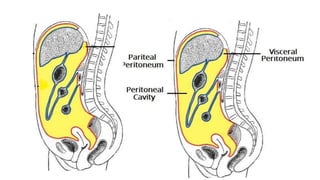
The Cavities of the Body: An Overview of the Peritoneum
- 4. Peritoneum • Large serous sac • Lines inner surface of abdomino- pelvic wall
- 5. Why different layers? • Invaginated by viscera from different sides • Invagination throws the peritoneum into folds & • Forms • Parietal & visceral layers • & potential spaces
- 6. Peritoneum - parts • Parietal Peritoneum • Lines the inner surface of • Abdominal and pelvic walls and • Lower surface • Diaphragm • Embryologically from somatopleuric mesoderm • Derives blood & nerve supply from body wall • Visceral Peritoneum • Lines outer surface of viscera • Firmly attaches with viscera • Develops from splanchnopeuric mesoderm • Blood supply and nerve supply are the same as those of underlying viscera
- 7. Interperitoneal organs • Most part of viscera surrounded by peritoneum • Stomach, Liver, gallbladder • Tail of pancreas, spleen • First part of duodenum, jejunum, ileum • Transverse colon, sigmoid colon • Upper part of rectum, urinary bladder and uterus
- 8. Retroperitoneal organs • Organs lie on the posterior abdominal wall are covered by peritoneum on their anterior surfaces • Descending and horizontal parts of duodenum, pancreas (head, neck & body) • Ascending & descending colon • Kidney, suprarenal gland, ureters • Abdominal aorta & IVC • Middle and lower parts of rectum
- 9. Secondary retroperitoneal organs • Duodenum • 2nd and 3rd part • Pancreas (except tail) • Ascending colon • Descending colon • Upper rectum
- 10. Folds of Peritoneum - types • Many organs within abdomen are suspended by folds of peritoneum • Provide pathways for passage of vessels, nerves and lymphatics • Named after their attached organs • Omentum • Fold of peritoneum connecting stomach to other organs • Mesenteries • Fold invests small intestine • Mesocolon • Fold invests large intestine • Peritoneal ligaments • Folds attached with other organs
- 11. Disposition – Vertical • Start from • Anterior abdominal wall • At umbilical level • Lines • Inner aspect of anterior abdominal wall • Trace • Upto ant part of diaphragm (under surface) • Right of median plane • Falciform ligament • In free margin it contains • Ligamentum teres hepatis • Obliterated left umbilical vein (extends from umbilicus to inferior surface of liver) • Also it contains para umbilical veins • Tributaries to left branch of Portal vein
- 12. Disposition – Vertical • Inferior surface of diaphragm to upper surface of liver • Falciform ligament • 2 layers diverge to right & left • On right (right layer of falciform) • From diaphragm to right lobe of liver forms • Superior layer of coronary ligament • On left (left layer of falciform lig) • From diaphragm to left lobe of liver forms • Left triangular ligament (anterior layer)
- 13. Disposition – Vertical • After covering the superior and anterior surfaces of liver • Reaches inferior surface of liver • Right of Gall bladder • Peritoneum passes down to • Suprarenal & kidney as inferior layer of coronary ligament • Bare area • Between the 2 layers of coronary ligament • Right triangular ligament • 2 layers of coronary ligament unite to form • Connects right lobe of liver with diaphragm
