Kidney Anatomy and Functions in 40 Characters
- 1. Prepared by Dr.Ismael I. Surchi
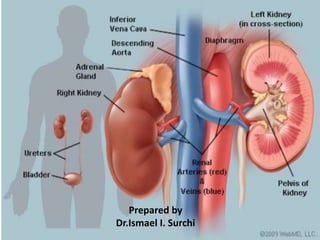
- 2. The Kidneys/Renes • Definition – The kidneys are a pair of excretory organs situated on the posterior abdominal wall, one on each side of the vertebral column, behind the peritoneum.
- 3. Location • The kidneys occupies the epigastric , hypochondriac, lumbar & umbilical regions. • Vertically they extends from upper border of twelfth thoracic vertebra to the center of the body of third lumbar vertebra. • The right kidney is slightly lower than the left, & the left kidney is little nearer to the median plane than the right.
- 4. The Kidneys- Surface Anatomy • External Features – Each kidney is bean shaped. – It has upper & lower poles, medial and lateral borders, and anterior and posterior surfaces. – The upper pole is broad & is in close contact with the corresponding suprarenal glands. – The lower pole is pointed.
- 5. • The lateral border is convex. • The medial border is concave. • The middle part of the medial border is depressed and is known as hilum (hilus) 11 cm 3cm 5cm 8
- 6. Measurements • Color • Length : Reddish Brown : About 11 cm long( the left kidney is little longer & narrower than right ) : 6cm broad : 3cm thick • Width • Thickness • Weight –Males –Females : 150gm : 135gm (In fetus the kidney is lobulated & is made up of about 12 lobules. After birth the lobules fuse , so that in adults the kidney is uniformly smooth)
- 7. Surface Marking- Morris Parallelogram Anterior aspect Posterior aspect
- 8. Coverings • It has 3 coverings 1. Innermost fibrous capsule or true capsule 2. Middle fatty capsule / perinephric fat-it is a collection of fatty tissue. (It acts as a shock absorber & helps to maintain the kidney in its position) 3. The false capsule – made of renal fascia .It has two layers-Anterior & Posterior. (Superiorly the two layers enclose the supra renal gland & then merge with diaphragmatic fascia, that is why the kidneys move with respiration)
- 10. Anatomy of Kidney Macroscopic Structure
- 12. • The functional unit of the kidney, the nephron, consists of the renal corpuscle, Proximal Convoluted Tubule(PCT), loop of Henle, and Distal Convoluted Tubule (DCT). • Cortical nephrons have short loops of Henle, whereas juxtamedullary nephrons have long loops of Henle extending into the medulla. • About 15 percent of nephrons are juxtamedullary. The glomerulus is a capillary bed that filters blood principally based on particle size. • The filtrate is captured by Bowman’s capsule and directed to the PCT. • A filtration membrane is formed by the fused basement membranes of the podocytes and the capillary endothelial cells that they embrace.
- 13. • Contractile mesangial cells further perform a role in regulating the rate at which the blood is filtered. • Specialized cells in the JGA(juxtaglomerular cell) produce paracrine signals to regulate blood flow and filtration rates of the glomerulus. Other JGA cells produce the enzyme renin, which plays a central role in blood pressure regulation. • The filtrate enters the Proximal Convoluted Tubule(PCT) where absorption and secretion of several substances occur. The descending and ascending limbs of the loop of Henle consist of thick and thin segments. • Absorption and secretion continue in the Distal Convoluted Tubule (DCT). but to a lesser extent than in the PCT. Each collecting duct collects forming urine from several nephrons and functions to fine tune water recovery.
- 15. Kidney: Frontal Section • Minor calyx: cup over papilla collects urine
- 16. Anatomy of Kidney • Renal cortex: outer 1 cm • Renal medulla: renal columns, pyramids - papilla • Lobe of kidney: pyramid and it’s overlying cortex
- 17. Microscopic Structure(Histology) The kidney may be regarded as a collection of millions of uriniferous tubules. Each uriniferous tubule consists of an excretory part called nephron and of a collecting tubule. Each kidney contains over 1(1-2 millions) million nephrons and thousands of collecting ducts
- 25. Blood Supply Diagram Arterial Supply: Renal arteries which are the direct branches of abdominal aorta & are large in size. Venous Drainage: Renal veins, ends in inferior vena cava. The left renal vein is longer than the right. Nerve Supply: Sympathetic fibers derived from T10,L1 segments and parasympathetic fibers from vagus nerve. Lymphatic drainage: into lateral aortic nodes.
