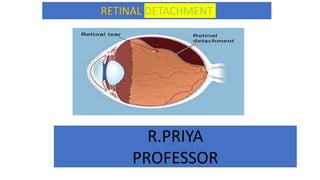
Retinal detachment
- 2. INTRODUCTION The incidence of retinal detachment in otherwise normal eyes is around 5 new cases in 100,000 persons per year. Detachment is more frequent in middle-aged or elderly populations, with rates of around 20 in 100,000 per year. The lifetime risk in normal individuals is about 1 in 300.
- 3. DEFINITION A separation of the retina from its connection at the back of the eye. The separation usually results from a tear (that is, a rent or rip, not a tear drop) in the retina, which often occurs when the vitreous gel pulls loose or separates from its attachment to the retina. Once the retina has torn, the vitreous liquid can pass through the tear and accumulate behind the retina. The build-up of fluid behind the retina is what separates (detaches) the retina from the back of the eye. Vision loss occurs if the detached retina is not repaired.
- 5. Continued with anatomy The eye is our organ of sight. The eye has a number of components which include but are not limited to the cornea ,iris ,pupil , lens ,retina , macula , optic nerve, choroid and vitreous. •Cornea: clear front window of the eye that transmits and focuses light into the eye. •Iris: colored part of the eye that helps regulate the amount of light that enters •Pupil: dark aperture in the iris that determines how much light is let into the eye •Lens: transparent structure inside the eye that focuses light rays onto the retina •Retina: nerve layer that lines the back of the eye, senses light, and creates electrical impulses that travel through the optic nerve to the brain •Macula: small central area in the retina that contains special light-sensitive cells and allows us to see fine details clearly •Optic nerve: connects the eye to the brain and carries the electrical impulses formed by the retina to the visual cortex of the brain •Vitreous: clear, jelly-like substance that fills the middle of the eye
- 6. CAUSES Age , Myopia, Cataract surgery ,Trauma ,Degenerative retinal lesions, Stickler's syndrome Juvenile X-linked retinoschisis , Marfan’s syndrome , Proliferative diabetic retinopathy , Proliferative vitreoretinopathy , Retinopathy of prematurity , Penetrating eye injury , Sickle cell retinopathy , Retinal vein occlusion Inflammatory (uveitis, scleritis),Hydrostatic (malignant hypertension, toxaemia of pregnancy), Neoplastic (choroidal melanoma, haemangioma, metastasis), Vascular (Coat’s disease, retinal macro aneurysm), Maculopathy (neovascular macular degeneration, central serous choroido retinopathy), Congenital disorders (nan ophthalmos, optic disc pit)
- 7. RISK FACTOR The following factors increase your risk of retinal detachment: •Aging — retinal detachment is more common in people over age 50 •Previous retinal detachment in one eye •Family history of retinal detachment •Extreme nearsightedness (myopia) •Previous eye surgery, such as cataract removal •Previous severe eye injury •Previous other eye disease or disorder, including retinoschisis, uveitis or thinning of the peripheral retina (lattice degeneration) •take glaucoma medications that make the pupil small (like pilocarpine) •had a serious eye injury •have weak areas in your retina (seen by an eye doctor during an exam) •Lattice degeneration (thinning along the edges of your retina) •Diabetic retinopathy (damaged blood vessels in your retina because of diabetes) •Posterior vitreous detachment (the vitreous gel in your eye pulls away from your retina)
- 8. TYPES Rhegmatogenous (reg-ma-TODGE-uh-nus). These types of retinal detachments are the most common. Rhegmatogenous detachments are caused by a hole or tear in the retina that allows fluid to pass through and collect underneath the retina, pulling the retina away from underlying tissues. The areas where the retina detaches lose their blood supply and stop working, causing you to lose vision. • The most common cause of rhegmatogenous detachment is aging. As you age, the gel-like material that fills the inside of your eye, known as the vitreous , may change in consistency and shrink or become more liquid. Normally, the vitreous separates from the surface of the retina without any complications — a common condition called posterior vitreous detachment (PVD). One complication of this separation is a tear. • As the vitreous separates or peels off the retina, it may tug on the retina with enough force to create a retinal tear. Left untreated, the liquid vitreous can pass through the tear into the space behind the retina, causing the retina to become detached. Tractional. This type of detachment can occur when scar tissue grows on the retina's surface, causing the retina to pull away from the back of the eye. Tractional detachment is typically seen in people who have poorly controlled diabetes usually because diabetes has damaged the blood vessels in the back of your eye. or other conditions. Exudative Or secondary retinal detachment or serous ratinal detachment. In this type of detachment, fluid accumulates beneath the retina, but there are no holes or tears in the retina. Exudative detachment can be caused by age-related macular degeneration, injury to the eye, tumors or inflammatory disorders.