- 14. Disposition – Vertical Ligamentum venosum - remnant of ductus venosus (oblitrated ductus venosus), which shunted blood from the umbilical vein to the IVC in fetal life • On the left of gall bladder • After covering quadrate lobe & left lobe • Becomes posterior layer of left triangular ligament • Then passes to • Left margin of fissure for ligamentum venosum & anterior lip of porta hepatis & • From anterior lip of porta hepatis to right and then posterior lip of porta hepatis • Covering caudate lobe & attached to right lip of fissure for ligamentum venosum • These two layers form • Lesser omentum • Has inverted L shaped attachment
- 15. Omentum • Peritoneal folds related to stomach • Lesser omentum • Greater omentum
- 16. Lesser omentum • Connects liver to stomach • Attachment • Above to porta hepatis & fissure for ligamentum venosum • Inferiorly to lesser curvature of the stomach & 1st inch of duodenum • Parts • Hepato gastric ligament • Hepato duodenal ligament • Forms free margin • Contains • Portal vein (posteriorly) • Hepatic artery (anterior & left) • Bile duct (anterior & right)
- 17. Lesser omentum • Contents • Hepatic artery, bile duct, portal vein • In free margin - • Rt. & lt. gastric vessels • Along lesser curvature
- 18. Tracing lesser omentum • Peritoneum from • Anterior lip of porta hepatis and left lip of fissure for ligamentum venosum • Posterior lip of porta hepatis and right lip of fissure for ligamentum venosum • Continues downwards as lesser omentum towards lesser curvature of stomach and first one inch of duodenum • Forms anterior boundary for upper part of lesser sac
- 19. Tracing lesser omentum • After reaching lesser curvature • Two layers separates • And covers the surfaces • Reaches greater curvature • Becomes anterior two layers of greater omentum
- 20. Tracing greater omentum • From greater curvature • Anterior & posterior layers comes downwards • After awhile it returns back towards anterior border of pancreas • So 4 layers are there • Together they form Greater omentum • Space between 2nd & 3rd layer is lesser sac • Patent in fetal life • But obliterated - after birth
- 21. Fate of 3rd & 4th layers • Continuation of layers of lesser omentum • Forms 1st & 2nd layer of greater omentum • While returns back to pancreas • 1st layer becomes 4th layer • 2nd layer becomes 3rd layer • Third layer • Runs upwards towards anterior border of pancreas (infront of transverse colon) • Passes infront of • Anterior surface of pancreas, kidney and suprarenal gland • Reaches the liver • Forms posterior wall of lesser sac
- 22. Fate of 3rd & 4th layers • 4th layer • Runs towards anterior surface of head & anterior border of body of Pancreas • Then comes down to transverse colon as upper layer of Transverse mesocolon • Encloses transverse colon • Then goes towards inferior surface of pancreas – as inferior layer of Transverse mesocolon Fourth layer of Greater omentum and Superior layer of Transverse mesocolon are adherent – but separable.
- 23. Greater omentum • Largest fold of peritoneum • Hangs down like an apron • In front of coils of small intestine • Made of 4 layers • Anterior 2 layers from Greater curvature and 1st part of duodenum • Extending downwards for a considerable distance & • Fold upon themselves to be 3rd & 4th layer • To anterosuperior surface of Tranasverse colon (head & ant border of pancreas)
- 24. Greater omentum – parts & contents • Parts • Gastrophrenic ligament • Gastrosplenic ligament • Gastrocolic ligament • Contents • Rt. &Lt. gastroepiploic vessels • Lymph nodes • Fat • Functions • Store house of fat • Limits the spread of infection
- 25. Transverse mesocolon • Suspends transverse colon • Attached to anterior aspect of head & anterior border of body of pancreas • Contains –Middle colic art.
