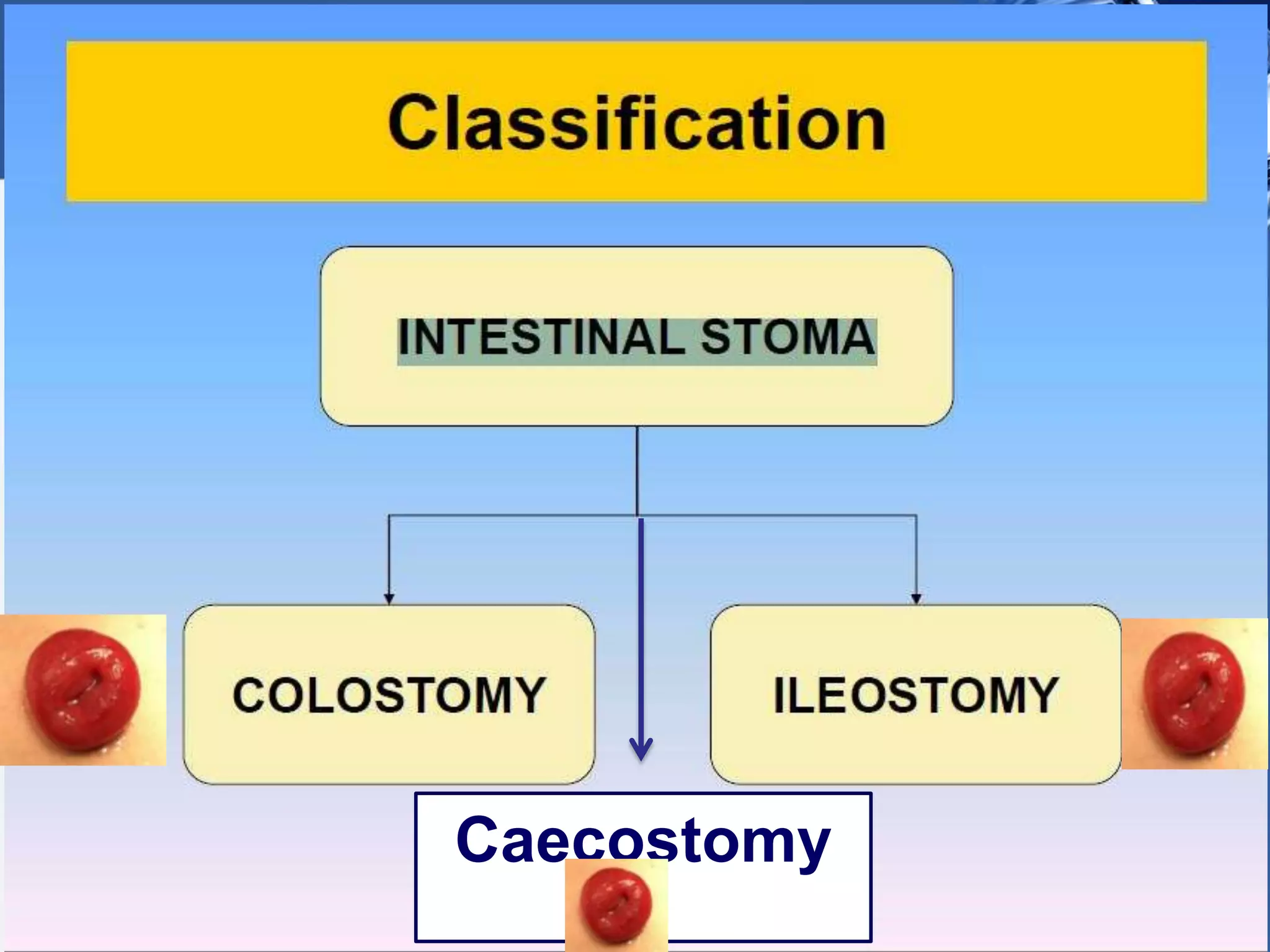
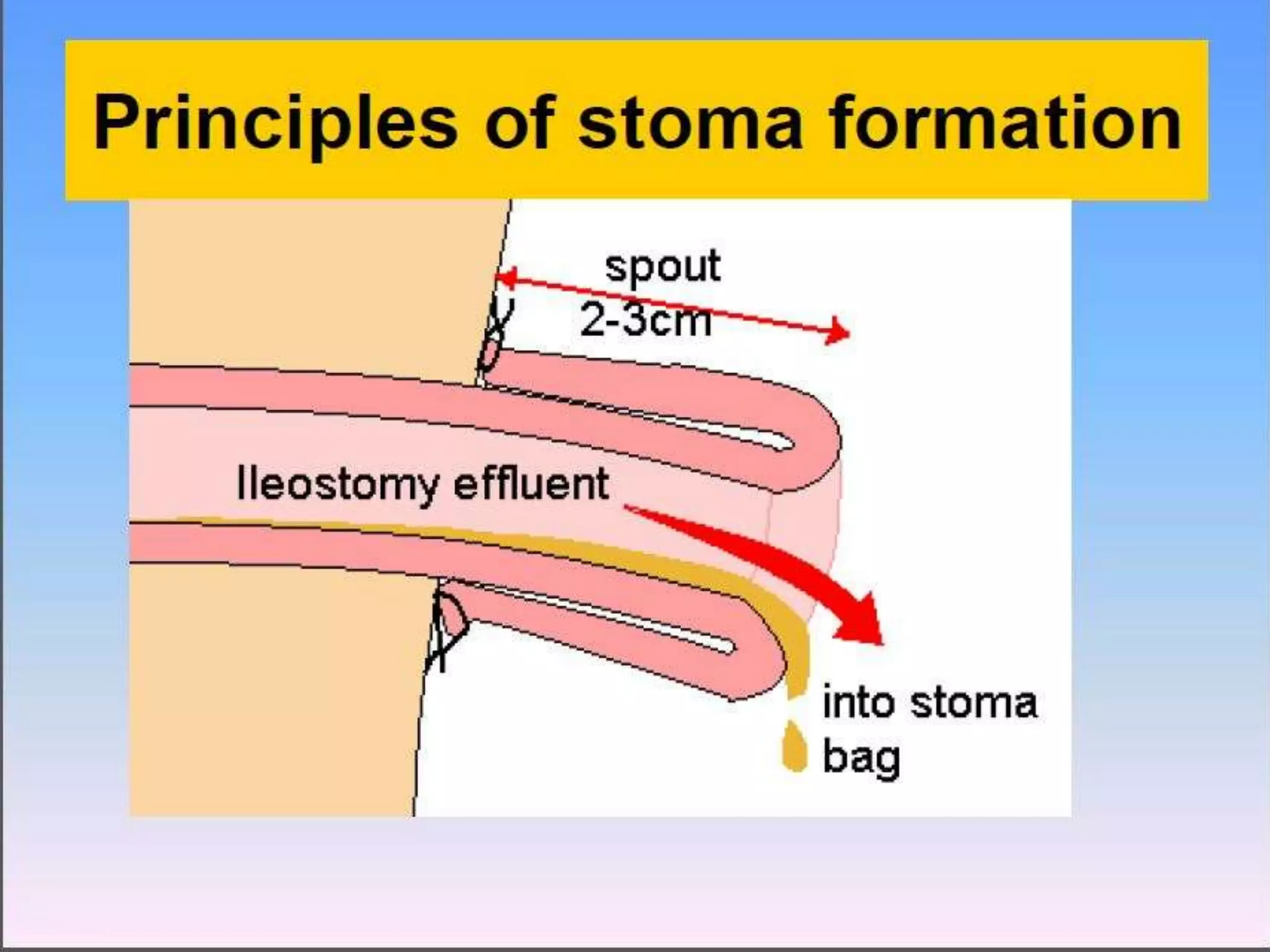
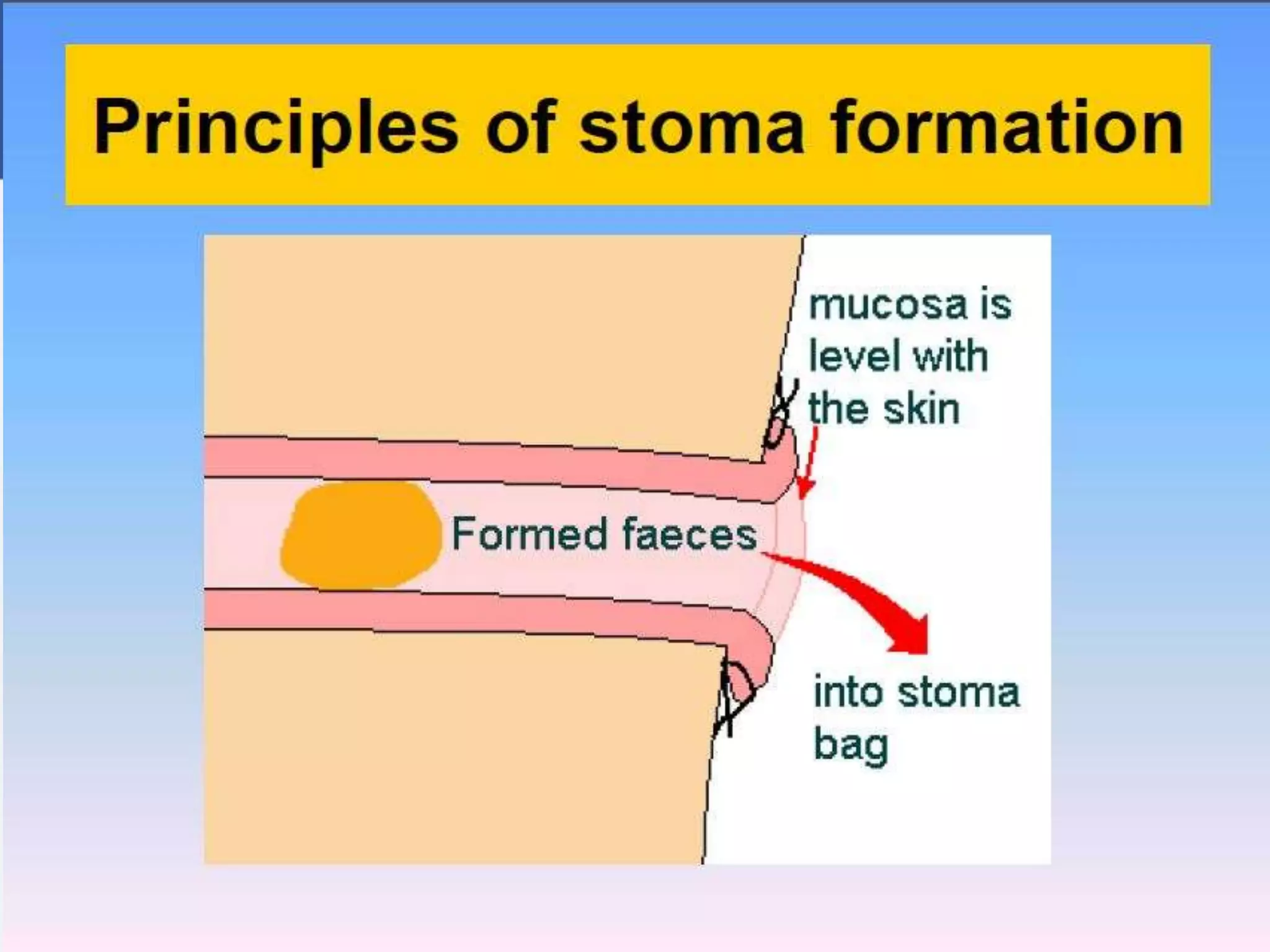
A stoma is a surgically created opening that allows stool or urine to exit the body. There are three main types - colostomy, ileostomy, and urostomy. A colostomy diverts feces, while an ileostomy diverts intestinal contents which are usually liquid. A urostomy diverts urine. Complications can include prolapse, retraction, hernia, and skin irritation. When siting a stoma, it is important to choose a well-vascularized area that is away from skin folds, scars, and bony prominences to help prevent these complications.