- 10. SIGNS AND SYMPTOMS •Photopsia, or sudden, brief flashes of light outside the central part of their vision, or peripheral vision. The flashes are more likely to occur when the eye moves. •A significant increase in the number of floaters, the bits of debris in the eye that make us see things floating in front of us, usually like little strings of transparent bubbles or rods that follow our field of vision as our eyes turn. They may see what looks like a ring of hairs or floaters on the peripheral side of the vision. •A heavy feeling in the eye •A shadow that starts to appear in the peripheral vision and gradually spreads towards the center of the field of vision •A sensation that a transparent curtain is coming down over the field of vision •Straight lines start to appear curved
- 11. DIAGNOSIS A dilated eye exam is the best thing can do for eye health! It’s the only way to check for eye diseases early on, when they’re easier to treat — and before they cause vision loss. The exam is simple and painless. eye doctor will check for vision problems that make it hard to see clearly, like being nearsighted or farsighted. Then doctor will give some eye drops to dilate (widen) your pupil and check for eye diseases. Get a dilated eye exam every 1 to 2 years if you: •Are over age 60,Are African American and over age 40,Have a family history of glaucoma •If have diabetes or high blood pressure, ask your doctor how often you need an exam. Most people with diabetes or high blood pressure need to get a dilated eye exam at least once a year. A visual acuity test to check how clearly you see. Your doctor will ask you to read letters that are up close and far away. •A visual field test to check peripheral (side) vision. doctor will test how well can see objects off to the sides of your vision without moving your eyes. •An eye muscle function test to check for problems with the muscles around eyeballs. doctor will move an object around and ask you to follow it with your eyes. •A pupil response test to check how light enters eyes. doctor will shine a small flashlight into your eyes and check how your pupils react to the light. •A tonometry test to measure the pressure in your eyes. doctor will use a machine to blow a quick puff of air onto eye, or gently touch eye with a special tool. Don’t worry — it doesn’t hurt! •Dilation to check for problems with the inner parts of your eye doctor will give some eye drops to dilate (widen) your pupil. This helps the doctor see inside your eye.
- 12. SURGICAL TREATMENT When a retinal tear or hole hasn't yet progressed to detachment, eye surgeon may suggest one of the following procedures to prevent retinal detachment and preserve vision. •Laser surgery (photocoagulation). The surgeon directs a laser beam into the eye through the pupil. The laser makes burns around the retinal tear, creating scarring that usually "welds" the retina to underlying tissue. •Freezing (cryopexy). After giving you a local anesthetic to numb eye, the surgeon applies a freezing probe to the outer surface of the eye directly over the tear. The freezing causes a scar that helps secure the retina to the eye wall.
- 13. SURGICAL TREATMENT•Injecting air or gas into your eye. In this procedure, called pneumatic retinopexy (RET-ih-no-pek-see), the surgeon injects a bubble of air or gas into the center part of the eye (the vitreous cavity). If positioned properly, the bubble pushes the area of the retina containing the hole or holes against the wall of the eye, stopping the flow of fluid into the space behind the retina. doctor also uses cryopexy during the procedure to repair the retinal break. •Fluid that had collected under the retina is absorbed by itself, and the retina can then adhere to the wall of eye. may need to hold your head in a certain position for up to several days to keep the bubble in the proper position. The bubble eventually will reabsorb on its own. •Indenting the surface of your eye. This procedure, called scleral buckling, involves the surgeon sewing (suturing) a piece of silicone material to the white of your eye (sclera) over the affected area. This procedure indents the wall of the eye and relieves some of the force caused by the vitreous tugging on the retina. •If have several tears or holes or an extensive detachment, surgeon may create a scleral buckle that encircles entire eye like a belt. The buckle is placed in a way that doesn't block vision, and it usually remains in place permanently. •Draining and replacing the fluid in the eye. In this procedure, called vitrectomy, the surgeon removes the vitreous along with any tissue that is tugging on the retina. Air, gas or silicone oil is then injected into the vitreous space to help flatten the retina. •Eventually the air, gas or liquid will be absorbed, and the vitreous space will refill with body fluid. If silicone oil was used, it may be surgically removed months later. •Vitrectomy may be combined with a scleral buckling procedure. After surgery your vision may take several months to improve. You may need a second surgery for successful treatment. Some people never recover all of their lost vision.
