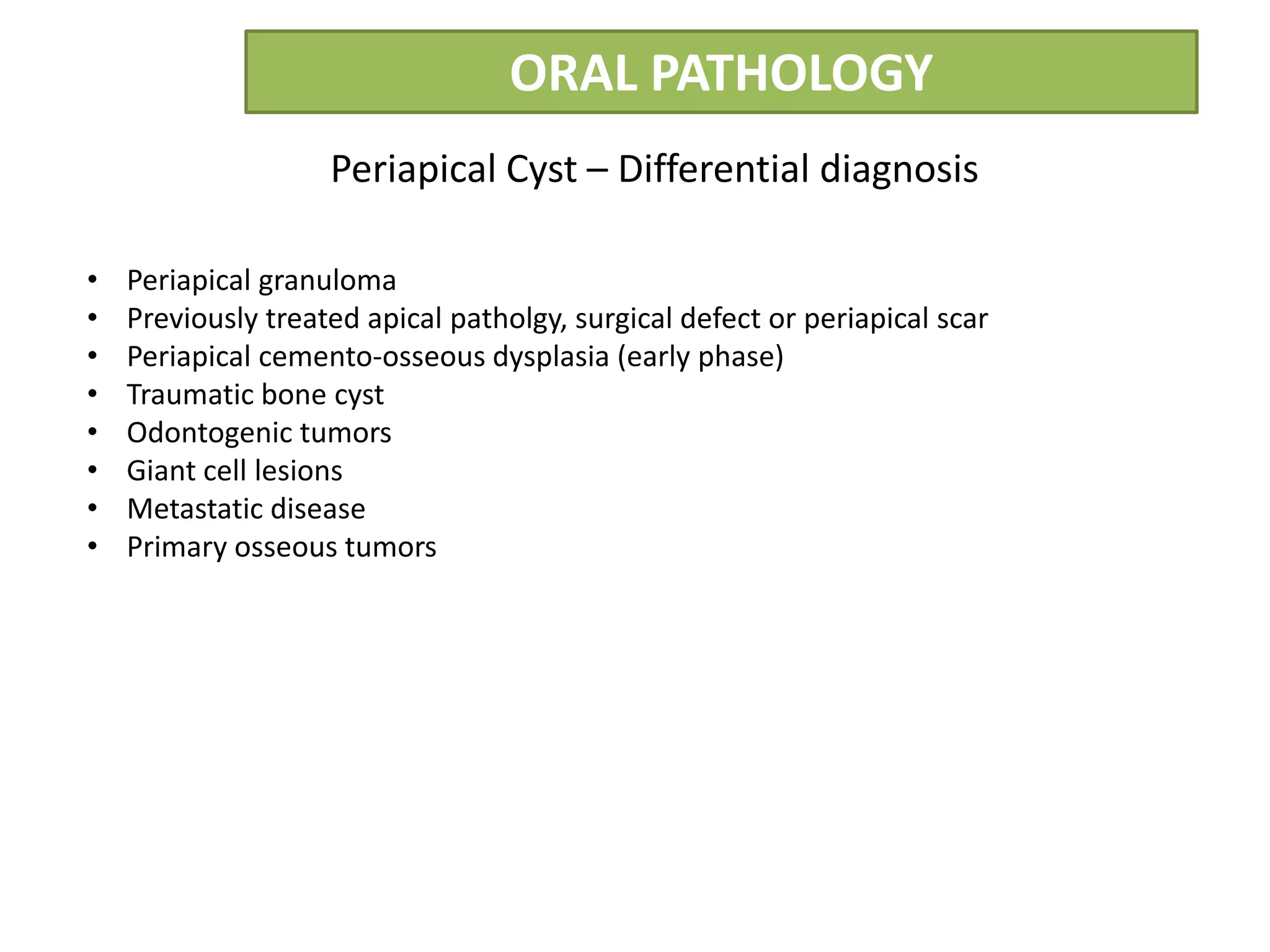
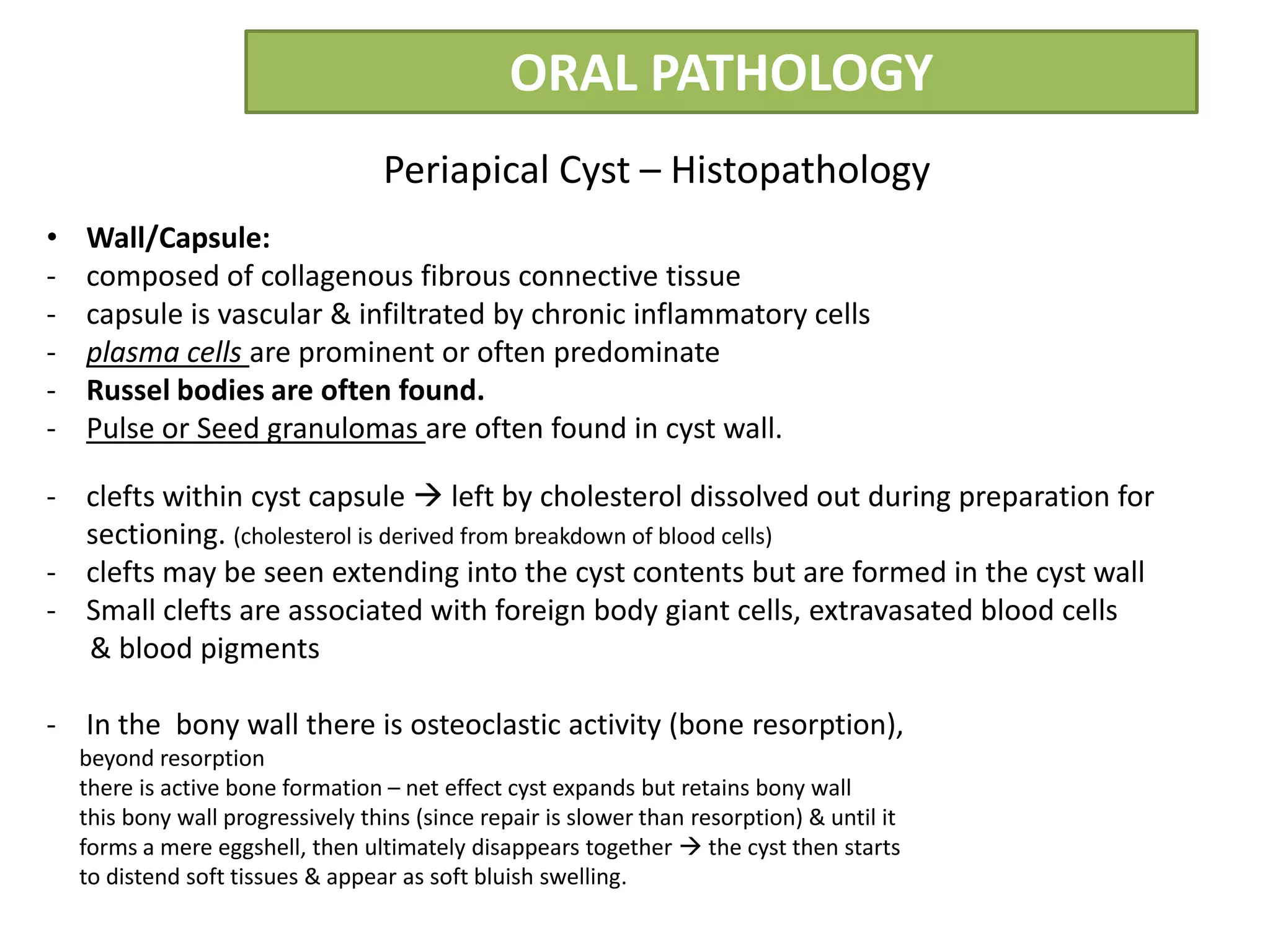
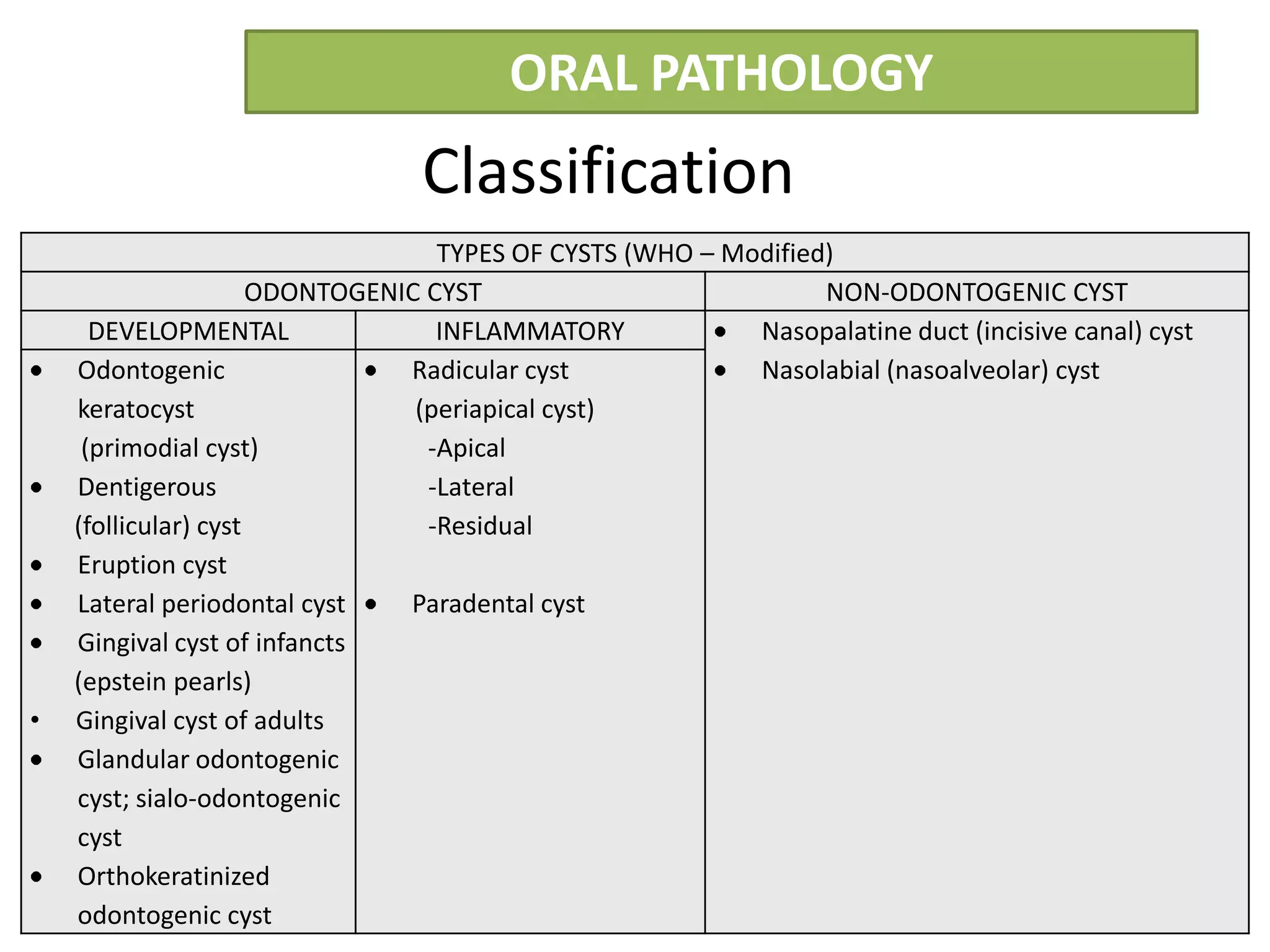
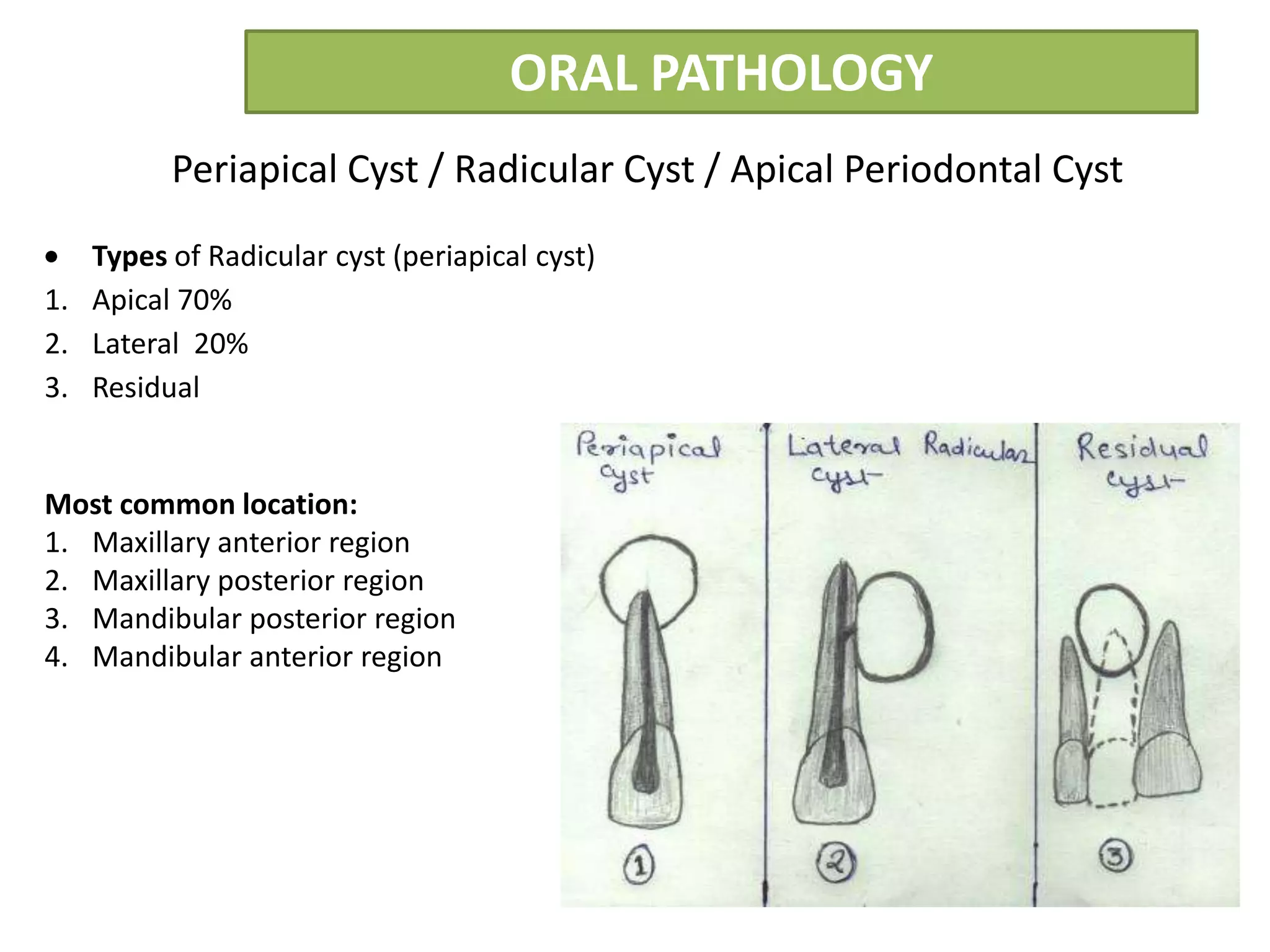
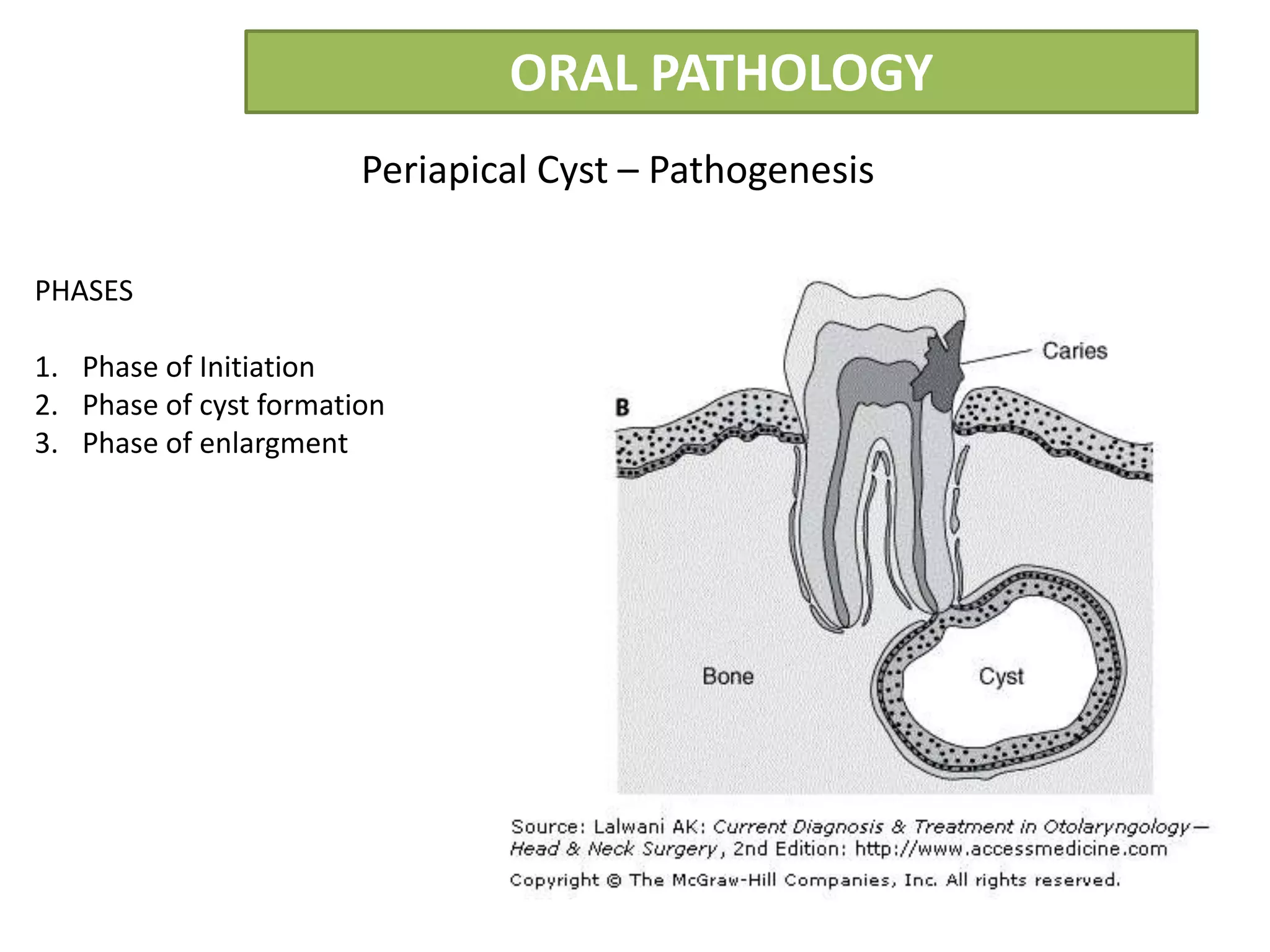