- 26. Kidney Functions • Filters blood plasma, eliminates waste, returns useful chemicals to blood • Regulates osmolarity of body fluids • Endocrine organ – A-Synthesis of acid protease RENIN – - enzyme involved in control of blood pressure and blood volume. Angiotensinogen Angiotensin I Renin
- 27. B-Erythropoietin synthesis – -glycoprotein hormone which regulates RBCs formation in response to decrease O2 concentration. - erythropoietin acts on specific receptors expressed on surface of CFU for erythrocytes in bone marrow. • Secretes erythropoietin, controls RBC count • Regulates PCO2 acid base balance • Detoxifies free radicals and drugs • Gluconeogenesis
- 29. Kidney Conditions • Pyelonephritis (infection of kidney pelvis): Bacteria may infect the kidney, usually causing back pain and fever. A spread of bacteria from an untreated bladder infection is the most common cause of pyelonephritis. • Glomerulonephritis: An overactive immune system may attack the kidney, causing inflammation and some damage. Blood and protein in the urine are common problems that occur with glomerulonephritis. It can also result in kidney failure. • Kidney stones (nephrolithiasis): Minerals in urine form crystals (stones), which may grow large enough to block urine flow. It's considered one of the most painful conditions. Most kidney stones pass on their own, but some are too large and need to be treated.
- 30. • Nephrotic syndrome: Damage to the kidneys causes them to spill large amounts of protein into the urine. Leg swelling (edema) may be a symptom. • Polycystic kidney disease: A genetic condition resulting in large cysts in both kidneys that hinder their work. • Acute renal failure (kidney failure): A sudden worsening in how well your kidneys work. Dehydration, a blockage in the urinary tract, or kidney damage can cause acute renal failure, which may be reversible. • Chronic renal failure: A permanent partial loss of how well your kidneys work. Diabetes and high blood pressure are the most common causes.
- 31. • Diabetic nephropathy: High blood sugar from diabetes progressively damages the kidneys, eventually causing chronic kidney disease. Protein in the urine (nephrotic syndrome) may also result. • Hypertensive nephropathy: Kidney damage caused by high blood pressure. Chronic renal failure may eventually result. • Kidney cancer: Renal cell carcinoma is the most common cancer affecting the kidney. Smoking is the most common cause of kidney cancer. • Interstitial nephritis: Inflammation of the connective tissue inside the kidney, often causing acute renal failure. Allergic reactions and drug side effects are the usual causes.
- 32. Kidney Tests • Urinalysis: A routine test of the urine by a machine and often by a person looking through a microscope. Urinalysis can help detect infections, inflammation, microscopic bleeding, and kidney damage. • Kidney ultrasound: A probe placed on the skin reflects sound waves off the kidneys, creating images on a screen. Ultrasound can reveal blockages in urine flow, stones, cysts, or suspicious masses in the kidneys. • Computed tomography (CT) scan: A CT scanner takes a series of X-rays, and a computer creates detailed images of the kidneys. • Magnetic resonance imaging (MRI) scan: A scanner uses radio waves in a magnetic field to make high-resolution images of the kidneys.
- 33. • Urine and blood cultures: If an infection is suspected, cultures of the blood and urine may identify the bacteria responsible. This can help target antibiotic therapy. • Ureteroscopy: An endoscope (flexible tube with a camera on its end) is passed through the urethra into the bladder and ureters. Ureteroscopy generally cannot reach the kidneys themselves, but can help treat conditions that also affect the ureters. • Kidney biopsy: Using a needle inserted into the back, a small piece of kidney tissue is removed. Examining the kidney tissue under a microscope may help diagnose a kidney problem.
- 34. Kidney Treatment • Antibiotics: Kidney infections caused by bacteria are treated with antibiotics. Often, cultures of the blood or urine can help guide the choice of antibiotic therapy. • Nephrostomy: A tube (catheter) is placed through the skin into the kidney. Urine then drains directly from the kidney, bypassing any blockages in urine flow. • Lithotripsy: Some kidney stones may be shattered into small pieces that can pass in the urine. Most often, lithotripsy is done by a machine that projects ultrasound shock waves through the body. • Nephrectomy: Surgery to remove a kidney. Nephrectomy is performed for kidney cancer or severe kidney damage.
- 35. Kidney Treatment • Dialysis: Artificial filtering of the blood to replace the work that damaged kidneys can't do. Hemodialysis is the most common method of dialysis in the U.S. • Hemodialysis: A person with complete kidney failure is connected to a dialysis machine, which filters the blood and returns it to the body. Hemodialysis is typically done 3 days per week in people with ESRD. • Peritoneal dialysis: Placing large amounts of a special fluid in the abdomen through a catheter allows the body to filter the blood using the natural membrane lining the abdomen. After a while, the fluid with the waste is drained and discarded. • Kidney transplant: Transplanting a kidney into a person with ESRD can restore kidney function. A kidney may be transplanted from a living donor, or from a recently deceased organ donor.
