapy that will be employed
- 27. Essentially a diagnostic procedure; reversible Mechanical stabilization – hypermobility reduction Method chosen – simplest, least expensive, least time consuming, esthetically acceptable, and should meet patient needs Aid in determining whether teeth with a borderline prognosis will respond to therapy
- 28. EXTRACORONAL SPLINTS 1. Wire Ligation Most common Easy to construct; sturdy Limitation – only where coronal form permits Greatest use in – mandibular incisors Hirschfield – loop tied at cervical line
- 30. 2. Orthodontic Bands Stabilize both anterior & posterior teeth Attention to the contours of the bands Contacts between teeth must be opened Acrylic over the bands Common path of insertion
- 33. 3. Removable Acrylic Appliances Dimensional instability of material may cause distortions Imperative to check these frequently & make necessary adjustments. Vital to check the path of insertion of appliance
- 34. 4. Acrylic Bite Guards (Night Guards) Treatment of bruxism and clenching Most common – covers occlusal surface of teeth For additional support – palate is covered
- 35. Maxillary Hawley Bite Plane with a labial wire Advantage – posterior teeth freed of occlusal contact Used in – anterior overbite Disarticulates posterior teeth
- 36. 5. Removable Cast Appliances Usually a rigid casting either of gold or of chrome cobalt Friedman’s variation – double continuous clasp casting One end is not joined but is left open so that the casting can be sprung over the undercuts and then ligated
- 37. The posterior end is continuous from the buccal to the lingual surface Another modification is an interlocking attachment on the distal end
- 38. 6. UV Light Polymerizing Bonding Materials Polson & Billen – "Because the materials do not polymerize until they are exposed to ultraviolet light, they provide prolonged working times for placement, shaping, and contouring over extensive areas of enamel” One popular kit – NUVA SYSTEM (Caulk, Division of Dentsply lnternational Inc. Milford, Delaware)
- 42. The composite resin splint can be strengthened by adding wire, monofilament line, fiberglass or by using a fibre meshwork to reinforce the material E.g.: RIBBOND, Ribbond Inc., Seattle, WA
- 47. Extracoronal resin-bonded retainers can strengthen the overall bonded situation The splints are usually cast from metals, usually non noble alloys Greater inherent strength than composite-resin splint Grooves, pins and parallel preparations increase retention
- 48. DIAMONDCROWN (Biodent Inc., Mont-Saint-Hilaire, QC) claims improved diametric tensile strength & bonding capabilities
- 49. INTRACORONAL SPLINTS 1. Wire Ligation Serves well for posterior teeth A channel is prepared on the labial, lingual and proximal surfaces Major disadvantage – channels may become undercuts in case crowns are needed later
- 52. 2. Wire & Acrylic (A-Splint) Obin & Arvins – wire fixed with acrylic in channels made in mobile teeth Utilized on – occlusal surfaces of posteriors and lingual surfaces of anteriors Possibility of caries or breakage Utilized more readily with anterior teeth
- 53. 3mm wide and 2mm deep channels Slight undercut Pulp protection Platinized knurled wire 22 to 16 gauge (0.64 – 1.3mm diameter) Major disadvantage – recurrent caries
- 54. Kessler’s variation of A-Splint 1 mm deep mesial and distal box is prepared parallel to long axis SnF2 or Ca(OH)2 varnish is applied and then threaded pin is placed Stainless steel wire is adapted around the pin while it passes through the slot
- 55. 3. Amalgam Splint Limited to posterior teeth Teeth prepared with sound operative principles and amalgam is condensed 2 to 5 teeth may be splinted Disadvantage – Tend to fracture easily
- 56. 4. Fixed Temporary Acrylic Bridges Used when permanent splints have to be given at a later stage With time acrylic wears and breaks Some clinicians prefer cast occlusals Some prefer metal copings (less irritating and less likely to cause caries due to cement washout)