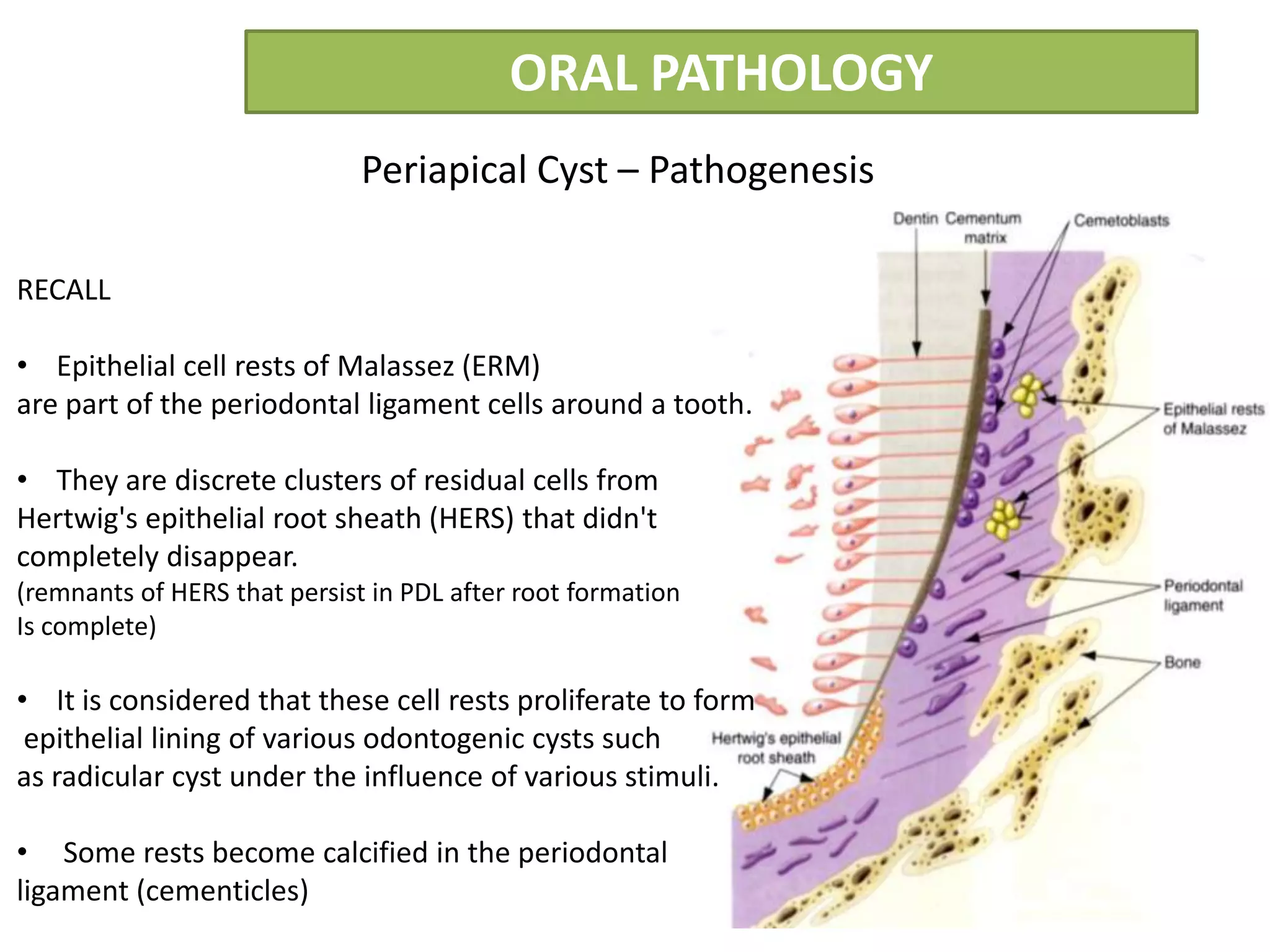
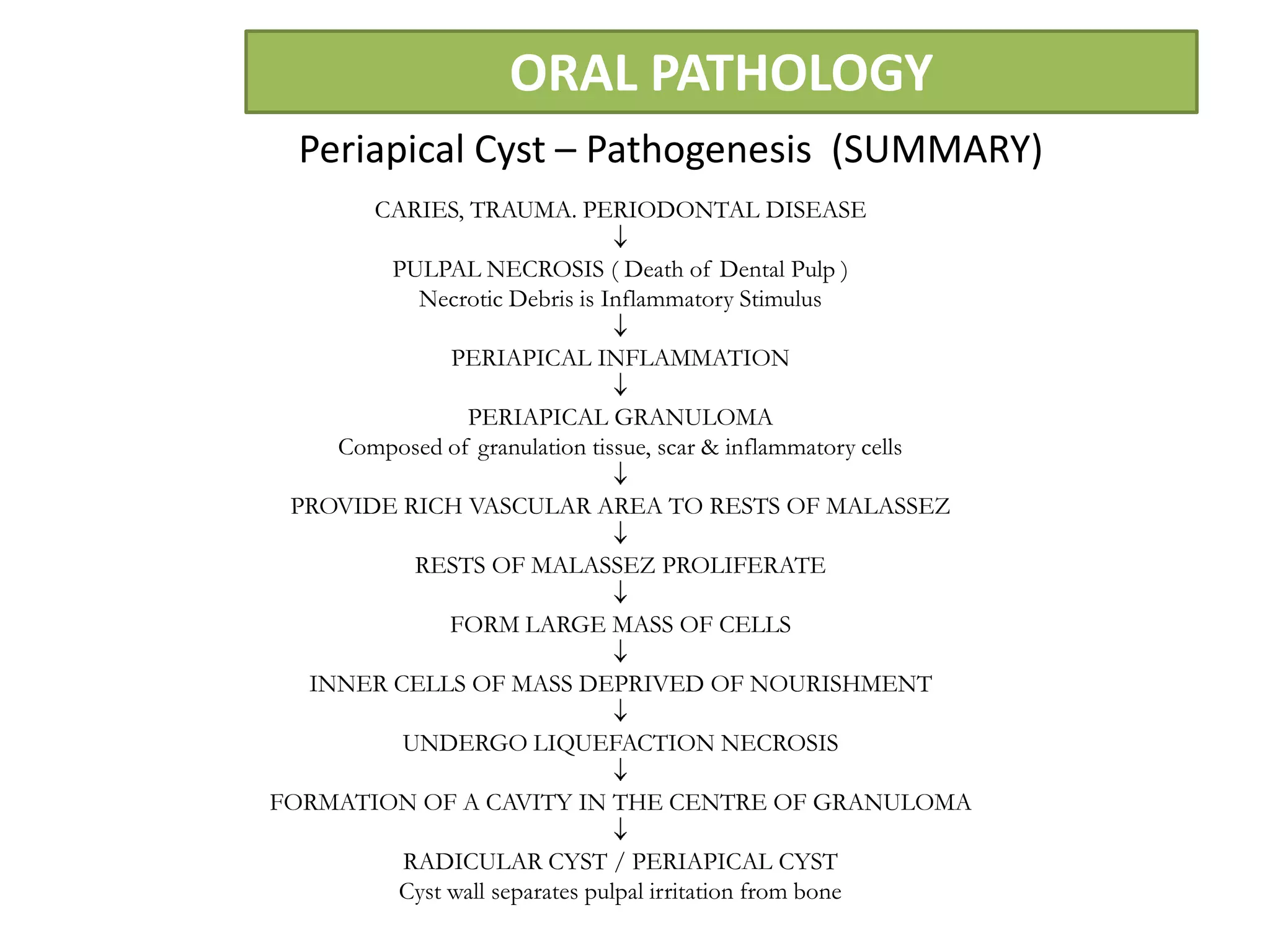
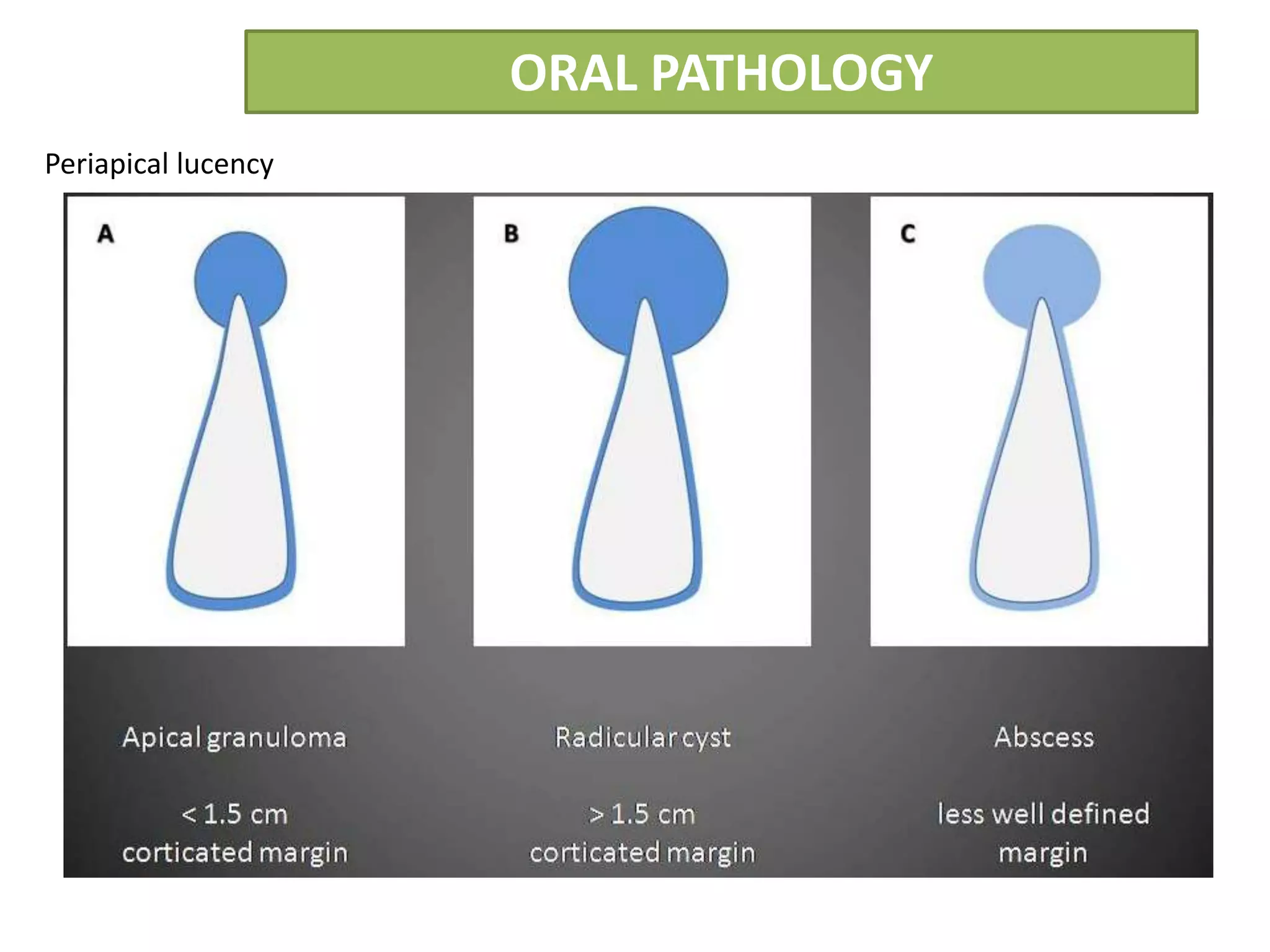
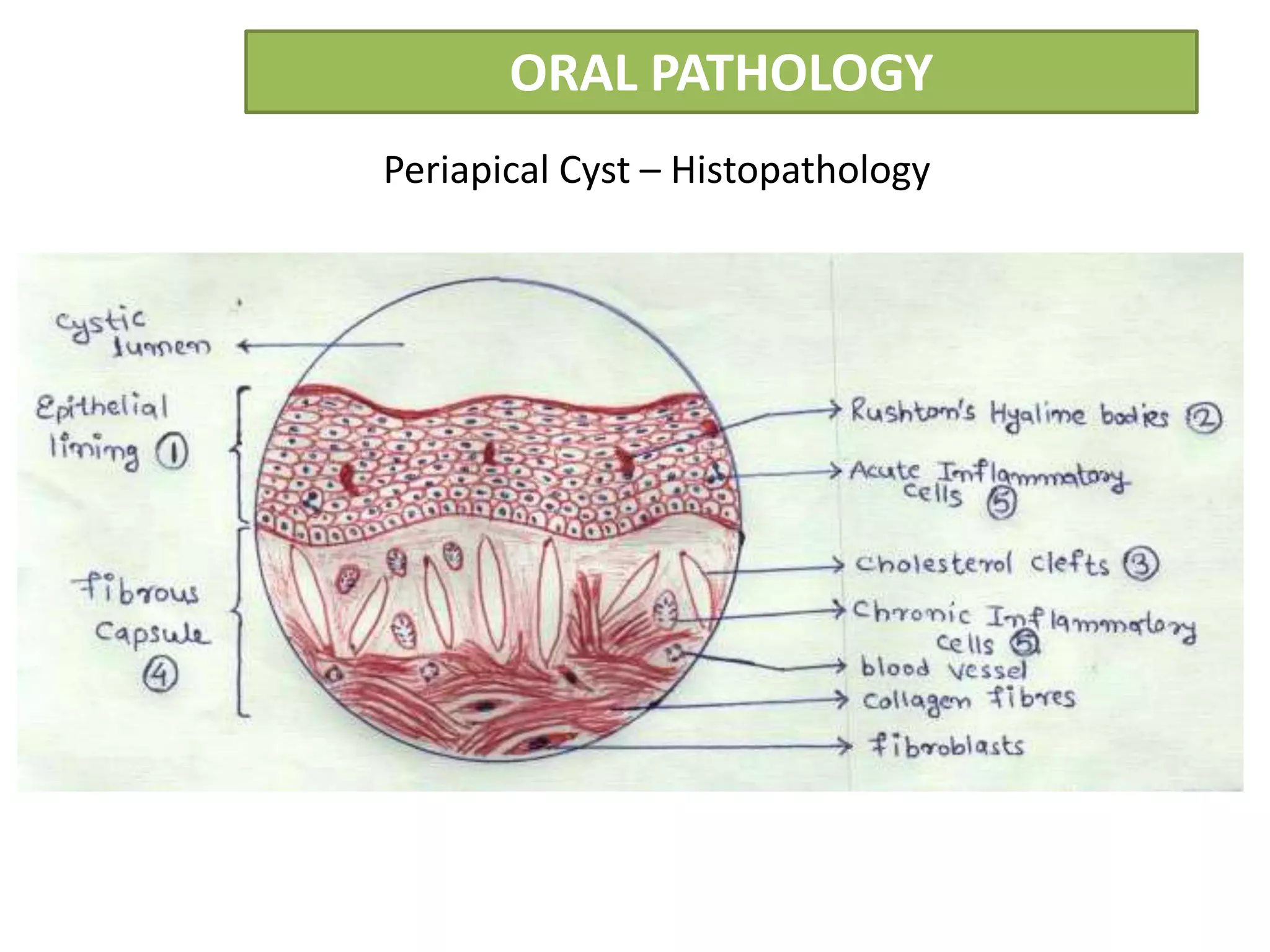