- 26. Root of mesentery • Peritoneum from transverse mesocolon • Covers lower part of anterior surface of head of pancreas • Passes to front of 3rd & 4th parts of duodenum • Then covers posterior abdominal wall • Becomes folded between • Duodenojejunal flexure(left of L2) to ileocecal junction (rt sacroiliac joint) • Forms root of mesentery
- 27. Mesentery • Fan-shaped fold of peritoneum • Suspends the coils of jejunum and ileum from posterior abdominal wall • Has 2 borders • Attached • Free
- 28. Mesentery - borders • Attached border • Known as root of mesentery • Lies obliquely • Extent • From • Duodenojejunal flexure (L2 – left side) • To • Ileocecal junction (Rt. Sacroiliac joint) • Length - 6 inches (15 cm) • Structures crossed by it • 3rd part of duodenum, Abdominal aorta, IVC • Rt. Psoas major, • Rt. Gonadal vessels, Rt. Genitofemoral nerve & Rt. ureter (medial to lateral) • Rt. Sacroiliac jt
- 29. Mesentery - borders • Free border • Encloses jejunum and ileum • 6 meters in length • Contents • Jejunum, ileum • Lymph nodes • Jejunal & ileal branches of superior mesenteric artery & nerve plexus • Fat
- 30. Meso-appendix • Δ-gular fold • Suspends appendix • From post surface of lower end of mesentery • Appendicular artery
- 31. Peritoneum in Pelvis • After covers the structures of posterior abdominal wall • Reaches pelvis • First invests sigmoid colon from pelvic wall • Sigmoid mesocolon • Then covers Rectum • Upper third on front & sides • Middle part on front only Tracing the peritoneum anteriorly differs in male & female
- 32. Sigmoid mesocolon • Suspends sigmoid colon • Attached to post abdominal and pelvic walls like inverted V • Apex of V lies on ureter at bifurcation of Lt. com iliac artery • Lt limb – along upper ½ of Lt, Ext iliac • Contents – Superior rectal vessels
- 33. Peritoneum - Pelvis • In male • From rectum to seminal vesicle • Then upper surface of urinary bladder • Forms rectovesical pouch • From apex of UB to inner surface of anterior abdominal wall till umbilicus • In female • From rectum to posterior fornix of vagina • And covers supravaginal cervix, body and fundus • Forms rectouterine pouch (pouch of Douglas) • Then covers anterior surface of body • From body to UB • Forms uterovesical pouch
- 34. Female pelvis • Communicates with extraperitoneal pelvis exteriorly • Through fallopian tubes, uterus and vagina
- 35. Folds in anterior abdominal wall • Median umbilical fold • Remnant of urachus (median umbilical ligaments) • Medial umbilical fold • Remnants of umbilical arteries (medial umbilical ligaments) • Lateral umbilical fold • Inferior epigastric vessels
- 36. Fossae of anterior abdominal wall
- 38. Peritoneal cavity - Divisions • Transverse mesocolon divides the peritoneal cavity in to • Supramesocolic space • Also known as subphrenic spaces • Inframesocolic space • Bilateral paracolic & pelvic spaces are also peritoneal spaces
- 39. Supra colic space • Also known as subphrenic spaces • Boundaries • Superiorly • Diaphragm • Inferiorly • Transverse colon • In front • Ant abdominal wall • Behind • Lesser omentum, stomach, greater omentum
- 40. Supracolic compartment • Supracolic compartment contains • Stomach, liver, and spleen • Infracolic compartment contains • Small intestine and ascending & descending colons • Infracolic compartment is divided into • Right and left infracolic spaces by the mesentery of small intestine • Communication occurs between the supracolic and infracolic compartments • Through paracolic gutters
- 41. • Right • Right anterior subphrenic (subdiaphragmatic) • Right posterior subphrenic (hepatorenal or Morrisons pouch) • Right extraperitoneal • Left • Left anterior intraperitoneal / left suprahepatic / subphrenic • Left posterior intraperitoneal / left subhepatic • Left extraperitoneal Supracolic compartment - Spaces
- 42. Right anterior intraperitoneal / subphrenic / suprahepatic • Presents • Right of falciform ligament • Boundaries • In front • Ant abdominal wall & diaphragm • Behind • Superior anterior & right lateral surface of right lobe of liver, superior layer of coronary ligament • Below • Communicates with right posterior intraperitoneal compartment • Above • Diaphragm
- 43. Morrison’s Pouch / Hepatorenal pouch / Rt subhepatic pouch • Right posterior subphrenic space • Most dependent part of peritoneal cavity in upper abdomen • Boundaries • In Front • Inferior surface of rt. lobe of liver and Gall bladder • Behind • Anterior surface of rt. kidney & rt. supra renal gland • Rt. Colic flexure & 2nd part of duodenum • Above • Inf layer of coronary ligament • Below • Communicate with infracolic part of peritoneal cavity • Left • Communicate with omental bursa • Right • Limited by diaphragm