- 57. 5. Wire & Amalgam Lloyd & Baer – continuous amalgam splint Series of mesial-occlusal-distal preparations Restored with amalgam with wire embedded in it Disadvantages - Limited to posterior teeth and possibility of fracture
- 59. 6. Wire, Resin, & Amalgam (Trachtenberg) Embed the wire in preexisting amalgam with acrylic Langeland et al – tagged acrylic in experimentally prepared cavities in monkeys
- 60. 7. Cast Chrome-Cobalt Alloy Bars Baumhammers – condensed amalgam over a 14 gauge chrome-cobalt bar Corn & Marks – cast bar fabricated on study casts prior to insertion A channel is made in the teeth to be stabilized; bar is inserted with acrylic into grooves prepared
- 64. May be used for months upto several years Usually fabricated in acrylic Stabilize a mobile dentition from initial tooth preparation to the time for permanent restorations Provide – Stability, Occlusal function, Good esthetic result
- 65. 1. All Acrylic Most common Can be fabricated chairside Limitation – marginal adaptation
- 66. 2. Adapted Metal Bands & Acrylic Amsterdam & Fox – copper / gold bands fitted and incorporated into acrylic Fulfills all objectives – exact marginal fit (caries control & pulp protection) Frequent removal is possible – added strength of metal bands
- 69. REMOVABLE FIXED CAST METAL RESIN BONDED FPDs COMBINED ENDODONTIC POSTS Continuous Clasp Devices Swing Lock Devices Overdenture Full Coverage / ¾th Crowns, Inlays Posts in Root Canals Horizontal Pin Splints Partial Dentures & Splinted Abutments Removable-Fixed Splints Full / Partial Dentures on Splinted Roots Fixed Bridges in Partial Dentures
- 70. Swing-Lock Devices Used in situations where fixed splinting is not possible or desirable Advanced age, poor physical / mental status, questionable prognosis Advantages – Conceals metal, avoids torque
- 71. Overdentures Used where few teeth with questionable prognosis remain Advantages – Favorable crown-root ratio, retention of alveolar bone around roots Disadvantage – Recurrent periodontal disease
- 72. FIXED SPLINTS Full coverage - simple Inlays – more conservative Reciprocal stabilization in all directions Palatal bar – cross arch stabilization Advantages – comfortable, esthetic
- 73. Cast Metal Resin Bonded FPDs Maryland splints Used with intact or very slightly altered enamel surfaces Advantages – functional, esthetic, reversible, economic Not suitable for – excessively mobile teeth under strong occlusal load
- 76. I. UNILATERAL SPLINTING II. BILATRAL / CROSS-ARCH SPLINTING
- 77. BILATRAL / CROSS-ARCH SPLINTING A. CONTINUOUS SPLINTS B. SEGMENT SPLINTS 1. Non Rigid Connectors 2. Soldered Joints 3. Locking Rod And Tube 4. Coping Connector
- 78. NON-RIGID CONNECTOR SOLDERLESS JOINT
- 79. LOCKING ROD & TUBE COPING CONNECTOR
- 80. COMMONLY USED SPLINTS For Anterior Teeth For Posterior Teeth 1. Wire Ligatures 2. Direct Bonding Systems 3. A-Splint 4. Variation of A-Splint 5. New Generation Bonded Reinforcing Materials with Composites 1. Intracoronal Amalgam Wire Splints 2. A-Splints 3. Bite Guards 4. Rigid Occlusal Splints 5. Composite Splints – for Severe Bruxism
- 81. J Can Dent Assoc 2000; 66: 440-443
- 82. J Can Dent Assoc 2000; 66: 440-443
- 83. Dental Traumatology 2006; 22: 345-349
- 84. J Prosthet Dent 2000; 84: 210-214
- 86. CONCLUSION Composite resin splints with fiber reinforcement BOON or BANE
- 87. REFERENCES 1. PERIODONTAL THERAPY – Henry M. Goldman & D. Walter Cohen, 6th Ed 2. PERIODONTICS IN THE TRADITION OF GOTTLIEB AND ORBAN – Grant, Stern & Listgarten, 6th Ed 3. PERIODONTAL DISEASES – Schluger, Youdelis, Page, & Johnson, 2nd Ed 4. Periodontology 2000, Vol 4, 1994, 15-22
- 88. REFERENCES 5. Compendium Aug 2001, Vol 22, No. 8, 610-620 6. J Can Dent Assoc 2000; 66: 440-443 7. J Contemp Dent Pract Nov 2002; (3) 4: 10-22 8. DCNA, Vol 43, No. 1, 1999 9. BDJ, Vol 191, No.10, Dec 8, 2001 10. Dental Traumatology 2006; 22: 345-349 11. J Prosthet Dent 2000; 84: 210-214