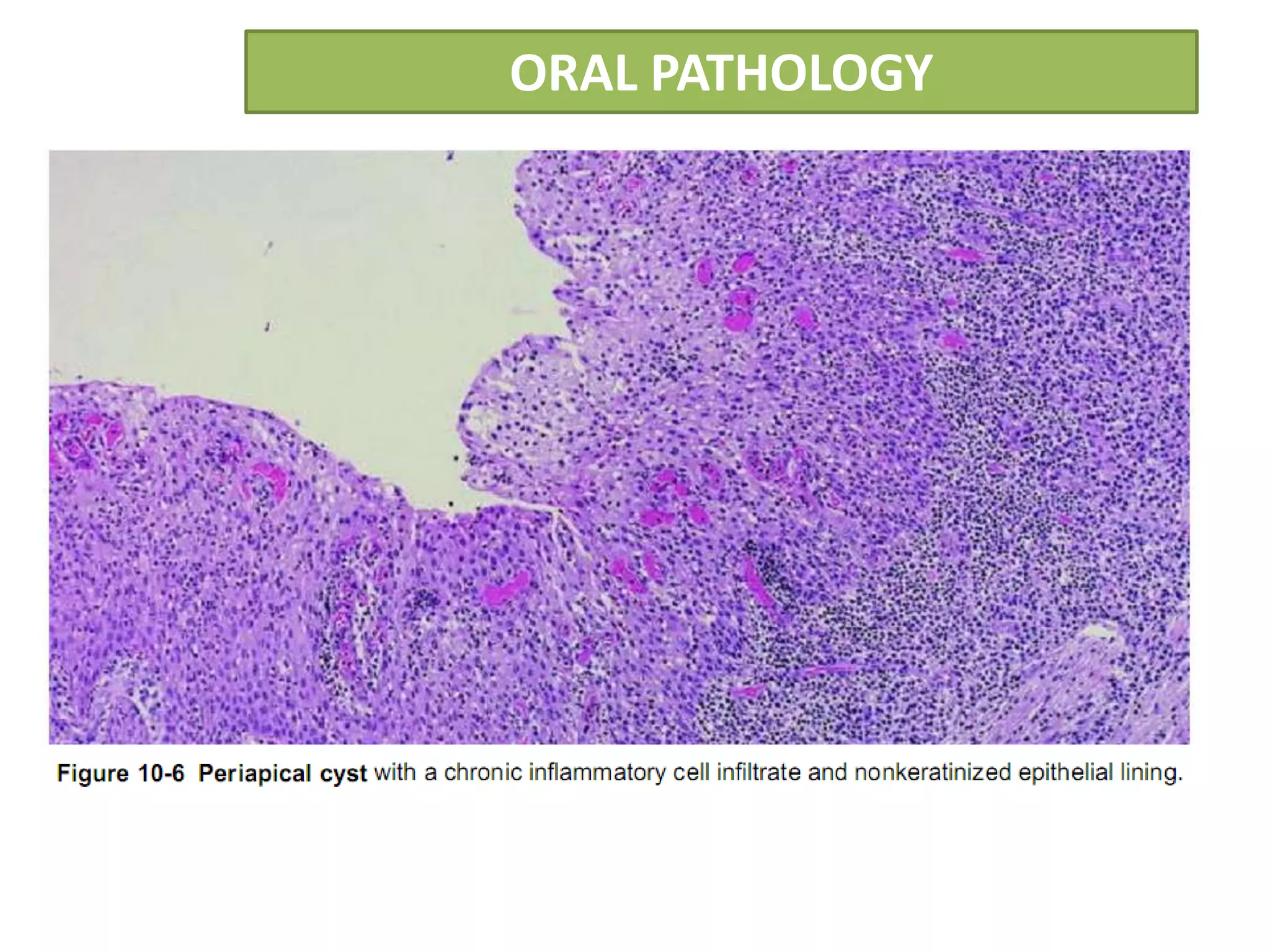
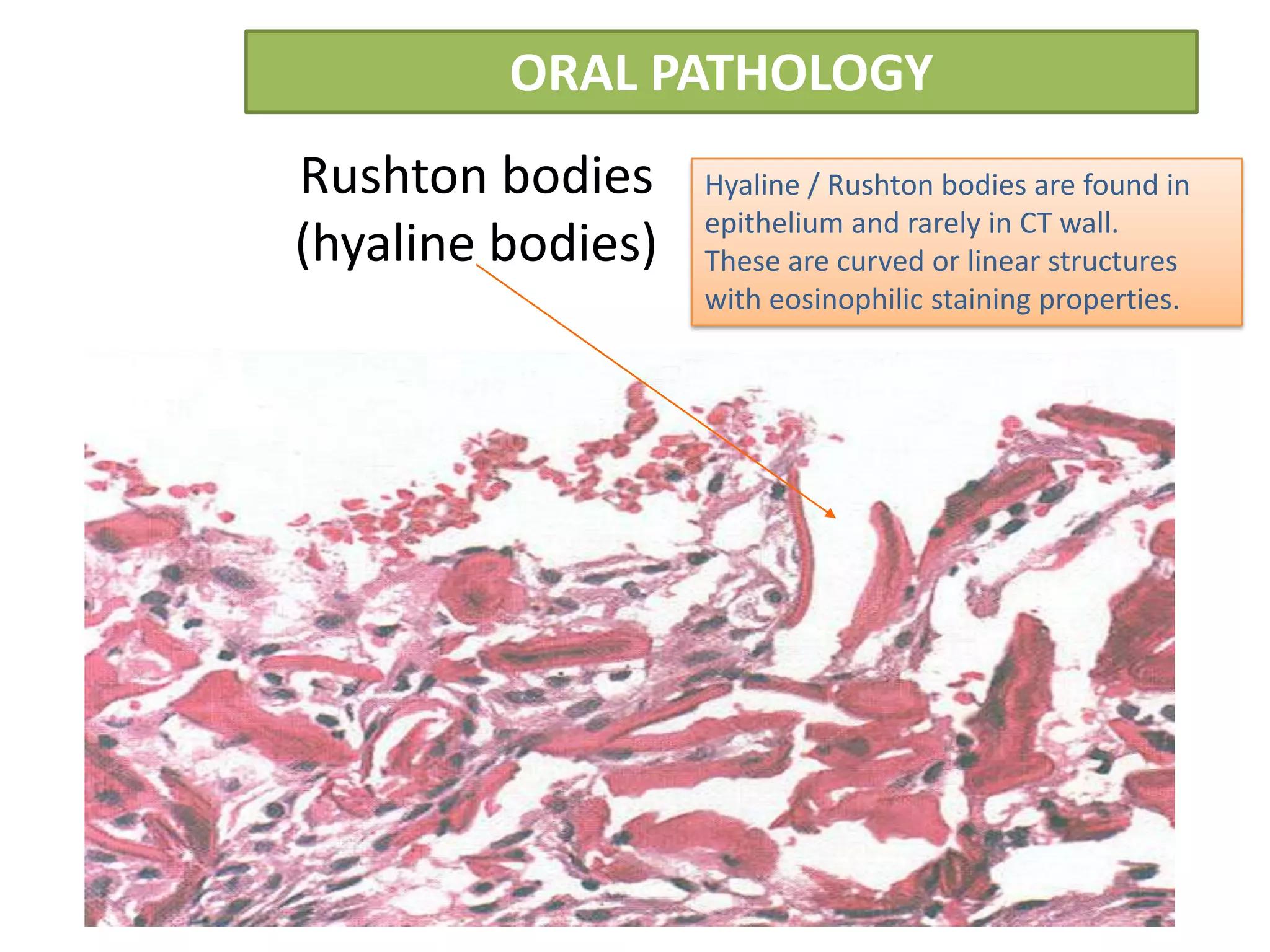
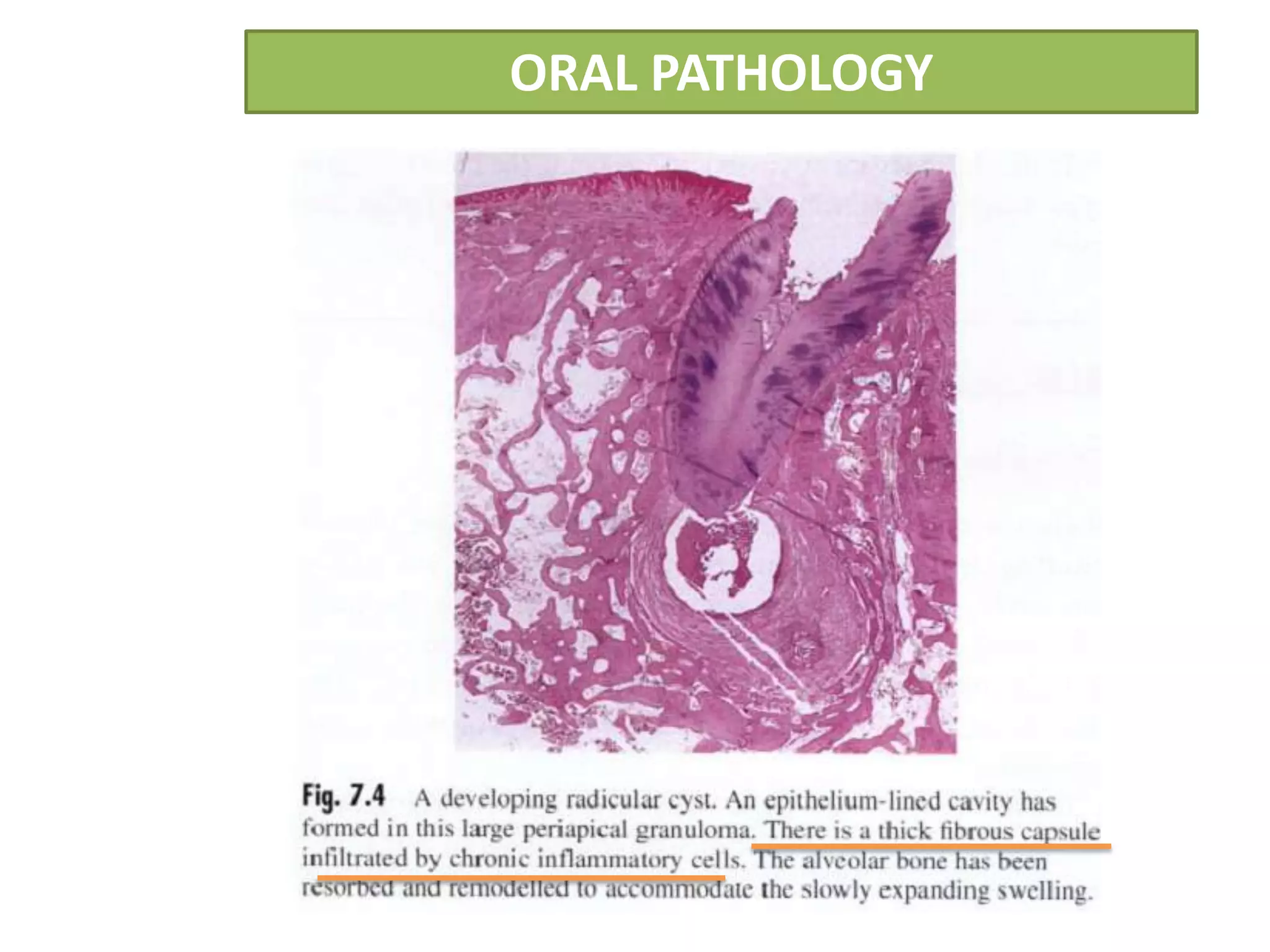
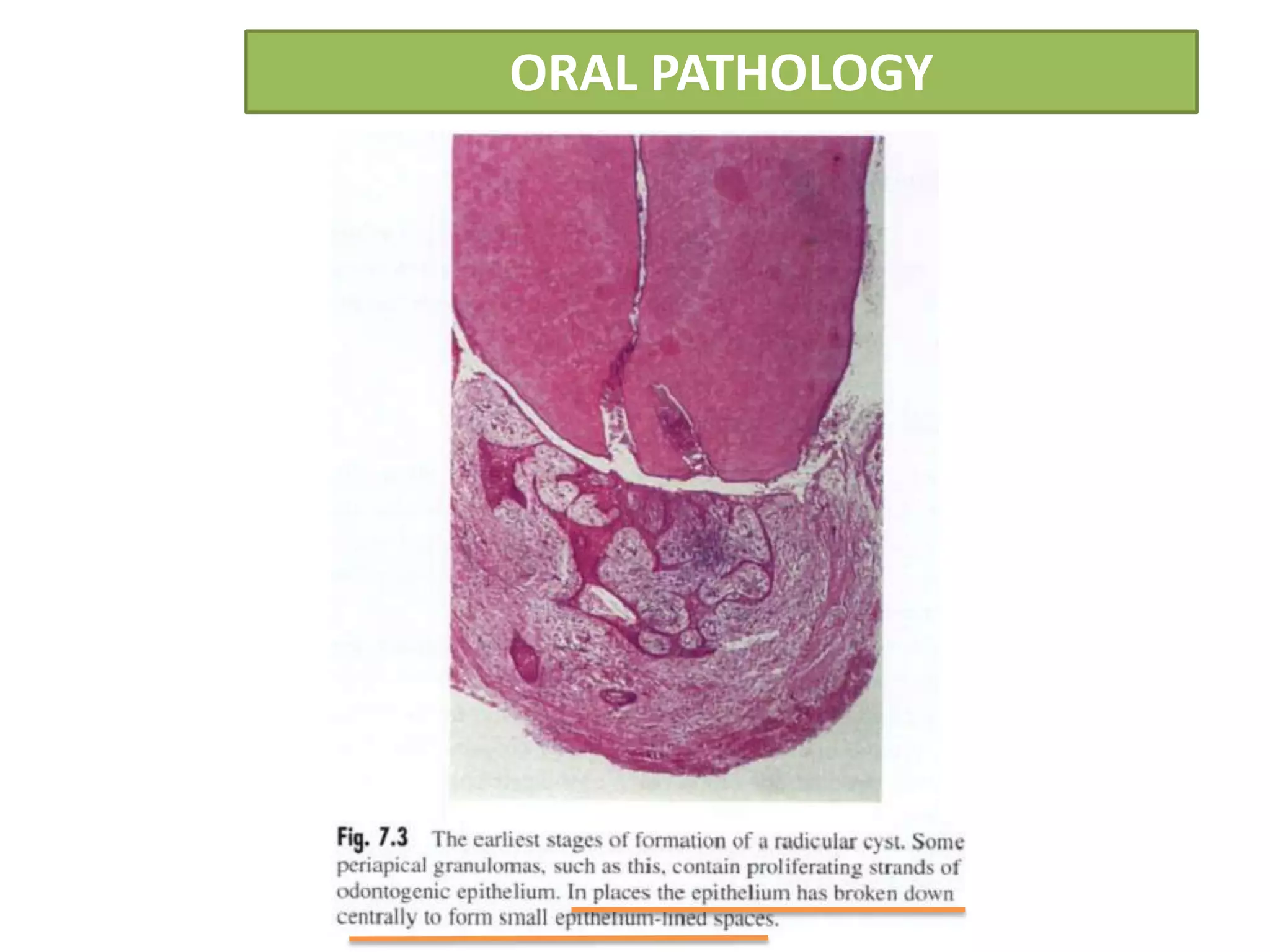
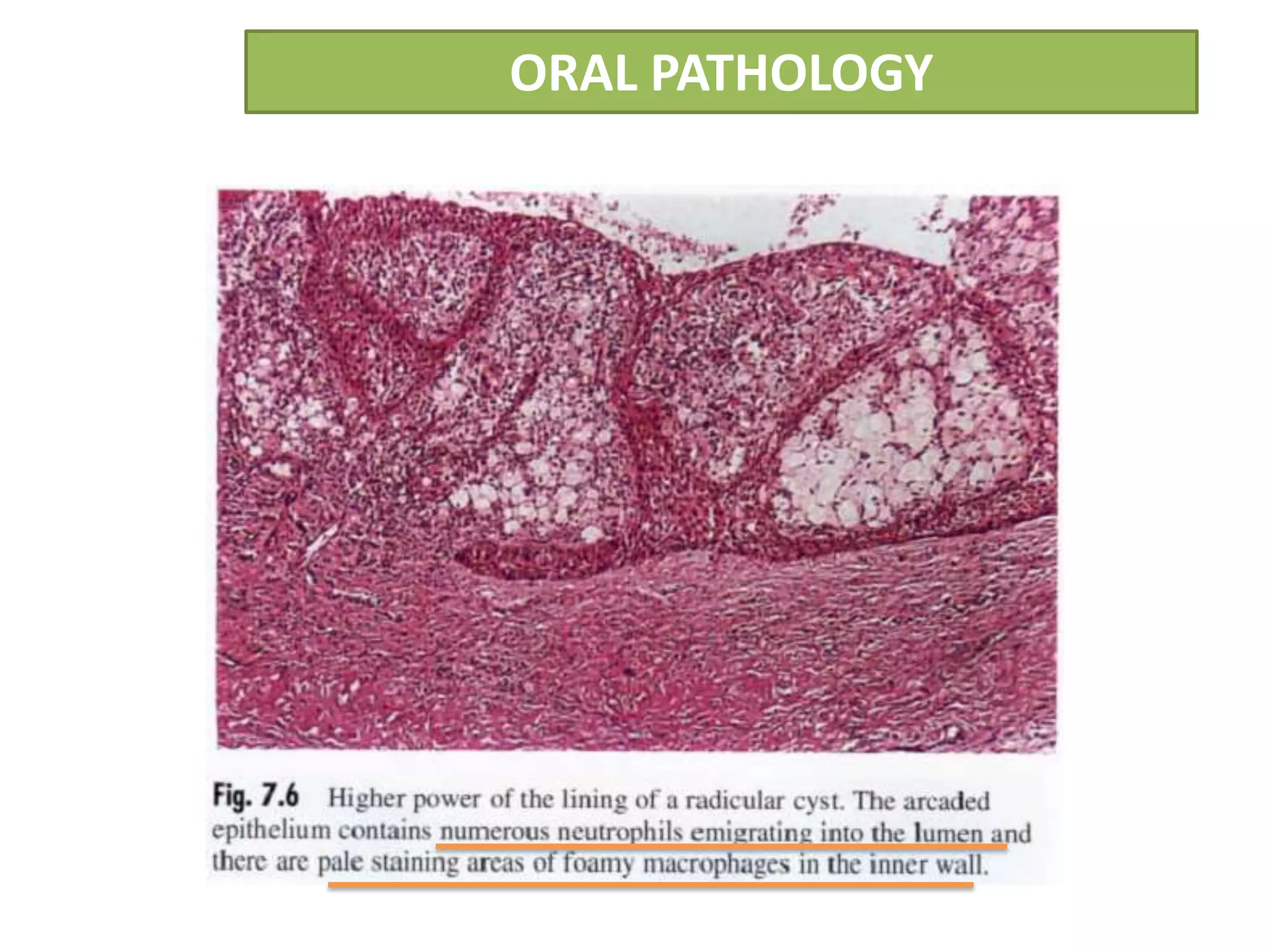