- 44. Morrison’s Pouch Hepatorenal pouch Rt subhepatic pouch • Most dependent part of abdomen proper • Commonest site of subphrenic abscess • From • Perforated peptic ulcer of stomach & duodenum
- 45. Right extraperitoneal space • Bare area of liver presents • Liver directly related to diaphragm • Boundaries • Left • IVC • Right • Rt. triangular ligament • Above • Superior layer of coronary ligament • Below • Inferior layer of coronary ligament • Clinical anatomy • Common site for • Amoebic liver abscess
- 46. Left anterior intraperitoneal • Lies on left of falciform ligament • Boundaries • In front • Ant abdominal wall • Behind • Lt triangular ligament • Lt. lobe of liver • Stomach & spleen
- 47. Left posterior intraperitoneal • It is lesser sac
- 48. Lesser Sac • Position • Behind the lesser omentum and stomach walls
- 49. Lesser sac • Boundaries • Superior • Peritoneum which covers the caudate lobe of liver and diaphragm • Anterior • Lesser omentum • Peritoneum of posterior wall of stomach • And anterior two layers of greater omentum • Posterior • Posterior two layers of greater omentum • Transverse colon & transverse mesocolon • Peritoneum covering pancreas, left kidney and suprarenalgland • Inferior • Continuity of anterior and posterior two layers of greater omentum
- 50. Lesser Sac • Right border • From above downwards • Deficient above • Epiploic foramen • Peritoneum covering • Posterior surface of proximal part of duodenum to the head of pancreas • Left border • From above downwards • Gastrophrenic ligament • Gastrosplenic and lienorenal ligament • Left border of greater omentum
- 51. Parts of lesser sac • Body • Lies behind lesser omentum & stomach • Superior recess • Lies behind caudate lobe of liver • Splenic recess • Between gastrosplenic and lienorenal ligament • Inferior recess • Lies between the folds of greater omentum
- 52. Epiploic foramen • Communication between • Lesser and greater sac • Location • T -12 vertebra level • Boundaries • Anteriorly • Free margin of lesser omentum • Contains • Front right to left • Bile duct & hepatic artery • Behind • Portal vein • Posteriorly • IVC (covered by peritoneum) • Superiorly • Caudate process of liver • Inferiorly • 1st part of duodenum
- 53. Epiploic foramen Boundaries • Anteriorly • Free margin of lesser omentum • Contains • Front right to left • Bile duct & hepatic artery • Behind • Portal vein • Posteriorly • IVC (covered by peritoneum) • Superiorly • Caudate process of liver • Inferiorly • 1st part of duodenum
- 54. Applied anatomy • Internal abdominal hernia • Occasionally a loop of intestine may enter into lesser sac • Through epiploic foramen • None of the boundaries can be incised to reduce the hernia • Pushing the herniated loop out of lesser sac by inserting the index finger into it through ant. 2 layers of greater omentum
- 55. Infracolic Compartments • Lies below the transverse colon & mesocolon and behind the greater omentum • Divided into w by root of mesentery • Right infracolic Compartment • Left infracolic Compartment
- 56. Right infracolic compartmet • Boundaries • Above • Transvers colon & mesocolon • On right • Ascending colon • On left • Root of Mesentery • Below • Closed
- 57. Left infracolic compartmet • Lies left of root of mesentery • Boundaries • In front • Anterior abdominal wall • Above • Transverse mesocolon • Below • Open with pelvis • On right • Root of mesentery • On left • Descending colon
- 58. Paracolic gutters • Longitudinal channels • Lined by peritoneum • Lies along the sides of ascending & descending colons • Right & left paracolic gutters • Right paracolic gutter • Lies lateral to ascending colon • Communication • Beween Hepato-renal pouch (above) & pelvis (below) • Left paracolic gutter • Lies lateral to descending colon • Above it is separated from • Spleen & lienorenal space by Phrenico-colic ligament • Below it is communicated with pelvis •
- 59. Rectouterine Pouch (Pouch of Douglas) • Boundaries: • Anteriorly: uterus and posterior fornix of vagina • Posteriorly: rectum • Inferiorly (floor): rectovaginal fold of peritoneum • Clinical anatomy • Most dependent part of peritoneal cavity • Pus collected here • Can be drained through rectum or posterior fornix of vagina
- 60. Applied anatomy • Ascites • Excessive accumulation of peritoneal fluid in peritoneal cavity • Commonly due to • Cirrhosis • TB & Malignancy • Paracentesis • Draining fluid • Peritonitis • Infection & inflammation of peritoneum • May result in fatal • Minimize the damage of peritoneum