- 14. CARE AFTER SURGERY Immediately after the operation, you can expect: •The eye will be covered with an eye pad and perhaps a protective eye shield. •May need to stay in hospital overnight or, occasionally, longer. During the post-operative period: •Eye may be uncomfortable for several weeks, particularly if a scleral buckle has been used. •Vision will be blurry – it may take some weeks or even three to six months for your vision to improve. •Eye may water. •Expect a ‘gritty’ feeling on the surface of your eye if stitches have been used. •Avoid rubbing or pressing on the eye. •May need to wear an eye pad for protection at night while your eye is healing. •Make sure to follow all directions for medications, such as eye drops. •Avoid vigorous activity for some weeks following surgery. •Obey all instructions on head positioning. •See surgeon immediately if you experience severe pain. If you have had gas inserted into eye as part of retinal re-attachment procedure, it is extremely important that do not fly until it has completely reabsorbed. This may take up to four weeks
- 15. COMPLICATION AFTER SURGERY •cataract formation (loss of clarity of the lens of the eye) •glaucoma (raised pressure in the eye) •infection •haemorrhage (bleeding) into the vitreous cavity •vision loss •loss of the eye, although with modern surgical techniques this is a very unlikely outcome.
- 16. PREVENTION • Regular routine eye examinations every year or two. These help your eye specialist to detect any changes such as inflammation, thinning or tears in the retina which could progress to retinal detachment. • Prevent eye injuries by wearing protective goggles when you are working with power tools or performing activities which involve small objects flying around (possibly into one eye). This also applies when you are using guns of any description, or participating in any type of fireworks show. in physical contact sports such as boxing, squash, or soccer, it is important to protect your eyes from a direct blow, which could lead to detachment of the retina, by wearing appropriate eye protection.
- 17. NATURAL REMEDIES FOR FLOATERSeye floaters involve many lifestyle changes. Try the following: •Eat a healthy diet full of anti-inflammatory foods. •Apply hot and cold compresses to help your eyes relax. •Gently massage your temples with your eyes closed. •Do eye exercises, such as rolling your eyes and focusing on a moving object, to build resistance to fatigue and reduce floaters. •Reduce screen time. •Wear protective glasses, such as sunglasses and computer screen glasses. •Drink lots of water to help rid the body of toxins that can lead to floaters. 1.Take a daily vitamin supplement that includes omega-3 fatty acids, beta-carotene, selenium, lutein, spirulina, chlorella, blue-green algae, and vitamins A, C, and E. eat more •Try self-acupressure. •Get good rest and allow your eyes time to relax. Herbal therapy is another natural treatment option for eye floaters. Herbal techniques to fight eye floaters include taking: •Gingko Biloba to improve circulation to the eyes. •Traditional Chinese formulations for eye health. •Grapeseed and bilberry extracts for their antioxidant properties. All of the above natural remedies are aimed at promoting eye health and reducing toxins and inflammation that can lead to eye floaters. Avoidingactivities to eye health such as too much screen time, reading in poor light, smoking, and drinking too much alcohol and caffeine, are additional steps you can take to treat your eye floaters naturally. Talk to your doctor before you begin taking any supplements. They can confirm it won’t negatively interact with any other medications you are taking.
- 18. CONT… 1.eat more blood-building foods, including fresh vegetables such as spinach and beets, and dried fruits, such as raisins, figs, and prunes. 2.Turnip tops, leeks, okra, tomatoes, lettuce, Swiss chard, cilantro, yams, carrots, cabbage, green peas, watercress, whole grains, beans (especially soybeans and mung beans), cloves, sesame seeds, and 3.Fresh fruits, including apples, peaches, pears, mulberries, blueberries, and blackberries, are all beneficial. 4.Avoid foods high in fat content, animal fats, red meat, dairy products, and spicy foods all contribute to the buildup of toxins and waste in the body and should be eliminated. 5.Avoid coffee and alcohol, which injure the yin essence.