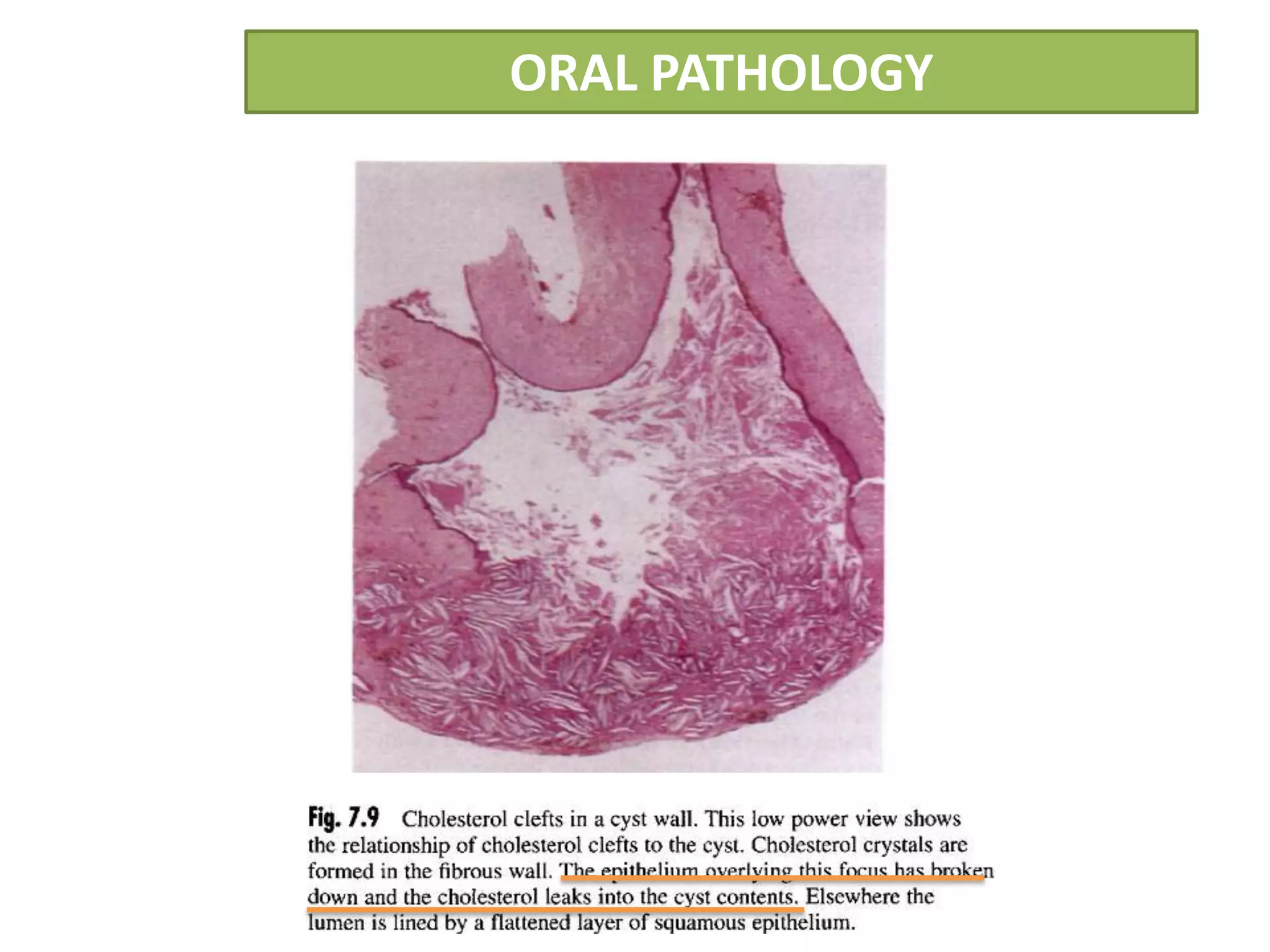
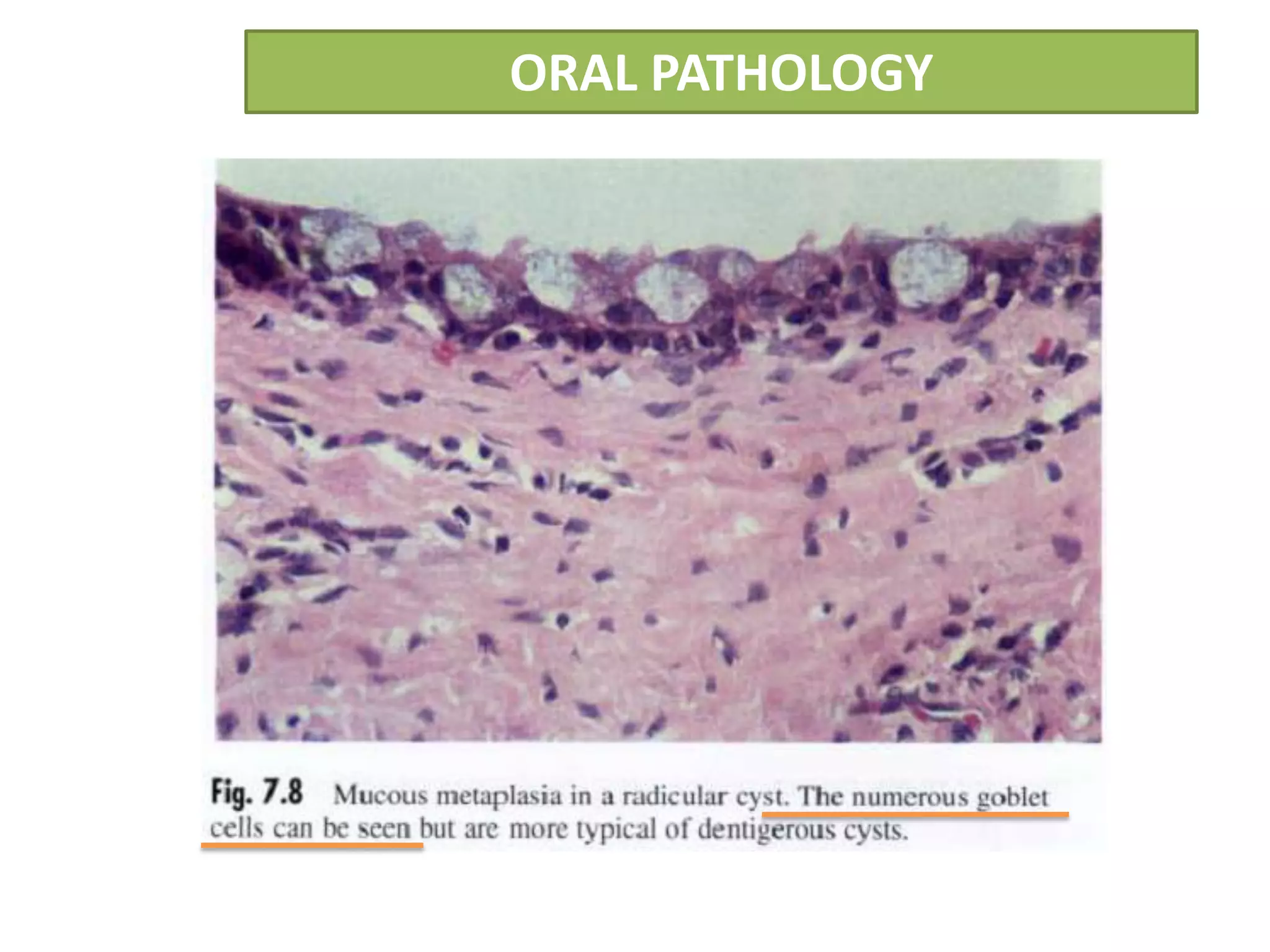
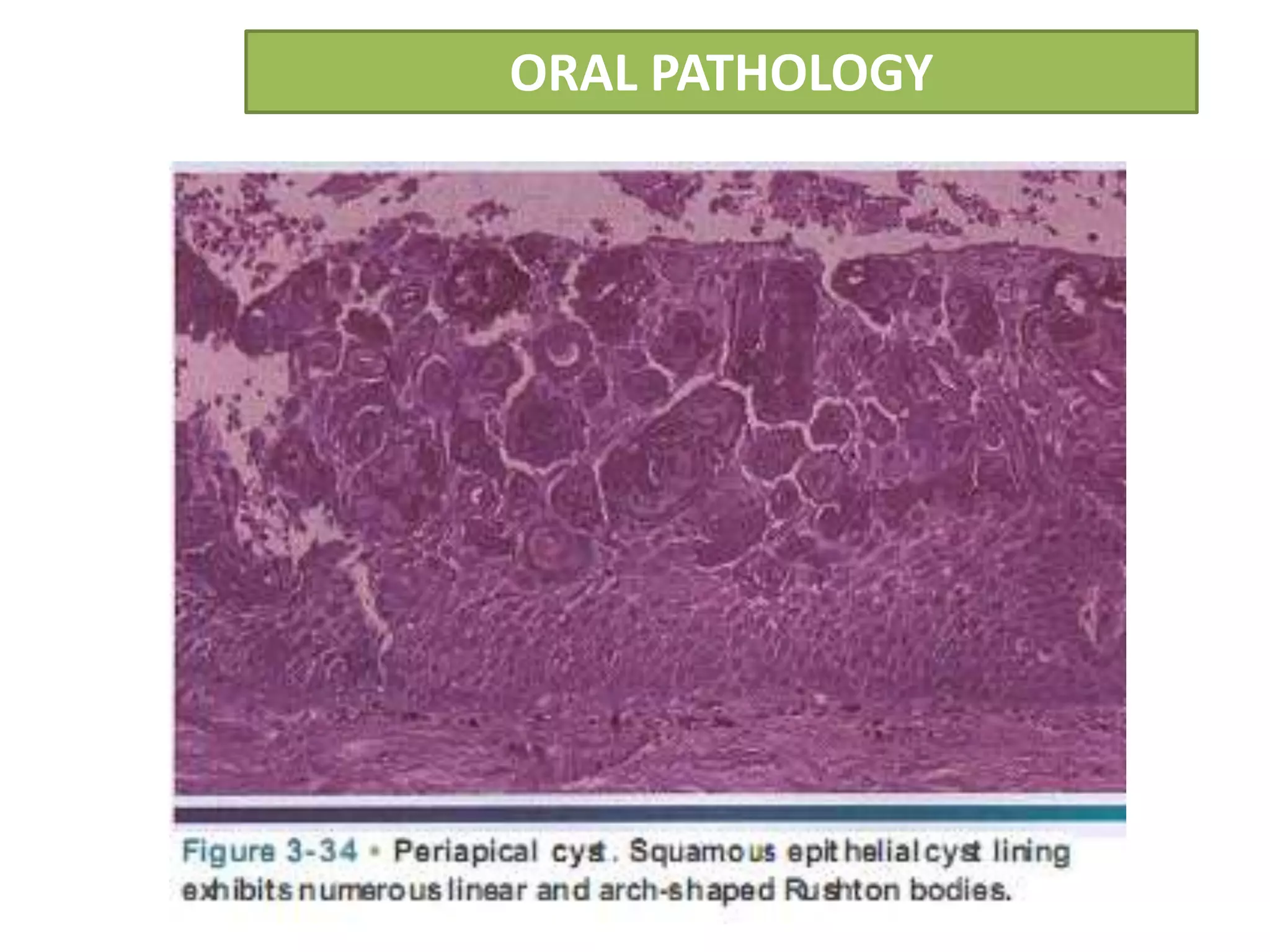
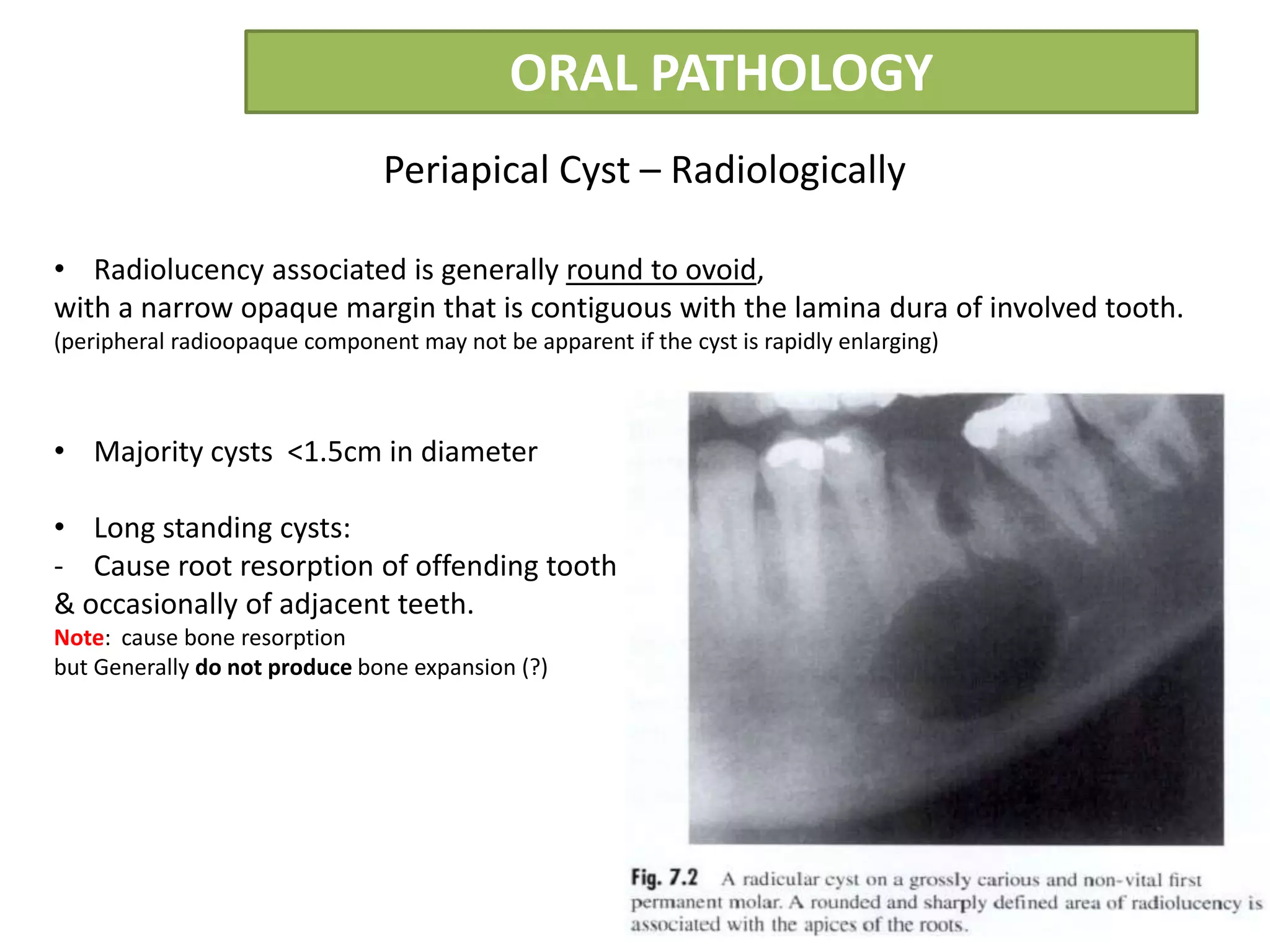
