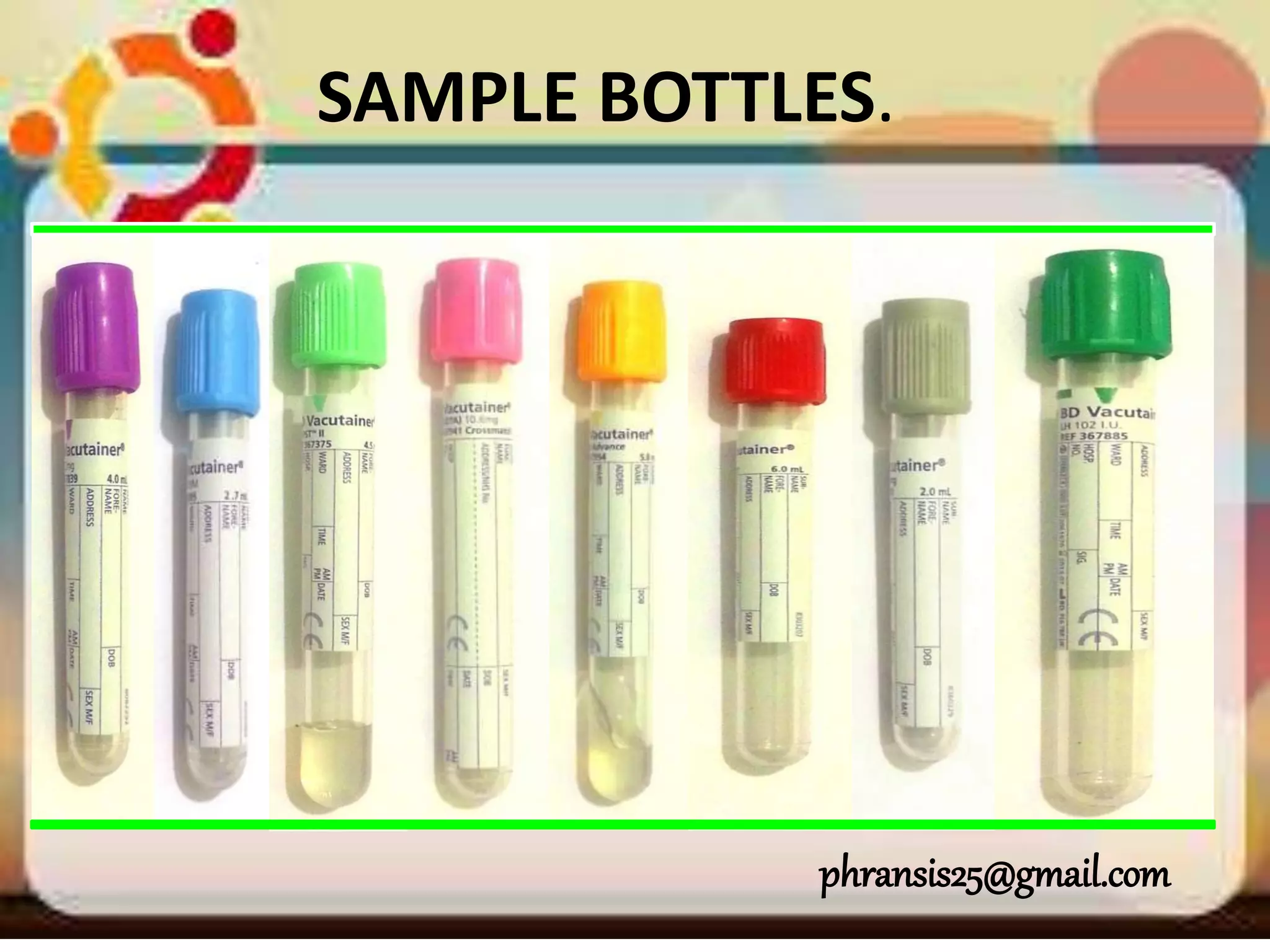
This document provides information about different colored blood collection tubes and their uses. It discusses the purposes and additives of purple, pink, blue, yellow, grey, and red tubes. The purple, pink, and blue tubes contain anticoagulants and are used for hematology and coagulation tests. The yellow, grey, and red tubes are used for biochemical and other serum-based tests. It provides examples of common tests performed using each tube type and tips for proper sample collection and handling.