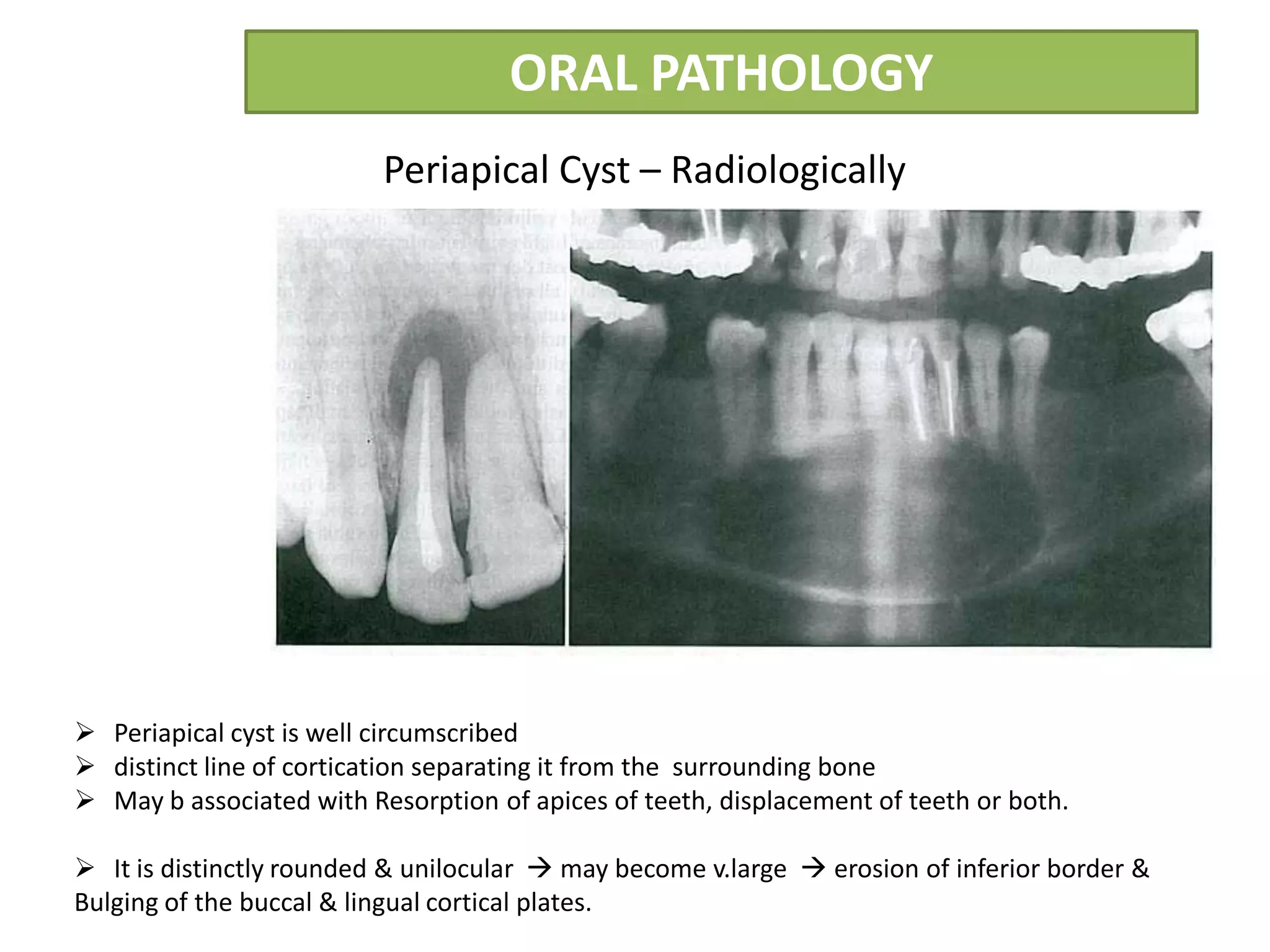
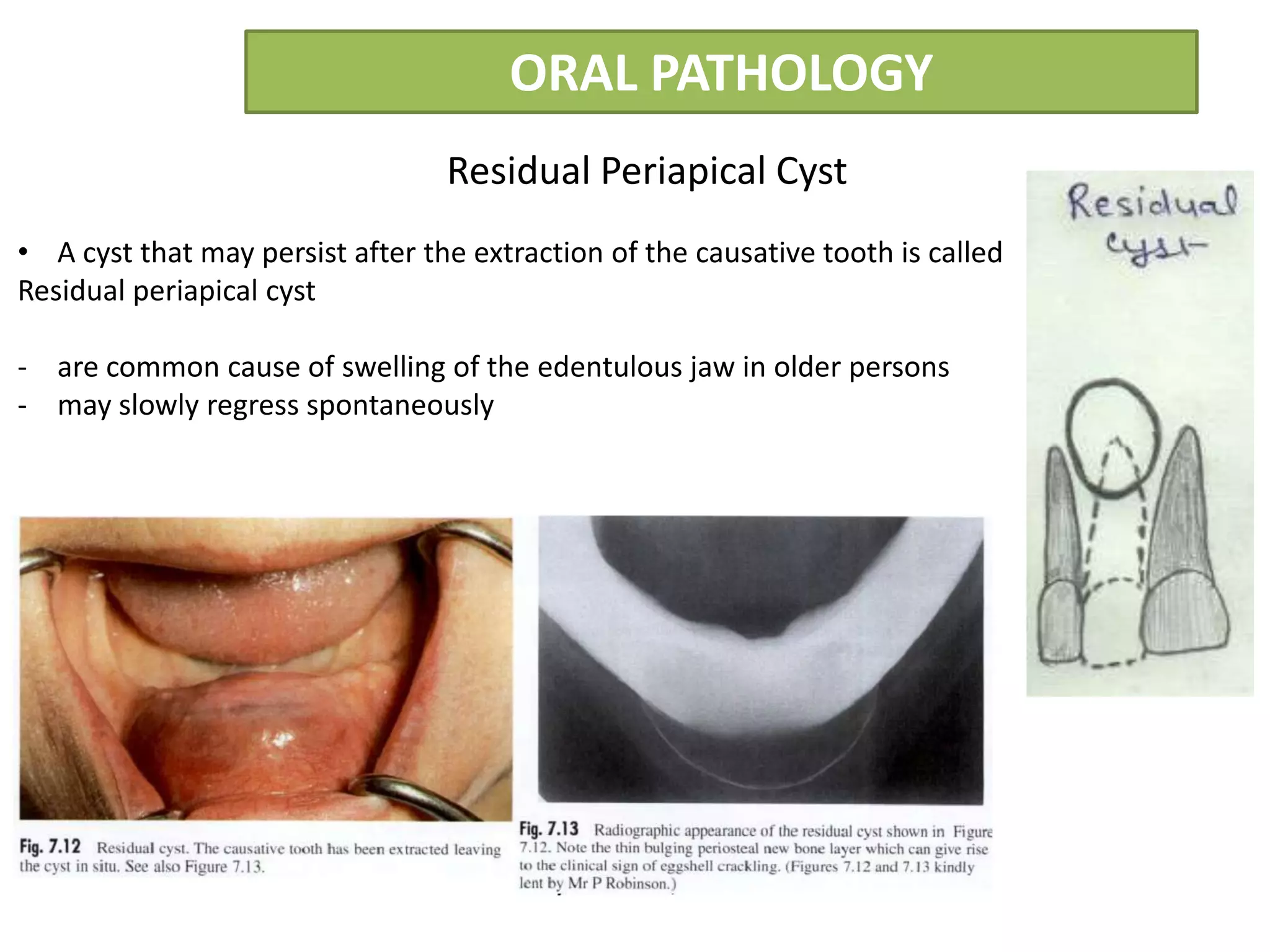
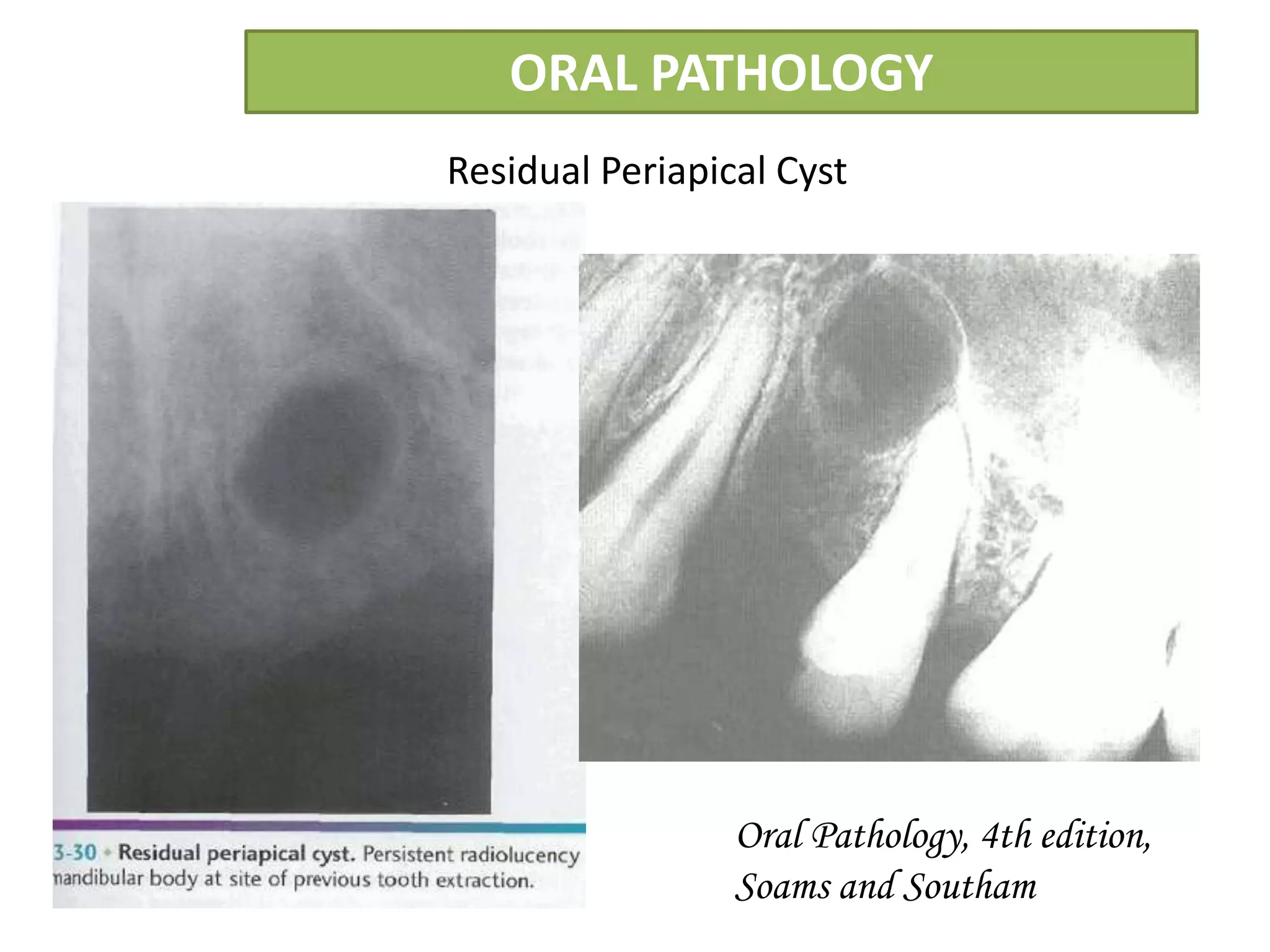
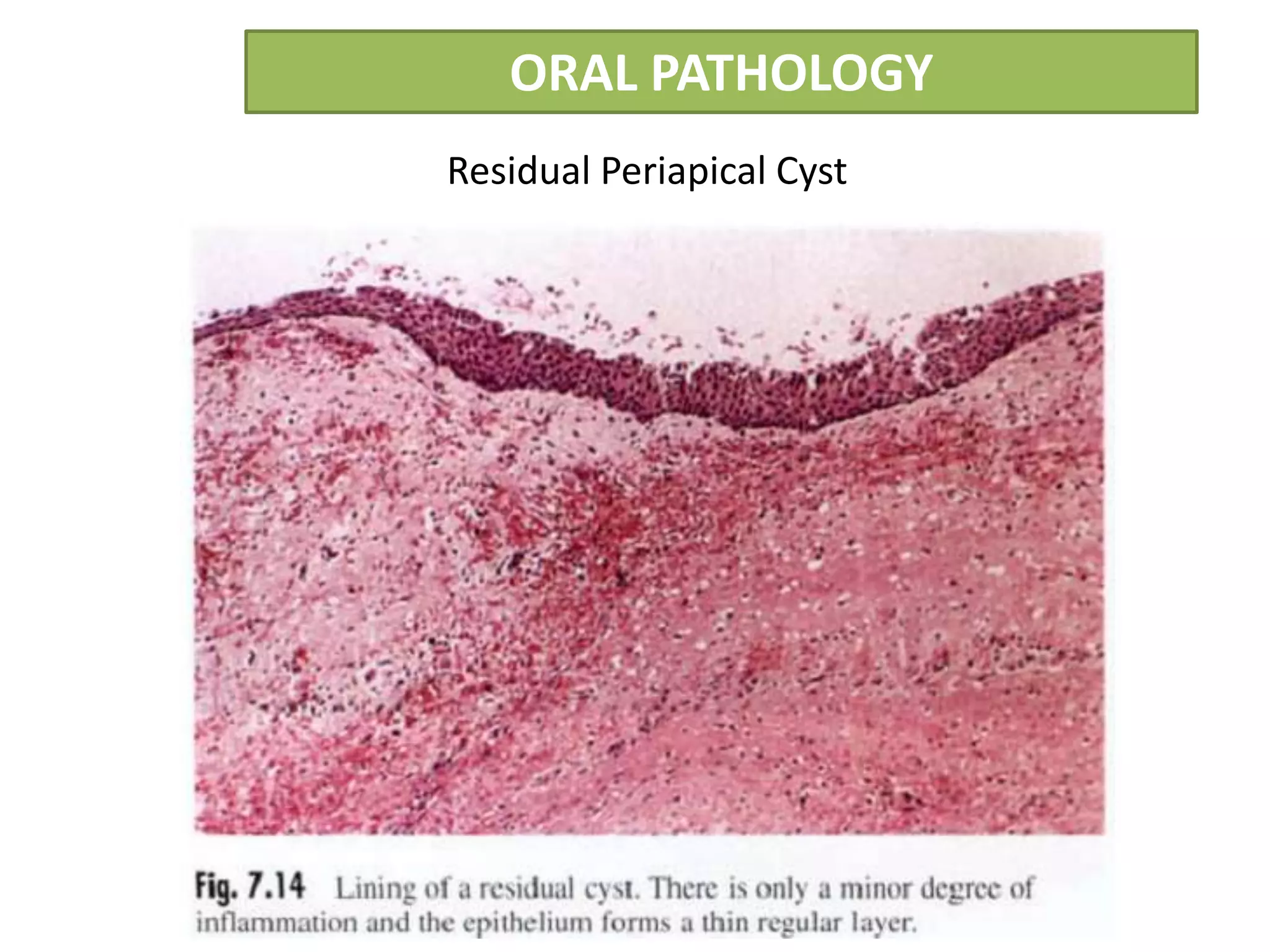
The document summarizes information about periapical cysts, also known as radicular cysts or apical cysts. It defines a periapical cyst as an odontogenic cyst derived from cell rests of Malassez that proliferate in response to inflammation from pulpal necrosis. Periapical cysts typically present as round radiolucencies associated with the apex of a non-vital tooth. Histologically, they contain a lumen lined by stratified squamous epithelium and surrounded by a fibrous connective tissue wall. Treatment involves extraction of the involved tooth along with cyst enucleation or marsupialization.